## Management of Pneumothorax Based on Radiological Size and Clinical Stability ### Classification of Pneumothorax by Radiological Size **Key Point:** Pneumothorax management is stratified by radiological size (measured as the distance between the visceral pleural line and the chest wall at the level of the hilum) and clinical stability. A 2 cm pneumothorax in a hemodynamically stable patient is classified as **small** and is managed conservatively. ### Size-Based Classification and Management | Pneumothorax Size | Radiological Criterion | Clinical Stability | Initial Management | Follow-up | |---|---|---|---|---| | **Small** | <2 cm (or <20% hemithorax) | Stable vitals, SpO₂ ≥90% | Observation ± supplemental O₂ | Repeat CXR at 4–6 hrs | | **Large** | ≥2 cm (or ≥20% hemithorax) | Stable | Observation + high-flow O₂ or chest tube | Repeat CXR at 2–4 hrs | | **Large + Symptoms** | ≥2 cm | Dyspneic, tachypneic | Chest tube insertion | Daily CXR until resolved | | **Tension** | Any size | Hemodynamic instability, tracheal shift | **Needle decompression** (14G needle) → chest tube | Immediate intervention | **High-Yield:** A 2 cm pneumothorax is at the **borderline** between small and large. However, this patient is hemodynamically stable (HR normal range implied, SpO₂ 94%, RR 22 — mildly elevated but not critical). Conservative management with observation and supplemental oxygen is appropriate. ### Rationale for Conservative Management in This Case 1. **Radiological size**: 2 cm is borderline; some guidelines classify this as small-to-moderate. 2. **Clinical stability**: Hemodynamically stable, no signs of tension (no tracheal shift mentioned, no hypotension). 3. **Oxygen therapy rationale**: High-flow O₂ (FiO₂ 0.8–1.0) creates a gradient favoring nitrogen reabsorption from the pleural space, accelerating pneumothorax resolution (4–6 fold faster than room air). 4. **Serial imaging**: Repeat CXR at 4–6 hours assesses progression; if size increases or patient deteriorates, chest tube is inserted. ### When to Escalate to Chest Tube ```mermaid flowchart TD A[Pneumothorax diagnosed]:::outcome --> B{Clinical stability?}:::decision B -->|Hemodynamic instability, tracheal shift| C[Tension pneumothorax]:::urgent C --> D[Needle decompression 14G needle 2nd ICS midclavicular]:::action D --> E[Chest tube insertion]:::action B -->|Stable| F{Size and symptoms?}:::decision F -->|Small <2cm, asymptomatic| G[Observation + O₂]:::action F -->|Large ≥2cm or dyspneic| H[Observation + high-flow O₂]:::action G --> I[Repeat CXR 4-6 hrs]:::action H --> J[Repeat CXR 2-4 hrs]:::action I --> K{Progression?}:::decision J --> K K -->|Yes| L[Chest tube]:::action K -->|No| M[Continue observation]:::action L --> N[Daily CXR until resolved]:::action ``` **Clinical Pearl:** In cystic fibrosis, pneumothorax is a common complication due to apical bullae rupture. Recurrent pneumothorax may warrant pleurodesis or VATS pleurectomy, but initial management follows the same size-based algorithm. **Tip:** Memorize the 2 cm threshold — it is the key decision point on NEET PG exams. Below 2 cm = observe; at or above 2 cm with symptoms = consider chest tube. [cite:British Thoracic Society Pneumothorax Guidelines 2010; Harrison 21e Ch 249] 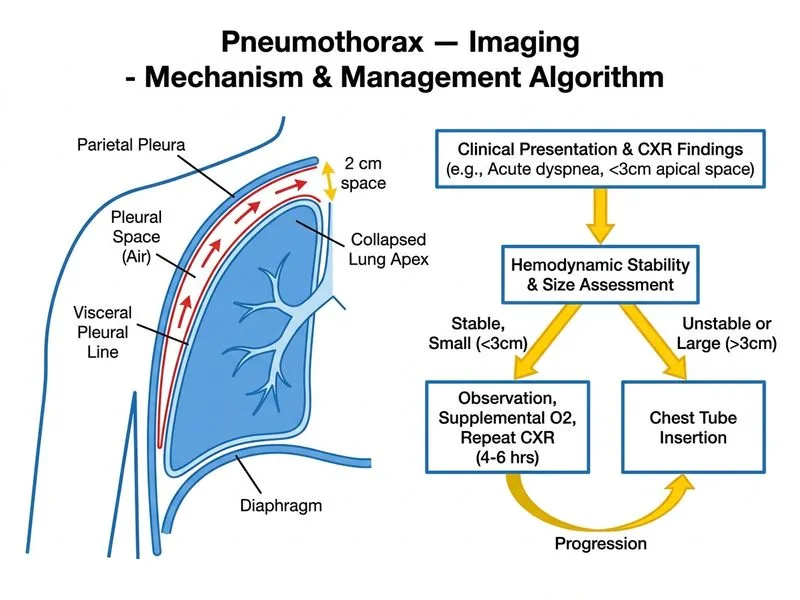
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.