## Distinguishing POAG from PACG ### Key Clinical Discriminator **Key Point:** The anterior chamber angle status and mode of onset are the primary distinguishing features between POAG and PACG. ### Comparative Table | Feature | POAG | PACG | | --- | --- | --- | | **Anterior Chamber** | Normal depth, wide angles | Shallow, narrow/closed angles | | **Onset** | Insidious, asymptomatic | Acute or subacute | | **Symptoms** | Often none until advanced | Pain, redness, blurred vision | | **Gonioscopy Finding** | Open angles (>20°) | Narrow/closed angles (<20°) | | **IOP Rise** | Gradual, progressive | Sudden, often >40 mmHg | | **Cornea** | Clear | Edematous (acute attack) | ### Pathophysiology **High-Yield:** POAG results from **trabecular meshwork dysfunction** with normal angle anatomy, whereas PACG results from **mechanical angle closure** due to pupillary block or anterior segment crowding. **Clinical Pearl:** The gonioscopic finding of **open angles** in POAG is pathognomonic and distinguishes it from PACG at the bedside. A patient with elevated IOP and open angles on gonioscopy has POAG until proven otherwise. ### Why Gonioscopy is Essential 1. **Angle assessment** — direct visualization of angle structures 2. **Trabecular meshwork appearance** — may show pigmentation or damage in POAG 3. **Exclusion of secondary causes** — rules out angle-closure mechanism **Mnemonic:** **OPEN angles = POAG; CLOSED angles = PACG** ### Clinical Presentation Contrast - **POAG:** Silent thief of sight — patients are unaware until visual field loss is detected on screening - **PACG:** Dramatic presentation — acute pain, redness, and vision loss prompt urgent evaluation 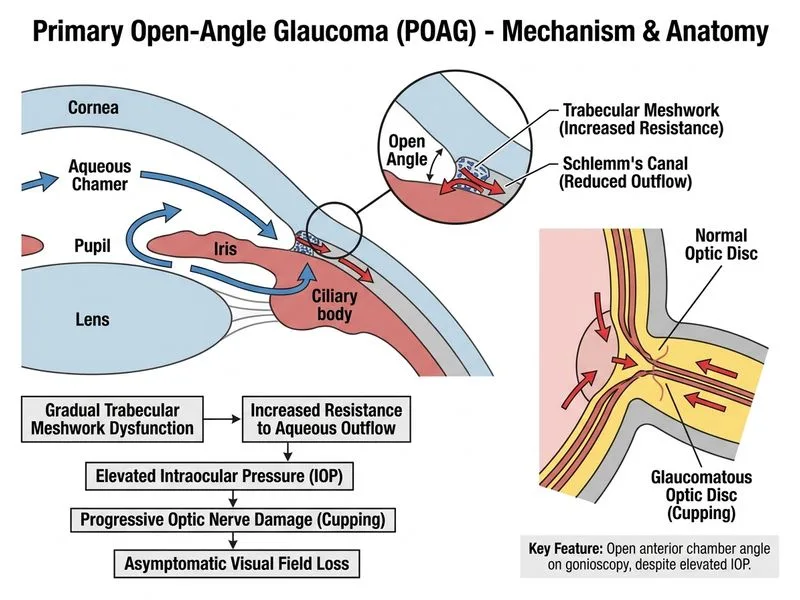
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.