## Investigation of Choice for Pleural Effusion Characterization **Key Point:** Thoracentesis with pleural fluid analysis is the gold standard for determining whether a pleural effusion is transudative or exudative, and for identifying the underlying etiology. ### Why Thoracentesis is Essential Thoracentesis allows: 1. **Light's criteria application** — distinguishes transudative from exudative effusions 2. **Biochemical analysis** — protein, LDH, glucose, cholesterol levels 3. **Cytology** — detection of malignant cells 4. **Microbiology** — culture, Gram stain, AFB for infection 5. **Cell count and differential** — lymphocytic vs. neutrophilic predominance ### Light's Criteria for Exudative Effusion An effusion is exudative if ANY of the following are present: - Pleural fluid protein / serum protein ratio > 0.5 - Pleural fluid LDH / serum LDH ratio > 0.6 - Pleural fluid LDH > 2/3 upper limit of normal serum LDH **High-Yield:** Transudative effusions (congestive heart failure, cirrhosis, nephrotic syndrome) do NOT require thoracentesis unless clinical presentation is atypical. Exudative effusions (malignancy, infection, PE, autoimmune) mandate fluid analysis. ### Clinical Pearl In this case, the 3-week progressive history with pleuritic chest pain suggests an exudative process (malignancy, tuberculosis, or parapneumonic effusion) rather than simple heart failure, making thoracentesis mandatory for diagnosis. **Tip:** Always perform thoracentesis on exudative effusions to guide treatment and identify treatable causes (infection, malignancy, autoimmune disease). 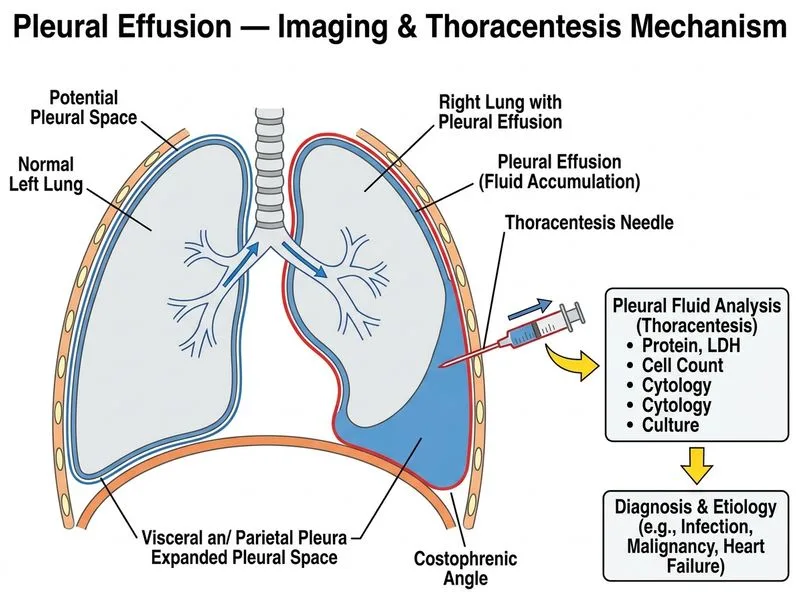
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.