## Clinical Diagnosis: Branchial Cyst / Fistula The presentation is pathognomonic for a **branchial fistula** (second pharyngeal arch derivative), specifically a **second branchial cleft fistula**: - **Location:** Anterior border of sternocleidomastoid, junction of upper and middle thirds - **Tract course:** Extends from skin opening upward to tonsillar fossa (internal opening in pharynx) - **Presentation:** Mucoid discharge, recurrent infections, hearing loss (if associated with middle ear involvement) **High-Yield:** Branchial remnants arise from incomplete obliteration of the pharyngeal pouches and clefts during embryonic development (weeks 5–12). The second arch derivatives are most common (95% of cases). ## Management Approach **Key Point:** Unlike cystic hygromas, branchial fistulas do NOT regress spontaneously. Once diagnosed, **definitive surgical excision is the standard of care**. ### Why Surgery Is Indicated 1. **No spontaneous closure:** Fistulas persist and are prone to recurrent infection 2. **Infection risk:** Mucoid discharge and recurrent infections (as seen here) indicate active tract 3. **Hearing complications:** Recurrent infections can lead to otitis media and conductive hearing loss 4. **Malignancy risk:** Chronic irritation and inflammation increase squamous cell carcinoma risk (rare but documented) ### Surgical Technique **Mnemonic:** **COMPLETE TRACT REMOVAL** — the key to preventing recurrence: - Excision of the entire epithelial-lined tract - Removal of the internal opening at the tonsillar fossa (or pharyngeal wall) - Careful dissection to avoid injury to the hypoglossal, vagus, and accessory nerves - Recurrence rate with complete excision: < 5%; with incomplete excision: 20–40% **Clinical Pearl:** Preoperative imaging (ultrasound or CT/MRI) helps delineate the tract course and plan the surgical approach. Methylene blue injection into the external opening can help identify the internal opening intraoperatively. ## Why Other Options Fail - **Prophylactic antibiotics:** Do not address the underlying anatomical defect; infections will recur - **Observation:** Fistulas do not close spontaneously; infections and complications will persist - **Repeated aspiration:** Temporary measure only; does not eliminate the tract 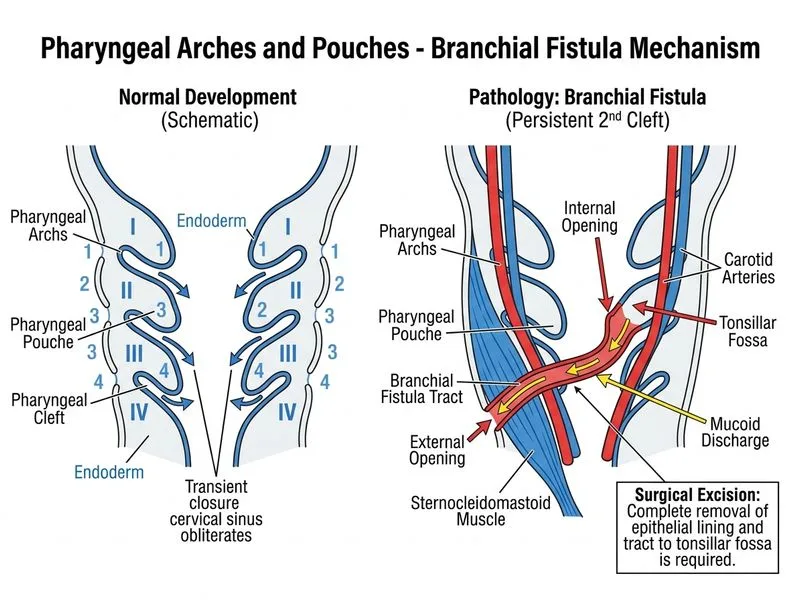
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.