## Investigation of Choice for Risk Assessment in Angle-Closure Glaucoma **Key Point:** Anterior segment OCT (AS-OCT) with angle measurement is the most appropriate investigation to quantify angle dimensions, assess the risk of angle closure, and guide preventive intervention in asymptomatic patients with anatomically narrow angles. ### Why AS-OCT for Risk Stratification? AS-OCT provides: 1. **Quantitative angle measurements** — anterior chamber depth (ACD), angle-opening distance (AOD), trabecular-iris space area (TISA) 2. **Non-contact imaging** — no corneal indentation; safe in shallow anterior chambers 3. **Reproducible measurements** — objective data for monitoring over time 4. **Bilateral assessment** — evaluates both eyes simultaneously 5. **Risk stratification** — identifies patients at high risk who need prophylactic laser peripheral iridotomy (LPI) ### Clinical Scenario Analysis This patient has: - Hyperopia (risk factor for angle closure) - Shallow anterior chamber on slit-lamp - Elevated IOP (24 mmHg) - Asymptomatic (no acute attack) - Family history of glaucoma **High-Yield:** In asymptomatic patients with anatomically narrow angles, AS-OCT quantifies the risk and helps decide whether prophylactic LPI is indicated, preventing progression to acute angle-closure glaucoma. ### Comparison of Investigations in Angle-Closure Evaluation | Investigation | Role | Best Used For | |---|---|---| | **AS-OCT** | Quantitative angle measurement; risk stratification | Asymptomatic narrow angles; monitoring; preventive planning | | **Gonioscopy** | Direct angle visualization; confirms closure | Acute angle closure; post-LPI assessment; angle anatomy | | **Tonometry** | Measures IOP | Screening and monitoring; not diagnostic of angle closure | | **Dilated fundus exam** | Assesses optic disc damage | Detecting glaucomatous optic neuropathy; not for angle assessment | | **Perimetry** | Functional visual field loss | Monitoring disease progression; not for acute diagnosis | **Mnemonic:** **TISA-AOD-ACD** — The three key AS-OCT parameters: - **TISA** = Trabecular-Iris Space Area (most predictive) - **AOD** = Angle-Opening Distance (at 500 and 750 μm from scleral spur) - **ACD** = Anterior Chamber Depth (overall chamber depth) ### Clinical Pearl AS-OCT has largely replaced gonioscopy for screening and risk assessment in asymptomatic patients because it is: - Non-contact (safer in shallow chambers) - Quantitative (objective decision-making) - Reproducible (allows longitudinal monitoring) - Better tolerated by patients Gonioscopy is still essential for confirming angle closure in acute presentations and for detailed angle anatomy assessment. [cite:Khurana Ophthalmology Ch 9] 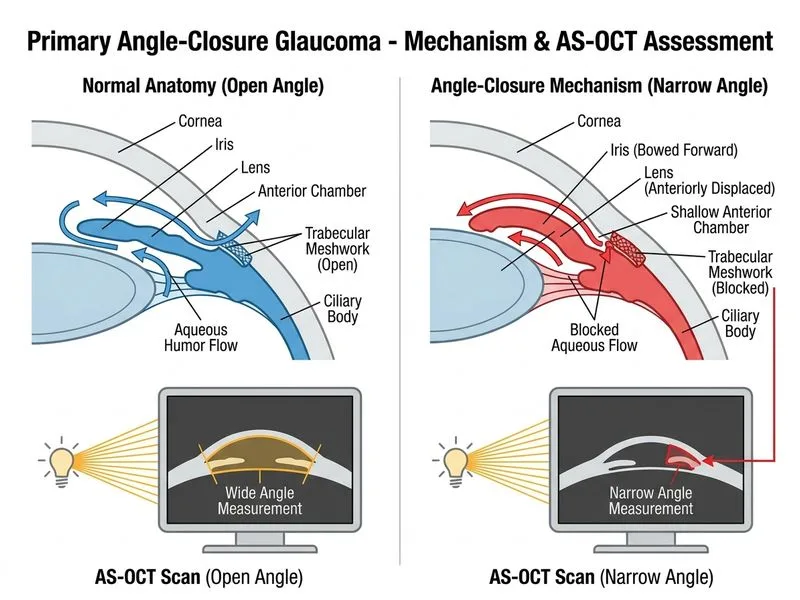
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.