## IOP and Optic Nerve Damage in POAG **Key Point:** While elevated intraocular pressure is the primary modifiable risk factor in POAG, the relationship between IOP and optic nerve damage is not linear or deterministic. Individual susceptibility, vascular factors, and genetic predisposition significantly influence whether a given IOP level causes damage. ### IOP as a Risk Factor — Not Deterministic **High-Yield:** The concept of "target IOP" in POAG management reflects the understanding that: 1. **Ocular hypertension does not always progress** — many patients with elevated IOP (>21 mmHg) never develop glaucomatous optic neuropathy 2. **Normal-tension glaucoma exists** — approximately 30% of POAG patients have IOP consistently ≤21 mmHg yet show progressive optic nerve damage 3. **Individual susceptibility varies** — some patients tolerate higher IOP without damage; others show progression at lower pressures ### Factors Influencing IOP-Damage Relationship | Factor | Impact on Susceptibility | |--------|-------------------------| | **Optic nerve head perfusion** | Poor perfusion → greater damage at same IOP | | **Vascular dysregulation** | Impaired autoregulation → increased vulnerability | | **Age** | Older patients more susceptible to IOP-related damage | | **Genetic factors** | Family history of glaucoma increases risk | | **Systemic hypertension** | Paradoxically increases glaucoma risk (diastolic hypotension) | | **Corneal biomechanics** | Thin corneas may underestimate true IOP | ### The Pathophysiology: Why IOP Matters But Isn't Absolute ```mermaid flowchart TD A[Elevated IOP] --> B[Mechanical strain on axons] A --> C[Reduced perfusion pressure] B --> D[Axonal damage] C --> D D --> E{Individual Susceptibility}:::decision E -->|High| F[Progressive optic nerve damage]:::urgent E -->|Low| G[Stable, no progression]:::outcome H[Vascular dysregulation] --> E I[Genetic predisposition] --> E J[Age, systemic disease] --> E ``` **Clinical Pearl:** The Early Manifest Glaucoma Trial (EMGT) and Ocular Hypertension Treatment Study (OHTS) demonstrated that IOP reduction slows progression, but does not prevent it in all patients. This justifies individualized target IOP goals rather than a universal threshold. ### Normal-Tension Glaucoma (NTG) — The Exception That Proves the Rule **Mnemonic:** **NTG = Non-Pressure-Dependent Damage** — In NTG, optic nerve damage occurs despite IOP ≤21 mmHg, indicating that: - Vascular insufficiency (not mechanical IOP) is the primary driver - Systemic hypotension, nocturnal dips, and vasospasm play major roles - IOP reduction still helps, but other interventions (blood pressure management, vasodilators) are equally important **Warning:** Do NOT assume that a patient with IOP >21 mmHg will inevitably develop glaucoma, nor that normal IOP excludes POAG. Always assess optic nerve head appearance and visual fields independently of IOP alone. [cite:Khurana Ophthalmology Ch 10, Harrison 21e Ch 377] 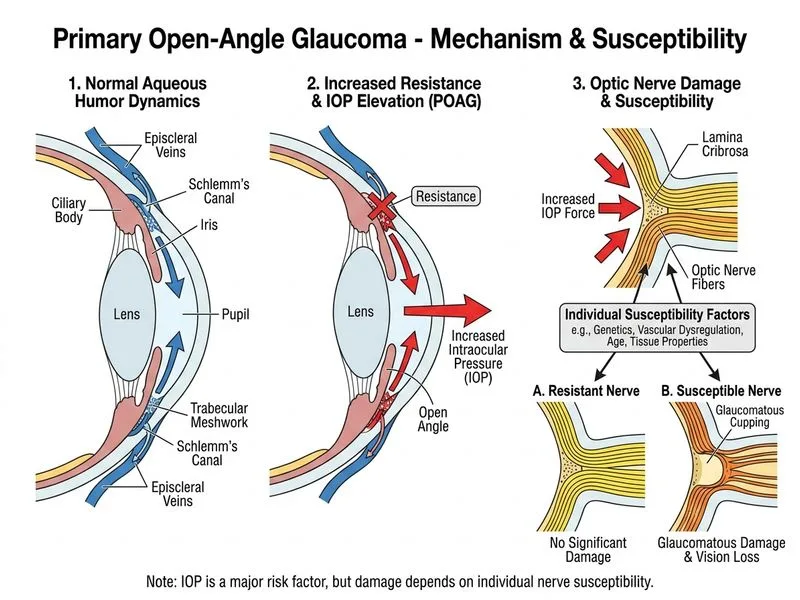
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.