## Acute Primary Angle-Closure Glaucoma: Immediate Management **Key Point:** Acute angle-closure glaucoma is an ophthalmic emergency requiring rapid reduction of IOP and definitive angle opening to prevent permanent vision loss. ### Pathophysiology In acute angle-closure, the peripheral iris is pushed forward against the cornea, blocking the trabecular meshwork and preventing aqueous outflow. IOP rises acutely (often >40 mmHg), causing corneal edema, iris ischemia, and potential optic nerve damage within hours. ### Immediate Management Algorithm ```mermaid flowchart TD A[Acute angle-closure suspected]:::outcome --> B[Confirm: IOP elevated + closed angle on gonioscopy]:::decision B -->|Confirmed| C[Medical therapy to lower IOP]:::action C --> D[Topical: beta-blocker + CAI drops]:::action C --> E[Systemic: oral/IV acetazolamide]:::action C --> F[Topical pilocarpine 4% - constrict pupil]:::action G[Allow corneal edema to clear] --> H[Definitive: Laser peripheral iridotomy]:::action C --> G H --> I[Prevent fellow eye: prophylactic iridotomy]:::action ``` ### Rationale for Correct Answer **Step 1: Medical Therapy (Immediate)** - **Topical pilocarpine 4%:** Causes pupillary constriction (miosis), pulling the peripheral iris away from the angle, reopening the trabecular meshwork. This is the cornerstone of acute management. - **Systemic acetazolamide (500 mg PO or IV):** Reduces aqueous humor production by inhibiting carbonic anhydrase, lowering IOP. - **Topical beta-blockers (timolol) and prostaglandin analogues:** Adjunctive IOP reduction. **Step 2: Definitive Treatment (Urgent, after IOP control)** - **Laser peripheral iridotomy:** Creates a small opening in the peripheral iris, allowing aqueous flow from posterior to anterior chamber, permanently widening the angle. This is the definitive treatment and prevents recurrence. - Timing: Perform once corneal edema has cleared enough to visualize the iris (usually 30 min–2 hours after starting medical therapy). **High-Yield:** The sequence is **medical first, then laser**. Never attempt laser while cornea is too edematous to visualize the iris clearly. ### Why Medical Therapy Before Laser? | Reason | Explanation | |--------|-------------| | **Corneal clarity** | Acute IOP elevation causes corneal edema; medical therapy lowers IOP, allowing edema to resolve and improving visualization for laser | | **Iris perfusion** | High IOP causes iris ischemia; lowering IOP restores perfusion and improves iris contractility to pilocarpine | | **Prevent further damage** | Rapid IOP reduction prevents optic nerve and retinal damage during the window before laser | **Clinical Pearl:** Pilocarpine is less effective in very high IOP (>50 mmHg) because iris ischemia impairs muscle function. Always start systemic acetazolamide and topical agents first to lower IOP, then add pilocarpine once IOP begins to fall. **Warning:** Do NOT attempt laser peripheral iridotomy in the presence of significant corneal edema — the beam cannot be focused and the procedure will fail. Wait for medical therapy to clear the edema. ### Post-Acute Management - Prophylactic laser peripheral iridotomy to the fellow eye (high risk of angle-closure). - Long-term IOP monitoring and topical therapy as needed. - Gonioscopy to assess angle anatomy after acute episode resolves. 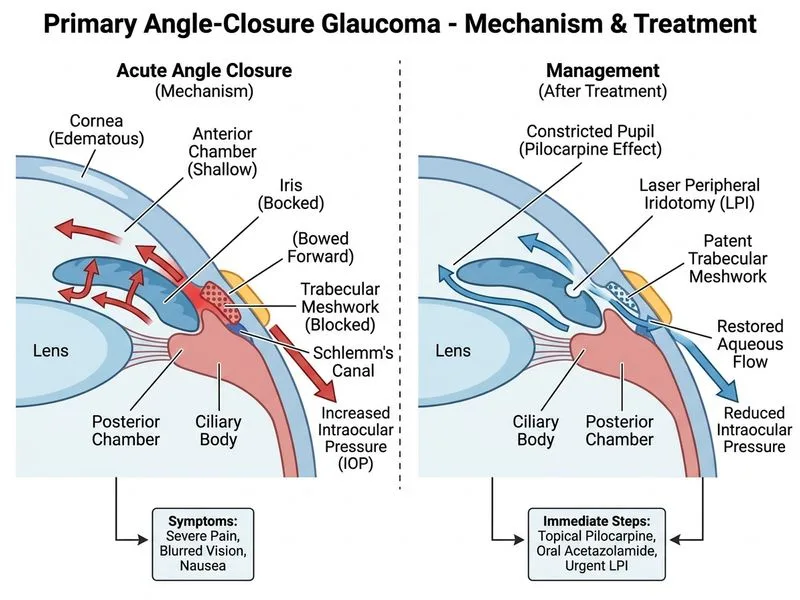
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.