## Clinical Diagnosis **Key Point:** This is acute primary angle-closure glaucoma (PACG) — a medical emergency requiring immediate IOP reduction before laser intervention. ### Why Immediate Medical Therapy First? The patient has: - Sudden severe pain, blurred vision, nausea (classic acute PACG triad) - Corneal edema (preventing clear view of angle for gonioscopy and laser) - IOP 58 mmHg (significantly elevated) - Mid-dilated pupil and occluded angle on gonioscopy **High-Yield:** Corneal edema is the critical barrier. Laser peripheral iridotomy (LPI) cannot be performed safely when the cornea is too hazy to visualize the angle and iris. Medical therapy must first reduce IOP to clear the cornea, then LPI can follow. ### Immediate Medical Management Protocol | Agent | Mechanism | Dosing | |-------|-----------|--------| | Pilocarpine 4% | Pupillary constriction → pulls iris away from angle | Every 15 min × 4 doses, then 4× daily | | IV Acetazolamide | Aqueous humor production ↓ | 500 mg IV/IM | | IV Mannitol | Vitreous volume ↓ (osmotic agent) | 1 g/kg IV bolus | | Topical β-blocker | IOP reduction adjunct | Timolol 0.5% BD | | Topical prostaglandin analogue | IOP reduction adjunct | Latanoprost nightly | **Clinical Pearl:** Pilocarpine works by: 1. Sphincter pupillae contraction → pupil constricts (miosis) 2. Ciliary muscle contraction → zonular tension increases 3. Iris root pulled away from trabecular meshwork → angle opens ### Timeline ```mermaid flowchart TD A["Acute PACG Presentation<br/>IOP >50, Corneal edema"]:::urgent --> B["Immediate Medical Therapy<br/>Pilocarpine, IV Acetazolamide, IV Mannitol"]:::action B --> C{"Corneal clarity<br/>improved?"}:::decision C -->|"Yes (2-4 hrs)"| D["Perform Nd:YAG LPI<br/>Definitive treatment"]:::action C -->|"No"| E["Continue medical therapy<br/>Consider anterior chamber paracentesis"]:::action D --> F["Perform LPI on fellow eye<br/>Prophylaxis"]:::action F --> G["Long-term IOP control<br/>Topical agents ± surgery"]:::outcome ``` **Key Point:** Once corneal edema clears and IOP drops to <40 mmHg, proceed to Nd:YAG laser peripheral iridotomy. This is the definitive treatment — it creates a patent communication between posterior and anterior chambers, relieving pupillary block. **Mnemonic — PACG Management: MEDI-LASER** - **M**annitol (IV osmotic) - **E**thazolamide (IV acetazolamide) - **D**ilation reversal (pilocarpine) - **I**nstill topical agents (β-blocker, PGA) - **L**aser (Nd:YAG LPI once cornea clears) - **A**ssess fellow eye (prophylactic LPI) - **S**urgery (if laser fails or recurrent) - **E**xamine long-term (IOP monitoring) ### Why Not Immediate Laser? Corneal edema prevents visualization of the angle and iris. Attempting LPI through a hazy cornea risks: - Inability to focus the laser - Iris burns instead of peripheral iridotomy - Procedure failure [cite:Khurana Comprehensive Ophthalmology Ch 11] 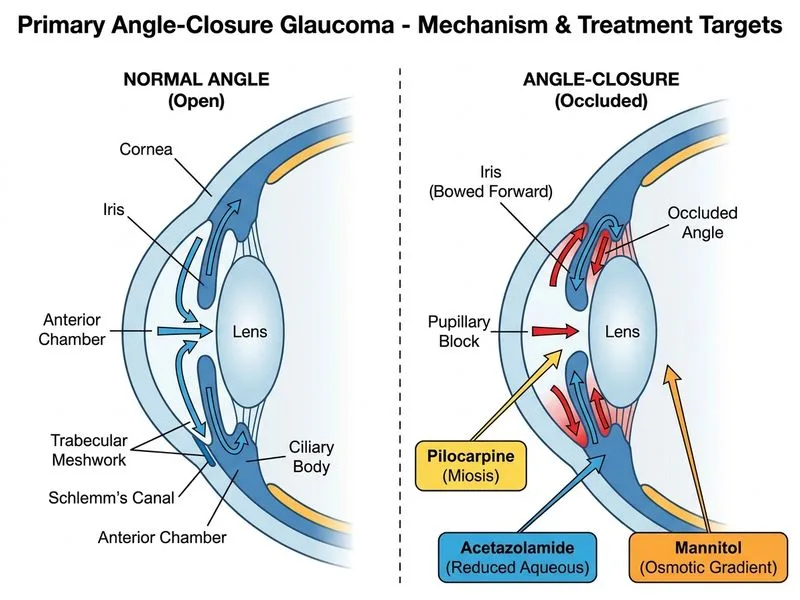
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.