## Subacute/Intermittent Angle-Closure: Prophylactic Management **Key Point:** Intermittent angle-closure episodes (prodromal symptoms) indicate impending acute angle-closure and warrant prophylactic laser peripheral iridotomy to prevent a full acute attack. ### Clinical Presentation Spectrum ```mermaid flowchart TD A[Narrow angle on gonioscopy]:::outcome --> B{Symptoms?}:::decision B -->|None: asymptomatic narrow angle| C[Prophylactic iridotomy if high risk]:::action B -->|Intermittent blurred vision, mild discomfort| D[Prodromal/subacute angle-closure]:::outcome D --> E[Prophylactic laser iridotomy BOTH eyes]:::action B -->|Acute: severe pain, IOP >40, corneal edema| F[Emergency medical + laser therapy]:::urgent E --> G[Prevent acute attack]:::outcome F --> G ``` ### Why This Patient Needs Prophylactic Iridotomy **Clinical Features Indicating Risk:** - Narrow angle on gonioscopy - Hyperopia (shallow anterior chamber predisposes to angle-closure) - Prodromal symptoms: recurrent episodes of blurred vision and mild discomfort - Each episode resolves spontaneously (intermittent appositional closure) **Pathophysiology of Prodromal Symptoms:** Intermittent episodes occur when the iris is pushed forward against the angle during pupil dilation (e.g., dim lighting, emotional stress, mydriatic medications). This temporarily blocks aqueous outflow, causing transient IOP elevation (usually 30–40 mmHg) and corneal edema. The eye recovers when the pupil constricts or the iris moves back. **High-Yield:** Prodromal symptoms are a **red flag** for impending acute angle-closure. The patient is at high risk of a full acute attack (IOP >50 mmHg, severe pain, permanent damage) if not treated prophylactically. ### Why Prophylactic Iridotomy to BOTH Eyes? | Reason | Explanation | |--------|-------------| | **Bilateral narrow angles** | Hyperopia and shallow anterior chamber are bilateral anatomical features | | **Fellow eye risk** | 50–80% of patients with acute angle-closure in one eye develop it in the fellow eye within 5–10 years if untreated | | **Prevention of acute attack** | Prophylactic iridotomy prevents both eyes from ever having an acute episode | | **Permanent solution** | Iridotomy creates a patent peripheral iris opening, eliminating angle-closure risk permanently | **Clinical Pearl:** In a patient with prodromal symptoms and narrow angles, prophylactic iridotomy is indicated even if IOP is currently normal (24 mmHg). The goal is to prevent progression to acute angle-closure. ### Why Not the Other Options? **Option B (Pilocarpine 2% QID):** - Pilocarpine is a temporizing measure, not definitive treatment. - Chronic pilocarpine use has poor compliance and side effects (accommodative spasm, myopia, brow ache). - It does not prevent angle-closure; it only constricts the pupil temporarily. - Pilocarpine is used acutely (during acute angle-closure) or as a bridge before laser, not as long-term monotherapy. **Option C (Gonioscopy under dark room):** - Gonioscopy has already been performed and shows narrow angle with intermittent closure. - Repeating gonioscopy under dark room conditions is diagnostic but does not change management. - The diagnosis is already established; the next step is treatment, not further investigation. **Option D (Oral acetazolamide):** - Acetazolamide is used acutely to lower IOP during an acute angle-closure episode. - It is not indicated for chronic prophylaxis in a patient with normal IOP and intermittent symptoms. - Long-term acetazolamide has significant side effects (paresthesias, metabolic acidosis, hypokalemia) and is not used for prevention. ### Laser Peripheral Iridotomy: Definitive Treatment **Procedure:** - Creates a small opening (150–200 μm) in the peripheral iris - Allows aqueous humor to flow directly from posterior to anterior chamber - Eliminates the pressure gradient that pushes the iris forward - Permanently widens the angle **Outcomes:** - Prevents acute angle-closure in >95% of cases - Can be performed as outpatient laser procedure - Minimal morbidity; rare complications (transient IOP spike, hyphema, corneal abrasion) **Timing:** - In acute angle-closure: after IOP is medically controlled and corneal edema clears - In prodromal/subacute angle-closure: elective, within 1–2 weeks - In asymptomatic narrow angle: prophylactic, within 4–6 weeks **Warning:** Do NOT delay iridotomy in a patient with prodromal symptoms. Each episode carries risk of progression to acute angle-closure with permanent vision loss. 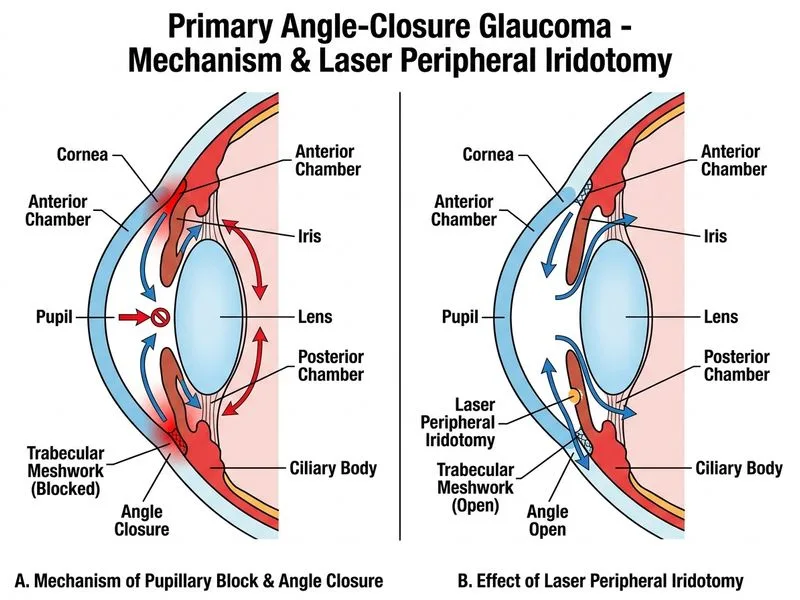
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.