## Clinical Context This patient presents with features suggestive of **suspected POAG (Primary Open-Angle Glaucoma)**: elevated cup-to-disc ratio with notching and borderline elevated IOP, but **normal visual fields and no confirmed diagnosis yet**. ## Why Gonioscopy is the Next Step **Key Point:** Gonioscopy is the **essential confirmatory test** before diagnosing POAG. It must be performed to: 1. Confirm the anterior chamber angle is **open** (Shaffer grade ≥ 3) 2. Rule out secondary causes of open-angle glaucoma (PXF, pigment dispersion, etc.) 3. Establish baseline angle anatomy before treatment **High-Yield:** POAG diagnosis requires **three criteria**: - Open angles on gonioscopy - Elevated IOP (typically > 21 mmHg, though normal-tension POAG exists) - Glaucomatous optic nerve damage (disc cupping/notching, RNFL loss) - Visual field defects (not yet present in this case) ## Why Other Options Are Premature | Option | Why Not Now | |--------|-------------| | Start prostaglandin analogue | Cannot treat POAG without confirming open angles; risks misdiagnosis of angle-closure variant | | Repeat VF + IOP in 3 months | Delays confirmation of diagnosis; gonioscopy must precede any treatment decision | | Laser trabeculoplasty | Inappropriate without confirmed open angles and established diagnosis | **Clinical Pearl:** Even with suspicious disc changes, **gonioscopy is mandatory** before labeling as POAG. This patient has optic nerve cupping but **no visual field loss yet** — he is at risk but not yet confirmed to have glaucoma. **Mnemonic: POAG Diagnosis Triad — OAD:** - **O**pen angles (gonioscopy) - **A**dvanced IOP (typically elevated) - **D**amage to optic nerve (disc + VF) Gonioscopy is the **gatekeeper test** that confirms the angle is open and rules out secondary causes. 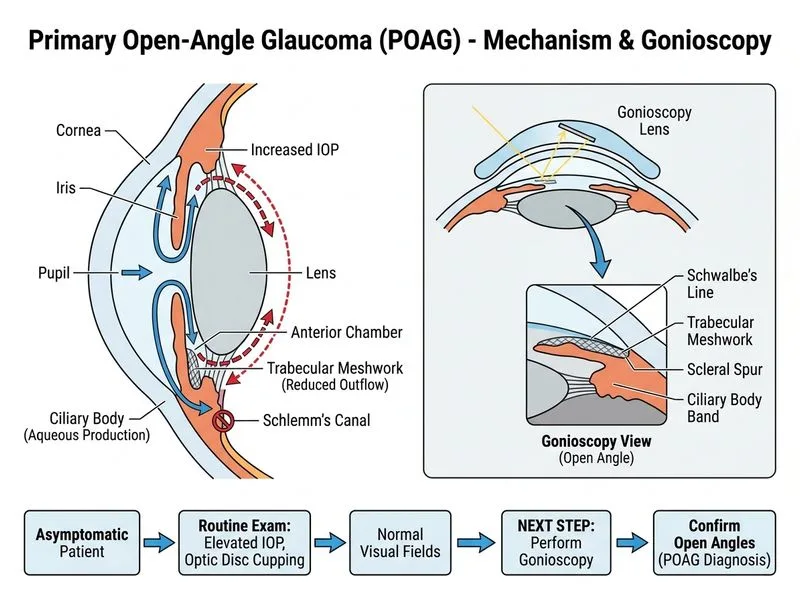
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.