## Clinical Assessment This patient presents with **classic plaque psoriasis** affecting <10% BSA (mild-to-moderate disease) with positive diagnostic signs (Auspitz, Koebner phenomenon) and a clear family history. The diagnosis is clinical and does not require biopsy confirmation. ## Management Algorithm for Psoriasis ```mermaid flowchart TD A[Psoriasis diagnosed clinically]:::outcome --> B{BSA involvement?}:::decision B -->|<10% mild-moderate| C[Topical therapy first-line]:::action B -->|10-30% moderate| D[Topical + phototherapy]:::action B -->|>30% severe| E[Systemic agents]:::action C --> F[Corticosteroids + Vitamin D analogues]:::action D --> G[NB-UVB phototherapy]:::action E --> H[Methotrexate/Biologic]:::action I[Joint symptoms present?]:::decision I -->|Yes| J[Rheumatology referral]:::action I -->|No| K[Monitor clinically]:::action ``` ## Why Topical Therapy is First-Line **Key Point:** For plaque psoriasis affecting <10% BSA **without systemic involvement**, topical corticosteroids (Class III–IV potency on flexures/face; Class I–II on trunk/limbs) combined with vitamin D analogues (calcipotriol) are the **gold standard initial therapy** [cite:Park 26e Ch 6]. **High-Yield:** The combination of a potent topical corticosteroid + vitamin D analogue offers: - Faster onset of corticosteroid - Sustained benefit and steroid-sparing effect from vitamin D analogue - Lower risk of tachyphylaxis than corticosteroid monotherapy **Clinical Pearl:** Auspitz sign (pinpoint bleeding when scale is scraped) and Koebner phenomenon (lesions at sites of trauma) are **pathognomonic for psoriasis** and support clinical diagnosis without need for biopsy. ## Why Systemic Therapy Is Not Yet Indicated - **Methotrexate** is reserved for moderate-to-severe disease (>10% BSA), pustular psoriasis, or erythrodermic psoriasis, or failure of topical therapy. - This patient has mild-moderate plaque psoriasis; systemic agents carry hepatotoxicity, myelosuppression, and teratogenicity risks that are not justified at this stage. ## Monitoring for Psoriatic Arthritis **Key Point:** Although the patient has **no current joint symptoms**, psoriatic arthritis (PsA) develops in 5–30% of psoriasis patients. However, **routine rheumatology referral is not indicated in asymptomatic patients**. Clinical surveillance for joint pain, swelling, or morning stiffness is appropriate during follow-up. 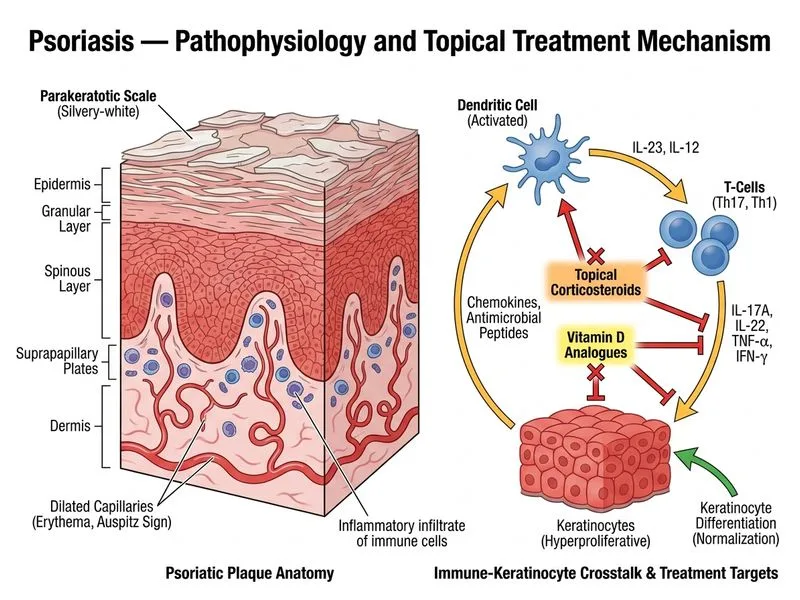
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.