## Imaging Differentiation of Tuberculous Pleural Effusion ### Clinical Context This patient has tuberculous pleuritis, evidenced by: - AFB-positive pleural fluid - Exudative effusion (protein 4.2 g/dL, LDH 450 IU/L) - Low glucose (35 mg/dL) and low pH (7.1) — classic for TB - Anechoic appearance on ultrasound (no loculation) ### Key Imaging Distinction **Key Point:** Pleural thickening and calcification are hallmark chronic imaging findings of tuberculous pleuritis and are NOT seen in acute parapneumonic effusions. Parapneumonic effusions (uncomplicated or simple) are: - Typically anechoic or minimally echogenic on ultrasound - Layering on lateral decubitus films (non-specific) - Associated with adjacent pneumonia on imaging - Resolve with antibiotic therapy without residual pleural changes Tuberculous pleuritis, especially with chronicity, shows: 1. **Pleural thickening** (>3 mm) — develops over weeks to months 2. **Calcification** — rare but highly specific when present 3. **Fibrosis** — may lead to pleural restriction 4. **Adhesions** — may cause loculation ### Why Each Distractor Is Wrong | Option | Why It's Wrong | |--------|---------------| | **Anechoic appearance on ultrasound** | Both TB and parapneumonic effusions can be anechoic; this is NOT differentiating. Anechoic = simple fluid without debris or loculation. | | **Layering on lateral decubitus radiograph** | Layering (gravity-dependent spreading of fluid) occurs in ANY free-flowing effusion — TB, parapneumonic, malignant, etc. Non-specific finding. | | **Unilateral distribution with ipsilateral hilar lymphadenopathy** | While TB commonly presents with hilar lymphadenopathy, this is a clinical-radiological pattern, NOT an imaging feature that differentiates the effusion itself. Parapneumonic effusions can also be unilateral. | ### High-Yield Imaging Pearls **High-Yield:** Pleural calcification is rare (~5% of TB cases) but is virtually pathognomonic when present. Pleural thickening (>3 mm on CT) is more common and develops as TB pleuritis becomes chronic. **Clinical Pearl:** In endemic TB regions, a young patient with exudative effusion, low glucose, and AFB positivity should be assumed tuberculous until proven otherwise. Imaging of pleural thickening/calcification confirms chronicity and supports TB diagnosis. **Mnemonic:** **THICK-TB** — Thickening, Hilar adenopathy, Ipsilateral, Calcification, Kyphosis (spinal TB) — chronic TB pleural signs. ### Differential Imaging Summary ```mermaid flowchart TD A[Pleural Effusion on CXR]:::outcome --> B{Pleural thickening or calcification on CT?}:::decision B -->|Yes| C[Suggestive of TB or chronic process]:::outcome B -->|No| D{Fluid characteristics on ultrasound?}:::decision D -->|Anechoic, free-flowing| E[Could be TB, parapneumonic, or other]:::outcome D -->|Echogenic, septated| F[Suggests complicated parapneumonic or empyema]:::outcome E --> G{Clinical context: AFB, low glucose?}:::decision G -->|Yes| H[TB pleuritis most likely]:::outcome G -->|No| I[Parapneumonic or other etiology]:::outcome ``` ## Summary While pleural fluid analysis (AFB, glucose, pH, LDH) is diagnostic, **pleural thickening and calcification on high-resolution CT are the most reliable imaging findings to differentiate tuberculous pleuritis from parapneumonic effusion**. These findings reflect chronic inflammation and fibrosis specific to TB and are absent in acute parapneumonic effusions. 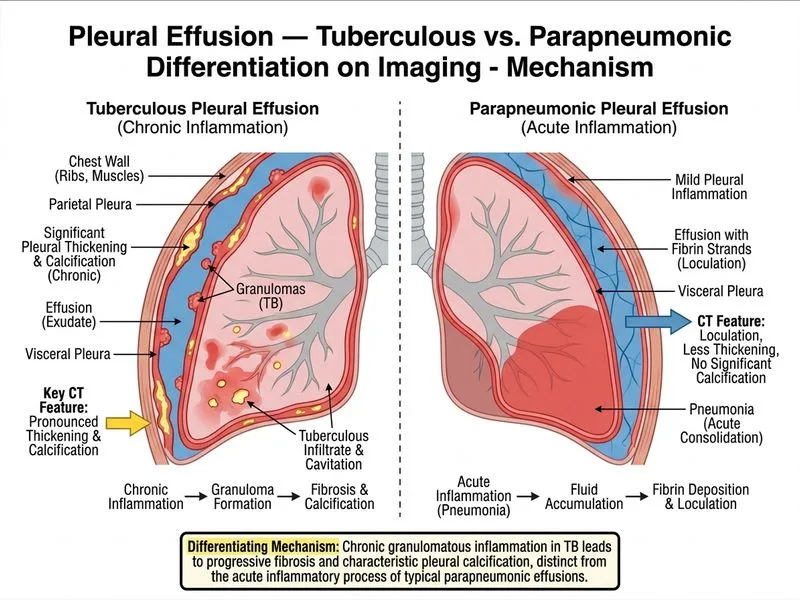
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.