## Clinical Context This patient presents with newly diagnosed primary open-angle glaucoma (POAG) with evidence of structural (optic disc changes) and functional (visual field defects) damage. The IOP of 28 mmHg is elevated, and gonioscopy confirms open angles, ruling out secondary causes. ## Management Algorithm for Newly Diagnosed POAG ```mermaid flowchart TD A[Newly diagnosed POAG with optic disc & VF damage]:::outcome --> B{IOP elevated?}:::decision B -->|Yes| C[Initiate medical therapy]:::action C --> D[Start topical monotherapy<br/>Prostaglandin analogue preferred]:::action D --> E[Recheck IOP in 4 weeks]:::action E --> F{Target IOP achieved?}:::decision F -->|Yes| G[Continue & monitor 6-monthly]:::action F -->|No| H[Add second agent or escalate]:::action B -->|No| I[Observe with regular monitoring]:::action ``` ## Why Topical Prostaglandin Monotherapy? **Key Point:** Prostaglandin analogues (latanoprost, travoprost, bimatoprost) are first-line agents in POAG because they: - Provide the greatest IOP reduction (25–35%) - Are administered once daily (evening dosing) - Have minimal systemic side effects - Are cost-effective **High-Yield:** In treatment-naïve POAG with elevated IOP and documented glaucomatous damage, medical therapy is the standard initial approach. Laser trabeculoplasty and surgery are reserved for inadequate response to medical therapy or patient non-compliance. ## Why Not the Other Options? | Option | Reason | |--------|--------| | Laser trabeculoplasty immediately | Laser is second-line, used after medical therapy failure or as adjunct. Not first-line in newly diagnosed POAG. | | Trabeculectomy without prior medical therapy | Surgical intervention is reserved for advanced disease uncontrolled on maximum medical therapy or poor compliance. This patient has not yet received medical treatment. | | Observation without treatment | Contraindicated. The patient has documented optic nerve damage (0.7 CDR with notching) and visual field defects. Untreated elevated IOP will cause progressive irreversible vision loss. | **Clinical Pearl:** The target IOP is individualized based on baseline IOP, degree of damage, and life expectancy. In this case, a target IOP reduction of 25–30% from baseline (aiming for ~20 mmHg) would be reasonable given the presence of early field defects. **Tip:** Always recheck IOP 4 weeks after initiating or changing therapy to assess response. If target IOP is not achieved, add a second agent (beta-blocker, CAI, or alpha-2 agonist) rather than switching monotherapy. 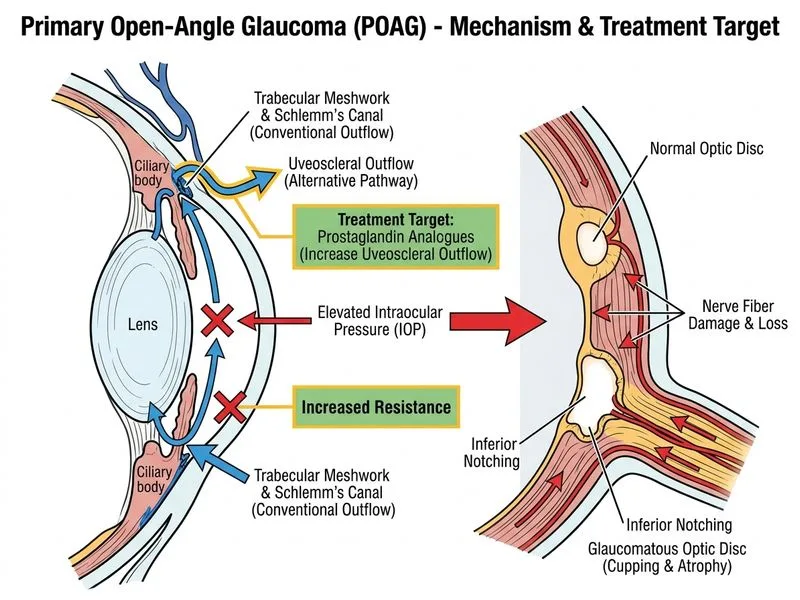
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.