## Acute Angle-Closure Glaucoma: Immediate Management Strategy **Key Point:** In acute angle-closure glaucoma with significantly elevated IOP (>50 mmHg) and corneal edema, medical therapy MUST precede laser treatment because corneal edema obscures the view needed for safe YAG laser peripheral iridotomy. ### Pathophysiology Acute angle closure occurs when the peripheral iris is pushed forward against the trabecular meshwork, blocking aqueous outflow. This leads to rapid IOP elevation and ischemic damage to the optic nerve and retina. ### Management Algorithm ```mermaid flowchart TD A[Acute Angle-Closure Glaucoma]:::outcome --> B{Corneal clarity?}:::decision B -->|Clear| C[YAG Laser Peripheral Iridotomy]:::action B -->|Edematous| D[Maximum Medical Therapy First]:::action D --> E[Topical agents + Systemic agents]:::action E --> F{IOP controlled + Cornea clear?}:::decision F -->|Yes| G[YAG Laser Peripheral Iridotomy]:::action F -->|No| H[Anterior Chamber Paracentesis]:::urgent G --> I[Prophylactic treatment of fellow eye]:::action H --> J[Reasses + Retry Laser]:::action ``` ### Immediate Medical Therapy (Stepwise) 1. **Topical agents** (instill every 15 minutes for 1 hour, then every 30 minutes): - Beta-blocker (timolol 0.5%) - Prostaglandin analogue (latanoprost, bimatoprost, travoprost) - Carbonic anhydrase inhibitor (dorzolamide 1% or brinzolamide 1%) - Avoid topical cholinergic agents (pilocarpine) in acute attack — they worsen angle closure by causing forward lens displacement 2. **Systemic agents**: - Oral acetazolamide 500 mg BD (or IV if vomiting) - IV mannitol 20% if no contraindications (osmotic agent to shrink vitreous) ### Why This Sequence? - Corneal edema from acute IOP elevation prevents clear visualization of the angle during gonioscopy and laser - Medical therapy reduces IOP by 30–50% within 1–2 hours, allowing corneal clarity to return - Once IOP is controlled and cornea is clear, YAG laser peripheral iridotomy can be performed safely and effectively - Iridotomy creates a patent communication between posterior and anterior chambers, relieving pupillary block **High-Yield:** The fellow eye MUST also receive prophylactic YAG laser peripheral iridotomy even if asymptomatic, because it shares the same anatomical risk factors (shallow anterior chamber, short axial length, thick lens). **Clinical Pearl:** If corneal edema is so severe that the angle cannot be visualized even after medical therapy, anterior chamber paracentesis may be needed as a temporizing measure to further lower IOP and allow laser treatment. ### Post-Laser Management - Continue topical IOP-lowering agents for several weeks - Perform gonioscopy to confirm angle opening - Monitor for any residual angle-closure areas - Educate patient on avoiding mydriatic medications (antihistamines, anticholinergics, sympathomimetics) 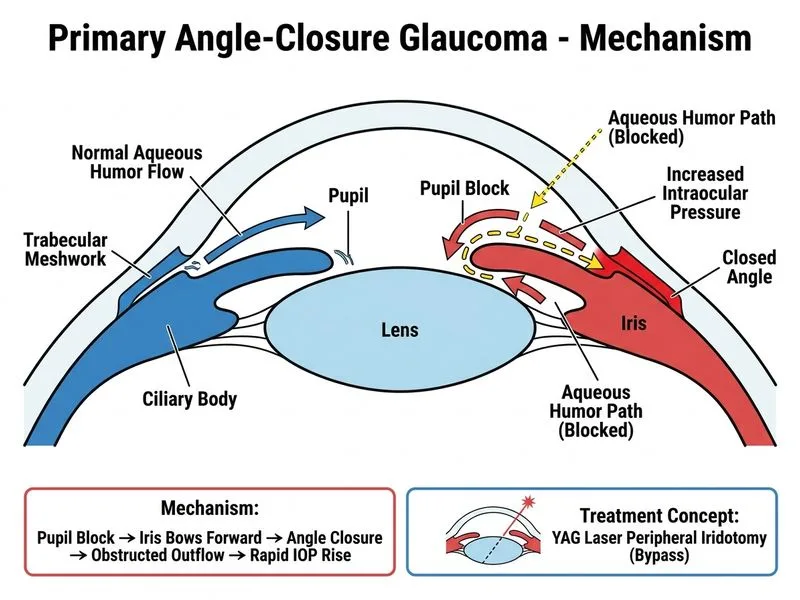
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.