## Biochemical Distinction Between PKU and Tyrosinemia Type I ### Overview Both PKU and tyrosinemia type I are autosomal recessive disorders of phenylalanine and tyrosine metabolism, but they differ in their primary enzymatic defect and biochemical signatures. ### Key Biochemical Differences | Feature | PKU | Tyrosinemia Type I | |---------|-----|-------------------| | **Primary enzyme defect** | Phenylalanine hydroxylase | Fumarylacetoacetase (FAA) | | **Plasma phenylalanine** | ↑↑↑ (>20 mg/dL) | Normal or mildly elevated | | **Plasma tyrosine** | Normal or low | ↑↑ (>1200 μmol/L) | | **Urine succinylacetone** | Absent | Present (pathognomonic) | | **Secondary hypertyrosinemia** | Absent | Present (due to hepatic dysfunction) | | **Hepatic involvement** | Minimal | Severe (cirrhosis, HCC risk) | ### Pathophysiology **PKU:** - Phenylalanine hydroxylase catalyzes: Phenylalanine → Tyrosine - Deficiency → phenylalanine accumulates, tyrosine becomes conditionally essential - Tyrosine is still synthesized from other pathways (minor contribution) **Tyrosinemia Type I:** - Fumarylacetoacetase is the final enzyme in tyrosine catabolism - Deficiency → accumulation of toxic intermediates (maleylacetoacetone, succinylacetone) - Succinylacetone is **pathognomonic** — not found in any other metabolic disorder - Secondary hypertyrosinemia occurs due to hepatic dysfunction and impaired protein synthesis ### Why Succinylacetone is the Best Discriminator **Key Point:** Succinylacetone in urine is virtually diagnostic of tyrosinemia type I and absent in PKU. It is formed from the accumulation of fumarylacetoacetate and maleylacetoacetate when FAA is deficient. **Clinical Pearl:** Succinylacetone is also a potent inhibitor of porphobilinogen synthase, explaining why tyrosinemia type I patients can present with acute porphyria-like crises (abdominal pain, neurological symptoms). **High-Yield:** In newborn screening, if elevated phenylalanine is found: - Measure plasma tyrosine and urine organic acids - Succinylacetone in urine → tyrosinemia type I (requires urgent treatment with nitisinone) - Normal tyrosine + normal urine → PKU (dietary management) ### Why Other Options Are Suboptimal - **Option 0 (elevated Phe, normal/low Tyr):** This is characteristic of PKU, not a discriminator between the two. - **Option 1 (elevated Tyr, normal Phe):** While seen in tyrosinemia type I, it is NOT specific — secondary hypertyrosinemia can occur in any severe liver disease, neonatal tyrosinemia, or other conditions. - **Option 3 (Phe hydroxylase deficiency):** This is the defect in PKU, not in tyrosinemia type I; it is not a discriminator but rather a definition of PKU itself. [cite:Robbins 10e Ch 5] 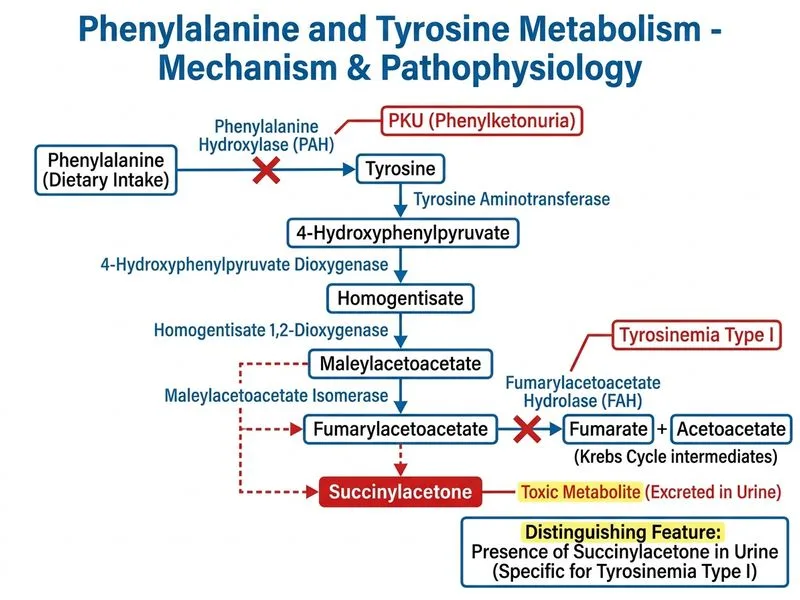
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.