## Clinical Context A 32-year-old male from rural Odisha presents with fever, chills, myalgia, splenomegaly, and ring forms/trophozoites on peripheral blood smear — this is a **confirmed diagnosis of malaria by microscopy**. The question asks for the **most appropriate next step in management**. ## Why Start Treatment Immediately **High-Yield:** Per WHO guidelines and NVBDCP (National Vector Borne Disease Control Programme) India protocols, a **positive blood smear is sufficient to initiate antimalarial therapy** — no additional confirmatory testing (RDT or QBC) is required before starting treatment. Delaying treatment in a confirmed smear-positive patient is inappropriate and potentially dangerous. **Key Point:** In India (including Odisha, a high *P. falciparum* burden state), the standard first-line treatment for **uncomplicated malaria** is: - *P. falciparum*: Artemisinin-based Combination Therapy (ACT) - *P. vivax*: Chloroquine 600 mg base stat (Day 1), followed by 300 mg at 6 hours, then 300 mg on Days 2 and 3 However, among the options given, **Option A (Chloroquine 600 mg base stat)** represents the correct principle of **initiating treatment based on confirmed smear positivity**, which is the most appropriate next step compared to the alternatives. **Clinical Pearl (Park's Textbook of Preventive & Social Medicine, 26th ed.):** The peripheral blood smear (thick and thin) remains the **gold standard** for malaria diagnosis. Once ring forms and trophozoites are identified, treatment should not be delayed for RDT or QBC. RDT is used when microscopy is unavailable, not as a confirmatory step after a positive smear. ## Why Other Options Are Wrong | Option | Reason Incorrect | |---|---| | B) RDT + QBC | Smear is already positive — further confirmation before treatment is unnecessary and delays therapy | | C) IV Artemether immediately | No features of severe/complicated malaria (altered consciousness, high parasitaemia, organ failure) to justify parenteral therapy | | D) Repeat smear in 48 hours | Withholding treatment in a confirmed case is dangerous and unethical | **Mnemonic: SMEAR POSITIVE → TREAT** — A positive peripheral blood smear is diagnostic; initiate appropriate antimalarial therapy without delay. 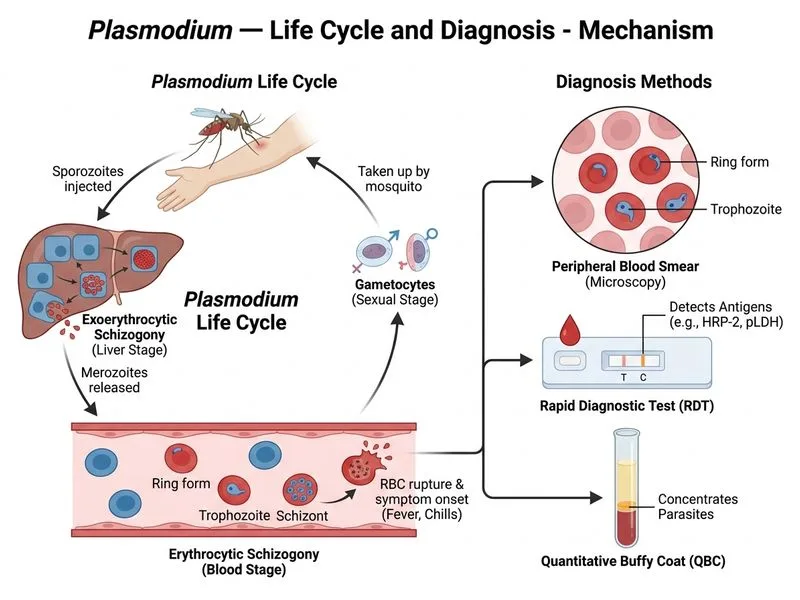
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.