## Distinguishing POAG from PACG ### Key Discriminating Feature **High-Yield:** The hallmark difference between POAG and PACG lies in the **mode and tempo of IOP elevation**. POAG causes gradual, insidious IOP rise that is often detected only on routine screening, whereas PACG typically presents acutely with symptomatic, rapid IOP spikes. ### Comparative Table | Feature | POAG | PACG | | --- | --- | --- | | **Angle appearance (gonioscopy)** | Open and normal | Closed or narrow | | **Anterior chamber depth** | Normal or deep | Shallow | | **IOP elevation** | Gradual, asymptomatic | Acute, symptomatic | | **Presentation** | Chronic, insidious | Acute crisis or prodromal | | **Cornea** | Clear | Edematous (acute attack) | | **Pain** | Absent | Severe (acute) | | **Symptoms** | Often none until advanced** | Halos, blurred vision, pain | **Key Point:** POAG is a **"silent thief of sight"** — patients are often unaware of disease until significant optic nerve damage has occurred. This is why screening is critical. ### Clinical Pearl **Clinical Pearl:** A 55-year-old man found to have elevated IOP (28 mmHg) on routine eye exam with clear media, normal anterior chamber depth, and open angles on gonioscopy is almost certainly POAG. The absence of acute symptoms and the open angle anatomy are diagnostic. ### Why This Matters **Mnemonic: POAG = "Quiet Killer"** - **P**rogressive, **O**pen angles, **A**symptomatic, **G**radual - Versus PACG = "Acute Crisis" **High-Yield:** POAG accounts for ~90% of all glaucoma cases and is the leading cause of irreversible blindness in developed nations. Early detection through IOP screening and optic disc examination is essential. [cite:Parson's Diseases of the Eye 22e Ch 11] 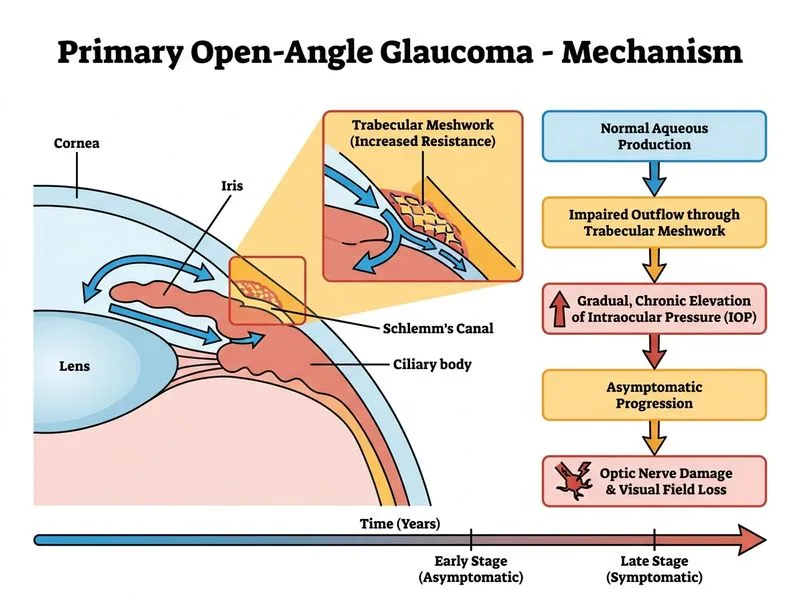
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.