## Investigation of Choice for Complicated Diverticulitis with Suspected Perforation **Key Point:** CT abdomen and pelvis with IV contrast (portal venous phase) is the imaging modality of choice for suspected perforated diverticulitis because it has the highest sensitivity and specificity to detect perforation, grade severity (Hinchey classification), identify complications (abscess, fistula), and guide percutaneous intervention or surgical planning. ### Why CT is Superior in This Scenario 1. **High Sensitivity for Perforation**: Detects free air, pericolonic abscess, and contained perforation even when erect CXR is negative. 2. **Hinchey Grading**: Allows accurate staging of diverticulitis severity: - **Stage I**: Pericolic inflammation/abscess < 4 cm - **Stage II**: Pericolic or distant abscess > 4 cm - **Stage III**: Purulent peritonitis (free pus without loculation) - **Stage IV**: Fecal peritonitis (free fecal material) 3. **Guides Management**: Determines need for percutaneous drainage (Stage II–III) vs. immediate surgery (Stage IV). 4. **Identifies Complications**: Detects fistulas, adjacent organ involvement, and septic thrombophlebitis. ### CT Findings in Perforated Diverticulitis | Finding | Significance | | --- | --- | | **Free air** | Indicates perforation; may be localized or diffuse | | **Pericolonic abscess** | Contained perforation; amenable to percutaneous drainage | | **Thickened colonic wall** | Diverticulitis; degree correlates with severity | | **Pericolonic fat stranding** | Inflammation; extent indicates severity | | **Fecal material in abscess** | Suggests fecal peritonitis (Stage IV) | | **Fistula tract** | Colovesical, colovaginal, or coloenteric fistula | **High-Yield:** CT with IV contrast in portal venous phase (60–70 seconds post-injection) provides optimal visualization of bowel wall enhancement and pericolonic inflammation. Non-contrast CT has lower sensitivity. ### Role of Other Investigations - **Abdominal Ultrasound**: Limited sensitivity for perforation and abscess characterization; operator-dependent; not reliable in acute setting. - **Barium Enema**: Contraindicated in acute diverticulitis with suspected perforation due to risk of extraperitoneal barium leak and peritonitis. - **MRI Abdomen**: High sensitivity but impractical in acute unstable patients; reserved for chronic complications or when CT is contraindicated. **Clinical Pearl:** In a hemodynamically stable patient with suspected perforated diverticulitis and negative erect CXR, CT is the next investigation of choice. It not only confirms perforation but also guides percutaneous drainage of Stage II–III abscesses, potentially avoiding emergency colostomy and allowing elective resection after resolution. **Mnemonic: HINCHEY** — Helps grade diverticulitis severity: - **H**igh-grade (Stage IV: fecal peritonitis) → emergency surgery - **I**nflammation alone (Stage I) → antibiotics - **N**eighboring abscess (Stage II) → percutaneous drainage + antibiotics - **C**ontained perforation (Stage III: purulent peritonitis) → drainage ± surgery - **H**igh-risk patients → consider early elective resection - **E**xtensive involvement → surgical planning - **Y**ield to imaging for staging **Tip:** If patient is hemodynamically unstable or septic, proceed to emergency surgery without waiting for CT if clinical and laboratory findings are highly suggestive. CT is for diagnostic confirmation and treatment planning in stable patients. 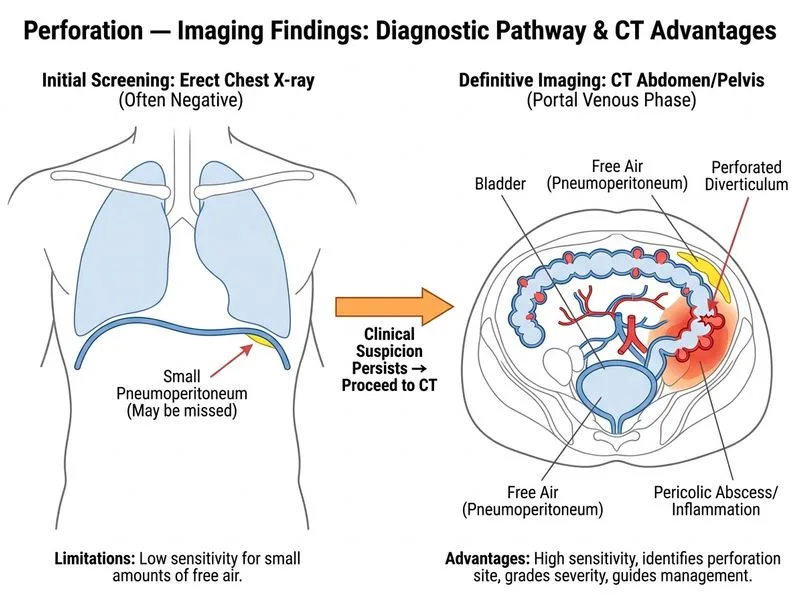
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.