## Diagnosis: Malignant Pleural Effusion (Likely Lung Adenocarcinoma or Metastatic Disease) ### Clinical Presentation & Pleural Fluid Analysis **Key Point:** The combination of **exudative effusion with high LDH (950 IU/L), low cellularity (450 WBC/μL with lymphocytic predominance), negative cultures, and weight loss** strongly suggests **malignant pleural effusion**. ### Pleural Fluid Criteria for Exudate | Criterion | Patient Value | Status | |-----------|---------------|--------| | Protein | 5.1 g/dL | Exudate (>3 g/dL) | | LDH | 950 IU/L | Exudate (>200 IU/L) | | Serum-to-pleural LDH ratio | 1:3 | Exudate (<1:1 ratio) | | Cellularity | 450 WBC/μL | Low (lymphocytic predominance) | | Cultures | Negative | Rules out infection | ### Why the Correct Answer: Pleural Thickening & Nodularity on CT **High-Yield:** The **most characteristic radiological finding in malignant pleural effusion is pleural thickening and nodularity with contrast enhancement on CT chest**, which reflects: 1. **Tumor infiltration of the pleura** — nodules represent metastatic deposits 2. **Pleural fibrosis and inflammation** — reactive to malignant process 3. **Neovascularization** — causes enhancement with IV contrast 4. **High specificity for malignancy** — distinguishes from benign causes (TB, parapneumonic) **Clinical Pearl:** CT-guided pleural biopsy of enhancing nodular thickening has >90% sensitivity for malignant effusion diagnosis, making this the gold standard imaging finding. ### Imaging Features of Malignant vs. Benign Pleural Effusion ```mermaid flowchart TD A[Pleural Effusion on CXR]:::outcome --> B{CT Chest with Contrast}:::decision B -->|Pleural nodules + thickening + enhancement| C[Malignant Effusion]:::outcome B -->|Smooth pleural thickening, no nodules| D[Consider TB or Benign]:::outcome C --> E[Pleural biopsy for confirmation]:::action D --> F[Acid-fast bacilli, culture, TB-LAMP]:::action ``` ### Radiological Features Favoring Malignancy | Finding | Sensitivity | Specificity | Notes | |---------|-------------|-------------|-------| | **Pleural nodules** | 65–75% | 90–95% | Most specific | | **Pleural thickening >1 cm** | 70–80% | 80–85% | Common but less specific | | **Mediastinal lymphadenopathy** | 60–70% | 70–75% | Often present but not diagnostic alone | | **Contrast enhancement** | 75–85% | 85–90% | Indicates neovascularization | **Warning:** Do NOT rely on **mediastinal lymphadenopathy alone** (option B) — while common in malignancy, it is also seen in TB, sarcoidosis, and lymphoma. The **pleural findings** (nodules + thickening) are more specific. ### Why Other Options Are Incorrect - **Option B (Mediastinal lymphadenopathy):** While present in many malignancies, lymphadenopathy alone is not specific for malignant effusion and occurs in TB, sarcoidosis, and other conditions. - **Option C (Bilateral effusions + cardiomegaly):** Suggests congestive heart failure, which would produce a **transudate** (low protein, low LDH), not the exudate seen here. - **Option D (Loculated effusion):** Loculation can occur in any chronic effusion (TB, parapneumonic, malignant) and is not specific for malignancy. **High-Yield:** The **combination of pleural nodules + thickening + enhancement on CT is the most specific radiological sign of malignant pleural disease** and should prompt pleural biopsy. [cite:Harrison 21e Ch 297; Robbins 10e Ch 15] 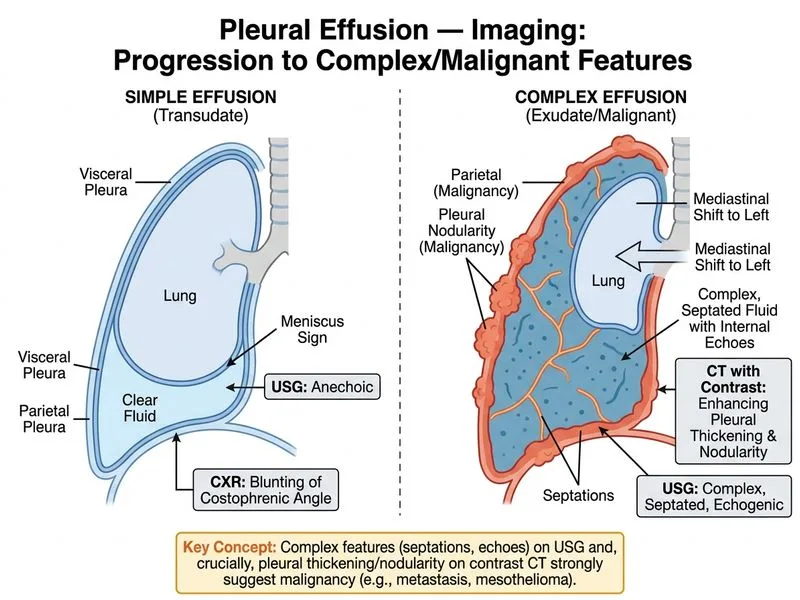
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.