## Clinical Context This patient has POAG on monotherapy with suboptimal IOP control. Despite 8 weeks of latanoprost, the IOP reduction is only ~8% (from 26 to 24 mmHg OD), which is insufficient given the presence of glaucomatous visual field changes. The target IOP should be lower to halt disease progression. ## Assessment of Therapeutic Response **Key Point:** A prostaglandin analogue typically achieves 25–35% IOP reduction. This patient's 8% reduction suggests inadequate response and need for escalation. **High-Yield:** When monotherapy fails to achieve target IOP after 4–8 weeks, the next step is to add a complementary second agent rather than switch monotherapy. ## Rationale for Adding Beta-Blocker ```mermaid flowchart TD A[POAG on monotherapy<br/>IOP still elevated]:::outcome --> B{Adequate IOP reduction?}:::decision B -->|No| C[Add second agent]:::action C --> D{Choose agent based on<br/>contraindications & comorbidities}:::decision D -->|No systemic CI| E[Beta-blocker or CAI]:::action D -->|Asthma/COPD| F[CAI or alpha-2 agonist]:::action D -->|Renal disease| G[Avoid CAI; use alpha-2 agonist]:::action E --> H[Recheck IOP in 4 weeks]:::action F --> H G --> H ``` ## Why Add Rather Than Switch? | Strategy | Rationale | |----------|----------| | **Add second agent** | Synergistic IOP reduction; different mechanism of action (prostaglandin + beta-blocker = ~40–50% total reduction). Proven approach. | | **Switch monotherapy** | Wastes time; no evidence that a different prostaglandin will work better if latanoprost has failed. | **Clinical Pearl:** Beta-blockers (timolol 0.5% BID) are excellent second agents because they: - Reduce aqueous humor production - Are well-tolerated topically - Have no systemic contraindications in this patient - Provide additive IOP reduction with prostaglandins **Tip:** Always check for contraindications (asthma, COPD, heart block, bradycardia) before prescribing beta-blockers. If present, use a carbonic anhydrase inhibitor (dorzolamide/brinzolamide) or alpha-2 agonist instead. ## Why Not the Other Options? | Option | Reason | |--------|--------| | Continue monotherapy | IOP reduction is inadequate (only 8%). Continuing without escalation risks progressive optic nerve damage. | | Switch to different prostaglandin | No evidence that switching prostaglandins improves response if one has already failed. Delays necessary escalation. | | Laser trabeculoplasty | Premature. Medical therapy escalation (adding a second agent) should be attempted first. Laser is indicated after failure of maximum medical therapy. | 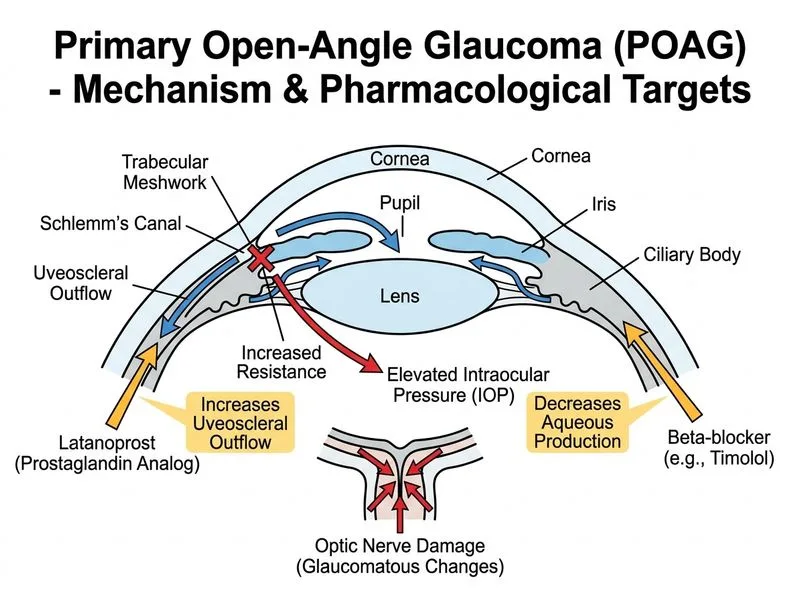
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.