## Clinical Context This patient has cirrhosis with a pleural effusion in a stable clinical state. The imaging characteristics (anechoic on ultrasound, no acute findings on CXR) and clinical stability suggest a transudative effusion secondary to portal hypertension. ## Management Approach for Transudative Effusions **Key Point:** Transudative pleural effusions (typically from cirrhosis, heart failure, or nephrotic syndrome) are managed medically without diagnostic thoracentesis if the clinical context is clear and the patient is stable. **High-Yield:** Light's criteria help distinguish transudative from exudative effusions: - Transudative: LDH ratio <0.6, protein ratio <0.5, pleural LDH <2/3 serum LDH - Exudative: meets ≥1 criterion In this case, the clinical diagnosis of cirrhosis-related effusion is established; thoracentesis is reserved for diagnostic uncertainty or therapeutic benefit. ## Why Diuretics and Sodium Restriction? 1. **Mechanism:** Reduces plasma volume and intravascular hydrostatic pressure, decreasing fluid transudation into the pleural space 2. **Evidence-based:** First-line for cirrhotic pleural effusions [cite:Harrison 21e Ch 297] 3. **Clinical follow-up:** Reassess response to therapy; if refractory, consider TIPS or other interventions **Clinical Pearl:** Refractory pleural effusion in cirrhosis (not responding to diuretics) is an indication for transjugular intrahepatic portosystemic shunt (TIPS) consideration. ## Why NOT the Other Options? Thoracentesis is unnecessary when the diagnosis is clinically clear and the effusion is transudative. CT and antibiotics are not indicated in a stable patient with known cirrhosis and typical imaging. 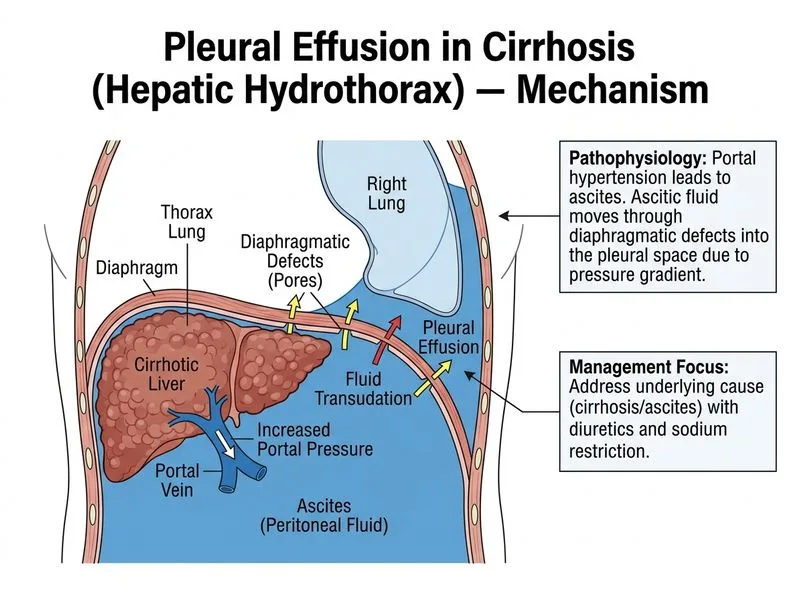
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.