## Investigation of Choice for POAG Confirmation **Key Point:** Automated perimetry (visual field testing) is the gold standard and most appropriate investigation to confirm POAG in a patient with elevated IOP and open angles on gonioscopy. ### Why Automated Perimetry? Automated perimetry detects functional damage to the retinal nerve fiber layer and ganglion cells, which is the hallmark of glaucomatous optic neuropathy. It: 1. Quantifies visual field defects objectively 2. Detects early glaucomatous damage (arcuate defects, nasal steps, paracentral scotomas) 3. Allows serial monitoring to assess disease progression 4. Is reproducible and standardized (24-2 or 30-2 programs) **High-Yield:** The diagnosis of POAG requires: - Elevated IOP (>21 mmHg, though not always) - Open angles on gonioscopy - **Evidence of optic nerve damage** (cup-to-disc ratio >0.5, vertical cup asymmetry, neuroretinal rim thinning) - **Visual field defect** on automated perimetry (most important confirmatory test) ### Diagnostic Sequence for POAG ```mermaid flowchart TD A[Elevated IOP + Family History]:::outcome --> B[Gonioscopy]:::action B --> C{Open angles?}:::decision C -->|Yes| D[Optic disc assessment]:::action D --> E{Disc damage signs?}:::decision E -->|Yes| F[Automated Perimetry]:::action E -->|No| G[Repeat monitoring]:::action F --> H{VF defect present?}:::decision H -->|Yes| I[POAG Confirmed]:::outcome H -->|No| J[Suspect glaucoma/Monitor]:::outcome ``` **Clinical Pearl:** In early POAG, IOP may be normal (<21 mmHg) in some patients (normal-tension glaucoma). The presence of optic nerve damage and visual field defect on perimetry is diagnostic regardless of IOP level. **Mnemonic: POAG Diagnosis = OAD-VF** - **O**pen angles (gonioscopy) - **A**cute/Absent symptoms - **D**isc damage (structural) - **V**isual **F**ield defect (functional) ### Role of Other Investigations | Investigation | Role in POAG | Timing | | --- | --- | --- | | **Automated Perimetry** | Confirms functional damage; gold standard | Initial diagnosis + monitoring | | **OCT (Optic Nerve/RNFL)** | Detects structural damage; early detection | Baseline + follow-up | | **Gonioscopy** | Confirms open angles; rules out secondary glaucoma | Initial assessment | | **Tonometry** | Measures IOP; risk factor assessment | Every visit | | **AS-OCT** | Assesses anterior segment anatomy; rules out angle closure | If angle closure suspected | | **FFA** | Evaluates retinal perfusion; not diagnostic for POAG | Only if vascular pathology suspected | [cite:Khurana Comprehensive Ophthalmology Ch 12] 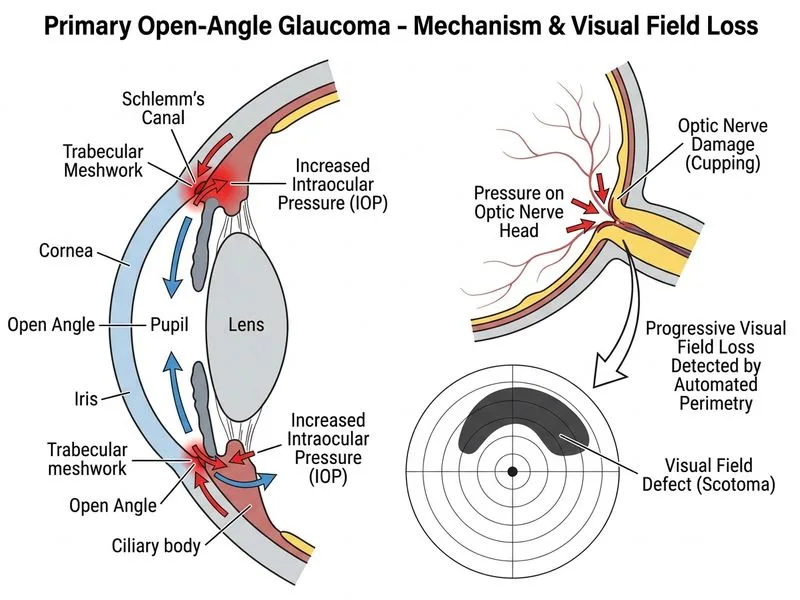
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.