## Imaging Hallmark of Perforated Diverticulitis **Key Point:** The **thin linear lucency (air tracking) through the colonic wall into the peritoneal cavity** is the pathognomonic CT sign of **diverticular perforation**. This finding, combined with a localized abscess and peritoneal inflammation, confirms perforation. ### CT Imaging Signs of Diverticular Perforation **High-Yield:** The **perforation tract sign** (or **diverticular fistula sign**) is a linear air collection extending from the diverticulum through the bowel wall into the adjacent peritoneal cavity or abscess. This is the single most specific imaging indicator of perforation in diverticulitis. | Imaging Finding | Meaning | Significance | |---|---|---| | **Thin linear air track through wall** | Perforation tract | Diagnostic of perforation | | **Localized pericolic abscess (3–5 cm)** | Contained perforation | Hinchey Stage II | | **Large peritoneal abscess (>5 cm)** | Larger collection | Hinchey Stage III | | **Free air without loculation** | Uncontained perforation | Hinchey Stage IV (generalized peritonitis) | | **Sigmoid wall thickening + fat stranding** | Acute inflammation | Supports acute diverticulitis | | **Diverticula with air inside** | Pneumodiverticulosis | May indicate perforation or fistula | **Clinical Pearl:** Perforated diverticulitis is **more common in the sigmoid colon** (90% of cases) because of the taeniae coli and increased intraluminal pressure in this region. ### Hinchey Staging of Diverticulitis (CT-based) ```mermaid flowchart TD A[Acute diverticulitis]:::outcome --> B{Imaging findings?}:::decision B -->|Inflammation only| C[Hinchey Stage I<br/>Uncomplicated]:::action B -->|Pericolic abscess| D[Hinchey Stage II<br/>Localized perforation]:::action B -->|Larger abscess or fistula| E[Hinchey Stage III<br/>Purulent peritonitis]:::action B -->|Free air, generalized| F[Hinchey Stage IV<br/>Fecal peritonitis]:::urgent D --> G{Abscess size?}:::decision G -->|< 4 cm| H[Conservative + antibiotics]:::action G -->|> 4 cm| I[Percutaneous drainage]:::action F --> J[Emergency colostomy]:::urgent ``` **Mnemonic:** **PERFORATED DIVERTICULITIS** — Perforation tract (air through wall), Extraluminal air, Rupture into peritoneum, Fistula formation, Obstruction, Rupture stage, Abscess (localized), Tract sign on CT, Extraluminal collection, Diverticula visible, Inflammation in sigmoid, Vascular compromise, Elevated WBC, Rigidity, Tenderness, Imaging (CT), Tract sign (linear air), Inflammation, Tract, Localized collection, Inflammation, Tract sign, Imaging (CT) ### Differentiation: Uncomplicated vs. Perforated Diverticulitis | Feature | Uncomplicated | Perforated | |---------|---------------|----------| | **Wall thickening** | Mild (< 5 mm) | Moderate to severe | | **Fat stranding** | Minimal pericolic | Extensive pericolonic | | **Abscess** | None | Present (localized or large) | | **Air tracking** | None | Linear tract through wall | | **Free air** | Absent | May be present | | **Clinical presentation** | Mild–moderate pain | Acute peritonitis | | **Management** | Antibiotics ± bowel rest | Drainage ± surgery | **Warning:** Do NOT confuse **pneumodiverticulosis** (air within diverticula) with **perforation**. Pneumodiverticulosis can occur with fistulization (e.g., colovesical fistula) but is not always indicative of acute perforation. The **linear tract through the wall** is the key discriminator. ### Management Pathway 1. **Uncomplicated diverticulitis (Stage I):** Outpatient antibiotics, clear liquid diet, follow-up CT in 6 weeks 2. **Localized abscess (Stage II, < 4 cm):** Antibiotics + bowel rest; if > 4 cm, percutaneous drainage + antibiotics 3. **Purulent peritonitis (Stage III):** Percutaneous drainage + antibiotics; surgery if fails or unstable 4. **Fecal peritonitis (Stage IV):** **Emergency surgical intervention** (Hartmann procedure with colostomy) **Clinical Pearl:** The presence of a **perforation tract on CT** (linear air through the wall) mandates close follow-up and consideration of surgical intervention, even if the abscess is small and the patient is initially stable on antibiotics. ## Answer Justification The **thin linear lucency tracking through the sigmoid wall** is the pathognomonic CT sign of diverticular perforation. Combined with a localized abscess, fever, and peritonitis, this is diagnostic of **perforated diverticulitis with localized abscess (Hinchey Stage II)**. This patient requires antibiotics, percutaneous drainage of the abscess (if > 4 cm), and close monitoring for progression to generalized peritonitis. [cite:Robbins 10e Ch 17; Harrison 21e Ch 297] 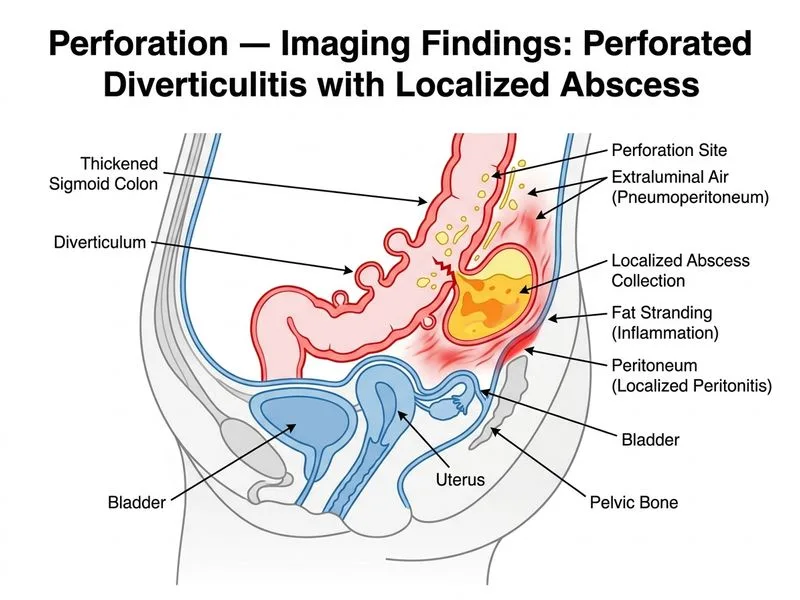
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.