## Tension Pneumothorax: Clinical Recognition and Emergency Management ### Clinical Context: Why This Is a Surgical Emergency **Key Point:** The combination of **hemodynamic instability** (hypotension, tachycardia) + **respiratory distress** + **radiological signs of pneumothorax** = **tension pneumothorax** until proven otherwise. This is a **life-threatening condition requiring immediate decompression**—do NOT delay for confirmatory imaging. ### Pathophysiology of Tension Pneumothorax ```mermaid flowchart TD A[Air enters pleural space]:::outcome --> B[Intrapleural pressure rises]:::outcome B --> C[Lung collapses]:::outcome C --> D[Mediastinal shift]:::outcome D --> E[Compression of SVC/IVC]:::urgent E --> F[Decreased venous return]:::urgent F --> G[Decreased cardiac output]:::urgent G --> H[Hypotension + Shock]:::urgent H --> I[DEATH if not decompressed]:::urgent I --> J[Needle decompression immediately]:::action J --> K[Chest tube insertion]:::action K --> L[Hemodynamic recovery]:::outcome ``` ### Recognition of Tension Pneumothorax | Feature | Simple PTX | Tension PTX | |---------|-----------|-------------| | **Hemodynamics** | Stable or mild tachycardia | Hypotension, shock, JVD | | **Respiratory status** | Dyspnea, normal SpO₂ usually | Severe distress, hypoxia | | **CXR findings** | Pleural line ± hyperlucency | Deep sulcus sign, mediastinal shift | | **Management** | Observation ± chest tube (elective) | **Immediate needle decompression** | | **Imaging** | CXR diagnostic | **Clinical diagnosis—do NOT delay for CT** | **Clinical Pearl:** Tension pneumothorax is a **clinical diagnosis**. The classic teaching is: "If you suspect tension PTX, decompress first and ask questions later." Waiting for CT or confirmatory imaging while the patient decompensates is fatal. ### Why the Deep Sulcus Sign Matters in Supine Position - On **upright CXR**, the pleural line is most visible - On **supine CXR** (ICU, trauma), air rises anteriorly → **deep sulcus sign** (hyperlucency at the lung base, deepened costophrenic angle) - The deep sulcus sign is **more sensitive for PTX in supine patients** than the pleural line - Combined with **hemodynamic instability**, it confirms tension PTX **High-Yield:** In a supine patient with hypotension and respiratory distress, the deep sulcus sign is a red flag for tension PTX. ### Immediate Management Protocol 1. **Needle decompression (STAT):** - Site: **2nd intercostal space, midclavicular line** (or 4th–5th intercostal space, anterior axillary line) - Device: 14–16 gauge needle/catheter - Expect: Rush of air, immediate hemodynamic improvement 2. **Chest tube insertion (within minutes):** - Site: **4th–5th intercostal space, anterior axillary line** (or 5th–6th ICS, midaxillary line) - Size: 28–32 Fr (adults) - Confirm placement with CXR after stabilization 3. **Supplemental oxygen:** - High-flow O₂ (FiO₂ 1.0) increases nitrogen gradient → faster air reabsorption **Warning:** Do NOT delay decompression for imaging. A patient with shock and PTX needs immediate needle decompression—this is a time-critical emergency. ### Why the Other Options Are Wrong **Option 0 (CT chest):** Imaging is contraindicated in hemodynamically unstable patients. CT takes time; the patient needs immediate decompression. CT can be obtained AFTER stabilization if needed for further evaluation. **Option 2 (Observe 24 hours):** Observation is appropriate for small, stable, simple pneumothorax. Tension PTX with shock requires immediate intervention. Waiting 24 hours is fatal. **Option 3 (Oxygen + outpatient follow-up):** Outpatient management is for stable, small PTX. This patient is in shock and requires ICU-level intervention. 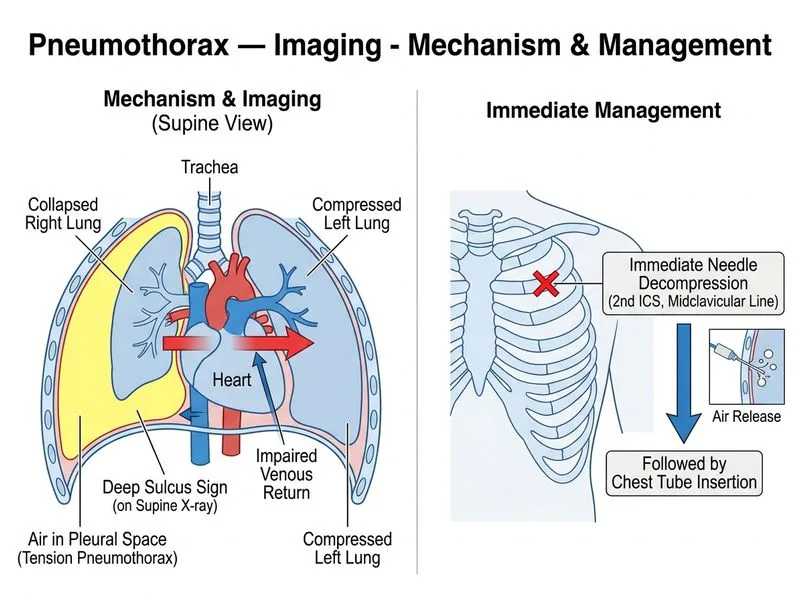
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.