## Clinical Assessment of Claudication Severity **Key Point:** This patient has intermittent claudication (Fontaine Stage II) with significant haemodynamic compromise (ABI 0.58). Management follows a stepwise approach based on symptom severity and functional impact. ### Fontaine Classification of PAD | Stage | Clinical Features | ABI Range | |-------|-------------------|----------| | I | Asymptomatic | < 0.9 | | II | Intermittent claudication | 0.4–0.9 | | III | Rest pain | 0.2–0.4 | | IV | Tissue loss (ulcer/gangrene) | < 0.2 | **High-Yield:** Claudication alone does NOT mandate intervention. First-line management is **conservative**: smoking cessation, supervised exercise, and optimised medical therapy (antiplatelet + statin). Intervention is reserved for: - Failure of conservative therapy (persistent symptoms limiting quality of life) - Lifestyle-limiting claudication unresponsive to 3–6 months of exercise - Critical limb ischaemia (rest pain, tissue loss) ### Why Conservative Management First? 1. **Natural history:** ~50% of claudicants improve or stabilise with exercise alone 2. **Symptom improvement:** Supervised exercise increases walking distance by 50–100% in 3 months 3. **Cardiovascular risk reduction:** Aggressive lipid and blood pressure control reduce MI/stroke risk more than revascularisation 4. **Durability:** PTA/stent patency rates are lower in SFA disease; reserve for failed conservative therapy **Clinical Pearl:** The SFA is the most common site of claudication in the lower limb. Although 90% stenosis is significant, the presence of collateral circulation (evidenced by palpable femoral pulse) means the limb is viable and claudication is the only symptom. ### Indications for Intervention in Claudication - Lifestyle-limiting symptoms despite 3–6 months supervised exercise - High-risk occupation (e.g. postman, manual labourer) - Anatomically favourable lesions (short, non-calcified SFA stenosis) - Patient preference after counselling on risks/benefits **Warning:** Immediate PTA/stenting in stable claudication increases cost, radiation exposure, and stent thrombosis risk without proven long-term benefit over conservative therapy. ### Optimised Medical Therapy - **Antiplatelet:** Aspirin 75 mg (already on board) - **Statin:** Atorvastatin 40 mg (adequate; no need to escalate for claudication alone) - **ACE inhibitor:** Consider if hypertensive or diabetic (cardioprotective) - **Cilostazol:** 100 mg BD can improve walking distance by ~50 m; consider if exercise plateau reached - **Smoking cessation:** Mandatory; improves prognosis dramatically **Mnemonic — SAFE PAD:** **S**moking cessation, **A**ntiplatelet, **F**itness (supervised exercise), **E**xercise; **P**ancreatic risk factors (lipids, BP, glucose), **A**ngiotensin inhibitor, **D**iabetes control. 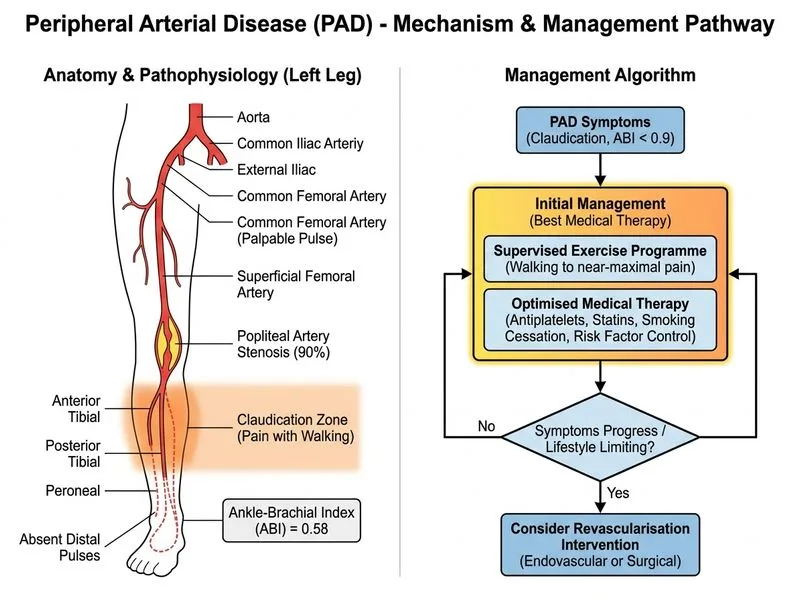
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.