## Distinguishing Intermittent Claudication from Critical Limb Ischemia **Key Point:** The hallmark discriminator between intermittent claudication and critical limb ischemia (CLI) is the **presence or absence of rest pain and tissue loss**. Claudication pain is reproducible, exercise-induced, and completely resolves with rest; CLI pain occurs at rest and does not fully resolve. ### Clinical Features Comparison | Feature | Intermittent Claudication | Critical Limb Ischemia | |---------|---------------------------|------------------------| | **Pain timing** | Only during exercise | At rest, especially nocturnal | | **Pain relief** | Complete resolution within 10 min of rest | Persistent, may require opioids | | **Tissue involvement** | Intact skin, no ulceration | Ulcers, gangrene, tissue loss | | **ABI range** | 0.4–0.9 | <0.4 | | **Prognosis** | ~5% progress to CLI per year | Limb-threatening; requires intervention | | **Collaterals** | Often present | May be absent or inadequate | **High-Yield:** The **exercise-induced, rest-relieved pain** is the single most reliable bedside discriminator. A patient who reports pain that does NOT resolve with rest has crossed into CLI territory and requires urgent intervention. **Clinical Pearl:** Ask the patient: "Does your leg pain wake you up at night?" or "Does it hurt when your leg is elevated?" Affirmative answers suggest CLI, not simple claudication. **Warning:** Do not rely solely on ABI or imaging stenosis percentage. A patient with severe stenosis (>70%) may still have claudication if collaterals are adequate; conversely, a patient with moderate stenosis may have CLI if collateral flow is poor. ### Why Option 0 is Correct Option 0 captures the **pathognomonic feature of claudication**: pain that is strictly exercise-dependent and resolves completely with rest. This reproducibility and reversibility distinguish it from the persistent, rest pain of CLI. 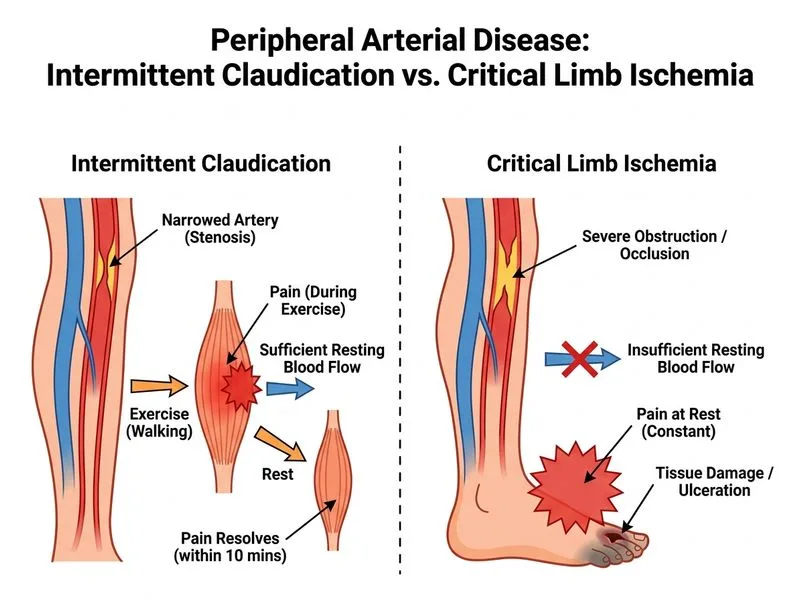
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.