## Acute Lower Limb Ischemia: Differential Diagnosis This patient presents with **acute limb-threatening ischemia** (pain, pallor, pulselessness, paresthesia) with acute popliteal artery occlusion. The clinical context — sudden onset, preserved femoral pulses, and minimal/no visible thrombus on CT angiography — points toward a specific etiology. ### Differential Diagnosis of Acute Popliteal Artery Occlusion | Feature | Acute Thrombosis | Acute Embolism | Entrapment | Dissection | |---------|------------------|----------------|------------|----------| | **Onset** | Acute or gradual | Sudden (minutes–hours) | Chronic claudication | Acute/subacute | | **Prior claudication** | Often present | Absent | Present (exertional) | Absent | | **Femoral pulses** | May be absent | Present | Present | Present | | **Thrombus on imaging** | Usually visible | Minimal/absent | No occlusion | Intimal flap | | **Cardiac source** | No | Yes (AF, MI, valve) | No | No | | **Age/risk factors** | Older, atherosclerotic | Variable | Young, athletic | Variable | ### Why Acute Embolism Is Most Likely (Option D) 1. **Sudden onset** — 6 hours of acute, severe symptoms is classic for embolic occlusion, which typically produces abrupt ischemia without a prodrome of claudication. 2. **Minimal/no visible thrombus on CT** — emboli are often small, fragmented, or of similar density to flowing blood, making them difficult to visualize as a discrete clot on CT angiography. This is in contrast to in-situ thrombosis, where a thrombus on a background of atherosclerotic plaque is usually identifiable. 3. **Femoral pulses present bilaterally** — indicates the occlusion is distal to the femoral bifurcation, consistent with an embolus lodging at the popliteal level. 4. **No prior claudication** — the absence of exertional leg pain argues against pre-existing significant atherosclerotic disease (Option A), which typically produces a history of claudication before acute-on-chronic occlusion. 5. **Age and comorbidities** — diabetes and CKD are associated with atrial fibrillation and cardiomyopathy, both potent sources of cardiac thrombus. **High-Yield:** In acute limb ischemia, **minimal or no visible thrombus on imaging** in the appropriate clinical context strongly suggests **embolism** rather than in-situ thrombosis of an atherosclerotic plaque. Note that small thrombi or those isodense to blood can occasionally be missed on CT, so the finding should be interpreted alongside the full clinical picture (Harrison's Principles of Internal Medicine, 21e, Ch. 256). ### Why the Other Options Are Less Likely - **Option A (Acute thrombosis of atherosclerotic plaque):** Typically occurs on a background of chronic atherosclerosis with prior claudication; a thrombus is usually visible on CT. The absence of claudication history and minimal thrombus make this less likely. - **Option B (Popliteal artery entrapment syndrome):** Classically affects young, athletic individuals (typically men aged 20–40) due to anomalous muscle or fibrous band compression. A 72-year-old woman with multiple vascular comorbidities is a very atypical demographic; entrapment also usually presents with exertional claudication rather than acute ischemia. - **Option C (Dissection of the popliteal artery):** Popliteal artery dissection is rare and would typically show an intimal flap or double lumen on CT angiography, not simply an absence of thrombus. It is usually associated with trauma or connective tissue disorders. ### Clinical Pearl: The "6 Ps" of Acute Limb Ischemia **Pain, Pallor, Pulselessness, Paresthesia, Poikilothermia, Paralysis** — this patient exhibits the first four. Paralysis indicates irreversible ischemia and is a surgical emergency. ### Next Steps in Management 1. **Immediate IV heparin anticoagulation** — to prevent propagation and recurrent embolism. 2. **Urgent revascularization** — surgical embolectomy (Fogarty catheter) or catheter-directed thrombolysis within 6 hours to salvage the limb. 3. **Cardiology evaluation + echocardiography** — to identify cardiac source (AF, LV thrombus, valvular disease). 4. **Renal precautions** — given CKD (eGFR 35), contrast nephropathy risk must be managed; hydration and minimizing contrast load are essential. [cite: Harrison's Principles of Internal Medicine, 21e, Ch. 256; Norgren et al. TASC II Inter-Society Consensus 2007; Rutherford's Vascular Surgery, 9e] 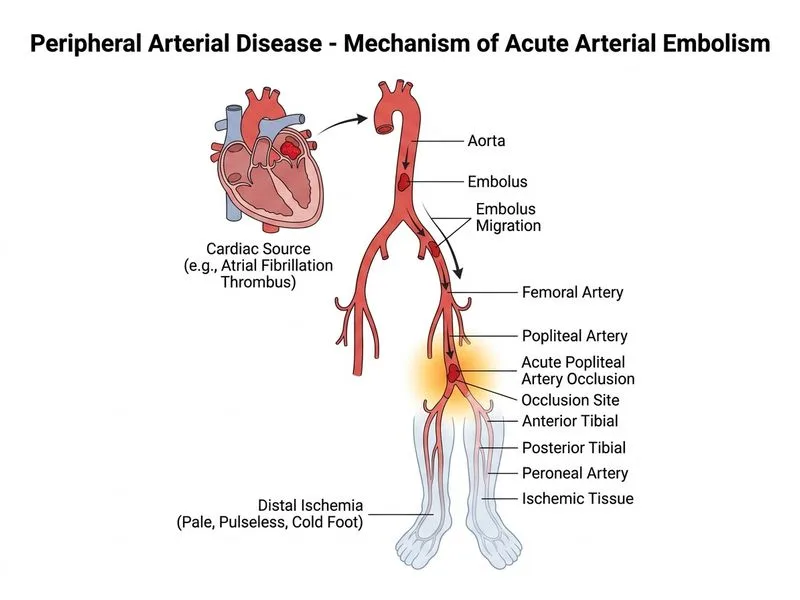
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.