## Clinical Diagnosis **Key Point:** The sudden onset of the **6 Ps** (Pain, Pallor, Pulselessness, Paresthesia, Paralysis, Perishing cold) in one leg with absent femoral pulse and no flow on Doppler indicates **acute arterial occlusion**. ## Differential Diagnosis of Acute Limb Ischemia | Feature | Acute Thrombosis | Acute Embolism | Dissection | AAA Rupture | |---------|------------------|----------------|-----------|-------------| | **Onset** | Sudden (hours) | Sudden (minutes) | Sudden | Sudden (catastrophic) | | **History** | Pre-existing PAD, claudication | AF, recent MI, cardiac source | Hypertension, Marfan syndrome | AAA, smoking, age >70 | | **Pulse** | Absent distally; proximal pulse may be present | Absent distally | Asymmetric pulses bilaterally | Absent bilaterally (shock) | | **Imaging** | Doppler: no flow in artery; CTA: thrombus in atherosclerotic vessel | Doppler: embolic occlusion | CTA: intimal flap, false lumen | CTA: rupture, hematoma | | **Systemic signs** | Localized to limb | Localized to limb | Chest/back pain, BP differential | Shock, hypotension, back pain | ## Why This Is Acute Thrombosis 1. **Unilateral presentation:** Absent left femoral pulse with patent right femoral pulse excludes aortic pathology (dissection, rupture). 2. **Localized ischemia:** Mottling and cyanosis confined to the left leg; no systemic shock or back pain. 3. **Doppler finding:** No flow in the superficial femoral artery indicates thrombosis, not embolism (which typically lodges at bifurcations). 4. **Risk factors:** Age, hypertension, hyperlipidemia—classic for atherosclerotic PAD with superimposed thrombosis. **High-Yield:** Acute thrombosis occurs when a **pre-existing atherosclerotic stenosis** (often asymptomatic or causing mild claudication) suddenly occludes due to: - Plaque rupture and thrombus formation - Reduced flow state (dehydration, heart failure, sepsis) - Hypercoagulability (malignancy, thrombophilia) ## Management of Acute Limb Ischemia ```mermaid flowchart TD A[Acute Limb Ischemia]:::outcome --> B{Viable limb?}:::decision B -->|Yes: No sensory loss, motor intact| C[Urgent revascularization]:::action C --> D[Angiography ± Thrombolysis/Thrombectomy]:::action B -->|Marginally viable: Sensory loss, weak motor| E[Revascularization + monitoring]:::action B -->|Non-viable: Sensory loss, paralysis, muscle rigidity| F[Amputation]:::urgent D --> G[Restore perfusion]:::outcome E --> H[Reassess at 6-12 hours]:::decision ``` **Clinical Pearl:** The **Rutherford Classification** stratifies acute limb ischemia: - **Stage I (Viable):** No sensory loss, no muscle weakness - **Stage II (Marginally viable):** Sensory loss in toes, weak plantarflexion - **Stage III (Irreversible):** Muscle rigidity, sensory loss, paralysis → amputation **Key Point:** Time is critical—revascularization must occur within **6–8 hours** to prevent irreversible tissue damage. This patient requires **urgent angiography with catheter-directed thrombolysis or mechanical thrombectomy**. [cite:Harrison 21e Ch 297; Norgren et al. TASC II] 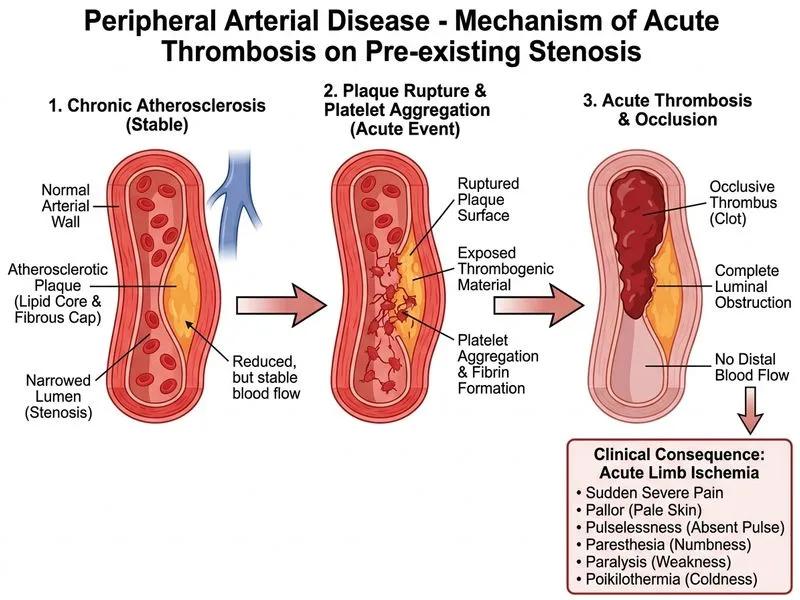
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.