## Imaging Modalities for Occult Pneumothorax Detection ### Sensitivity Comparison Across Modalities | Modality | Sensitivity for Small PTX | Sensitivity for Bilateral PTX | Advantages | Limitations | |----------|---------------------------|-------------------------------|-----------|-------------| | **Upright CXR (PA/Lateral)** | 60–90% | Moderate (may miss small contralateral) | Readily available, low cost | Limited for small PTX, poor for supine patients | | **Expiration CXR** | Improved vs. inspiration | Better than inspiration alone | Increases PTX visibility | Still misses ~10–15% of small PTX | | **Decubitus CXR** | 70–85% | Moderate | Useful for supine patients | Less sensitive than CT | | **High-resolution CT (HRCT)** | **95–100%** | **95–100%** | **Gold standard; detects 1–2 mm PTX** | Higher radiation dose; not first-line for stable patients | | **Ultrasound (US)** | 86–98% (operator-dependent) | Variable | Radiation-free; bedside; real-time | Operator-dependent; cannot quantify size accurately | ### Why HRCT is Superior for Bilateral Pneumothorax **High-Yield:** High-resolution CT with **thin-section slices (1–2 mm)** in both **inspiration and expiration** can detect pneumothorax as small as 1–2 mm, making it the gold standard for: - Occult (clinically suspected but radiographically occult) pneumothorax - Small bilateral pneumothorax - Pneumothorax in supine or obese patients - Assessment of underlying lung disease (bullae, blebs) **Key Point:** CT is superior because: 1. **No summation artifact** — unlike 2D radiographs, CT provides cross-sectional imaging 2. **Detects tiny air collections** — even 1–2 mm of air is visible 3. **Bilateral assessment** — entire thorax is imaged simultaneously 4. **Characterizes underlying lung** — can identify COPD, bullae, or fibrosis predisposing to recurrence ### Clinical Decision-Making Algorithm ```mermaid flowchart TD A[Suspected pneumothorax]:::outcome --> B{Hemodynamically stable?}:::decision B -->|No| C[Tension PTX: needle decompression + CXR]:::urgent B -->|Yes| D[Upright PA + lateral CXR]:::action D --> E{PTX confirmed?}:::decision E -->|Yes, large| F[Assess for intervention]:::action E -->|No, but high clinical suspicion| G[Expiration CXR or CT]:::action E -->|Yes, bilateral concern| H[HRCT chest ± expiration]:::action G --> I{PTX found?}:::decision I -->|Yes| J[Manage accordingly]:::outcome I -->|No| K[Alternative diagnosis]:::outcome H --> L[Bilateral assessment complete]:::outcome ``` ### Why Other Options Are Suboptimal **Clinical Pearl:** Expiration films increase the **relative** size of pneumothorax (lung volume decreases, PTX volume stays constant), improving visibility on radiographs. However, even with expiration films, sensitivity for small bilateral PTX remains 85–90%, missing ~10–15% of cases. CT is definitively superior. **Mnemonic: "CT Beats All" for Occult PTX** - **C**ross-sectional imaging - **T**hin slices detect 1–2 mm air - **B**ilateral assessment in one study - **E**xcels in supine/obese patients - **A**ccurate for underlying lung disease - **T**rue gold standard - **S**ensitivity >95% **Tip:** In a stable patient with clinical suspicion of bilateral pneumothorax, HRCT is justified because it: - Definitively rules in/out contralateral PTX - Characterizes underlying COPD severity - Guides management (observation vs. intervention) - Prevents missed diagnosis and complications 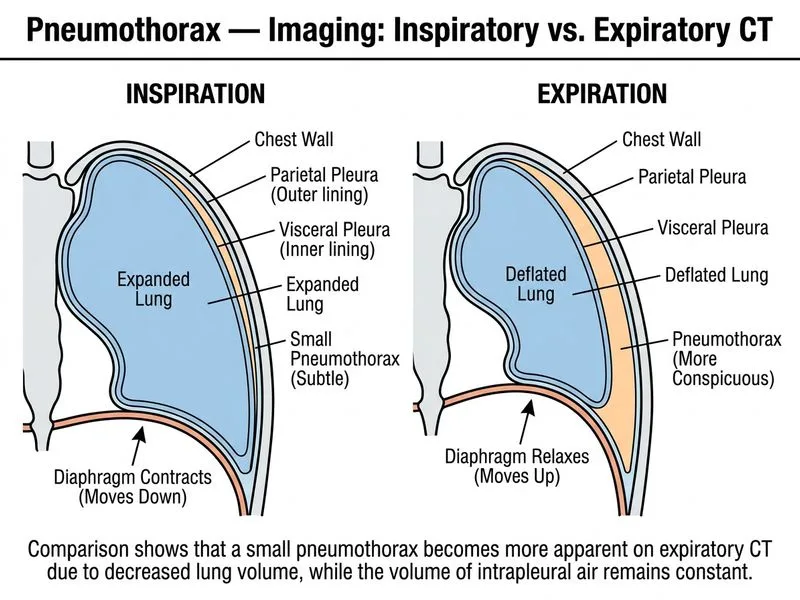
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.