## Clinical Diagnosis: Pustular Psoriasis (Acute Exacerbation) This patient has **acute generalized pustular psoriasis** (likely triggered by corticosteroid withdrawal), a severe and potentially life-threatening variant characterized by: - Widespread erythema with pinpoint pustules - Systemic symptoms (fever, malaise) - Elevated inflammatory markers (WBC, CRP) - Hypoalbuminemia (indicating systemic inflammation and protein loss) ## Classification of Psoriasis Severity | Feature | Mild | Moderate | Severe/Pustular | |---------|------|----------|------------------| | **BSA** | <10% | 10–30% | >30% or any pustular | | **Systemic symptoms** | None | Possible | Fever, malaise, systemic toxicity | | **Hospitalization need** | Outpatient | Outpatient/day care | **Inpatient mandatory** | | **First-line therapy** | Topical | Topical + phototherapy | Systemic (acitretin, cyclosporine) | ## Management Algorithm for Severe Pustular Psoriasis ```mermaid flowchart TD A[Acute pustular psoriasis]:::outcome --> B[Assess severity & triggers]:::action B --> C{Systemic toxicity present?}:::decision C -->|Yes fever, malaise, BSA >30%| D[Admit to hospital]:::urgent C -->|No| E[Day care/outpatient] D --> F[Discontinue systemic corticosteroids]:::action F --> G[Start systemic retinoid or cyclosporine]:::action G --> H[Supportive care: fluids, electrolytes]:::action H --> I[Monitor for complications]:::action I --> J{Complications?}:::decision J -->|Sepsis, SIRS| K[ICU admission]:::urgent J -->|None| L[Gradual improvement]:::outcome ``` ## Why Hospitalization is the Correct Next Step **Key Point:** Acute generalized pustular psoriasis is a **dermatological emergency** requiring **immediate hospitalization** because of: 1. **Systemic toxicity:** Fever, malaise, and elevated inflammatory markers indicate SIRS (Systemic Inflammatory Response Syndrome) 2. **Risk of complications:** Sepsis, electrolyte imbalance, dehydration, acute kidney injury, and secondary infection 3. **Hypoalbuminemia (2.8 g/dL):** Indicates significant protein loss through inflamed skin and systemic inflammation 4. **Need for intensive monitoring:** IV fluids, electrolyte correction, and systemic therapy initiation **High-Yield:** Pustular psoriasis has a **mortality rate of 1–5%** if not managed aggressively in hospital [cite:Park 26e Ch 6]. ## Immediate Management Steps After Admission 1. **Discontinue systemic corticosteroids** (which triggered the flare) 2. **Initiate systemic therapy:** - **Acitretin** (oral retinoid): First-line for pustular psoriasis; 0.5–1 mg/kg/day - **Cyclosporine** (if rapid response needed): 3–5 mg/kg/day IV or oral - Avoid methotrexate in acute pustular psoriasis (risk of hepatotoxicity with rapid cell turnover) 3. **Supportive care:** - IV fluids and electrolyte replacement - Emollients and bland topical agents (avoid irritants) - Antibiotics only if secondary infection suspected 4. **Monitoring:** - Daily assessment of BSA, vital signs, and inflammatory markers - Renal function, liver function, lipid profile (especially if on acitretin) **Warning:** Do NOT restart systemic corticosteroids — they can paradoxically worsen pustular psoriasis upon withdrawal (rebound phenomenon). ## Why Other Options Are Inappropriate - **Topical therapy alone:** Insufficient for >80% BSA and systemic toxicity; risk of rapid deterioration - **Phototherapy:** Contraindicated in acute pustular psoriasis (can exacerbate) - **Outpatient management:** Dangerous given fever, elevated CRP, hypoalbuminemia, and risk of sepsis 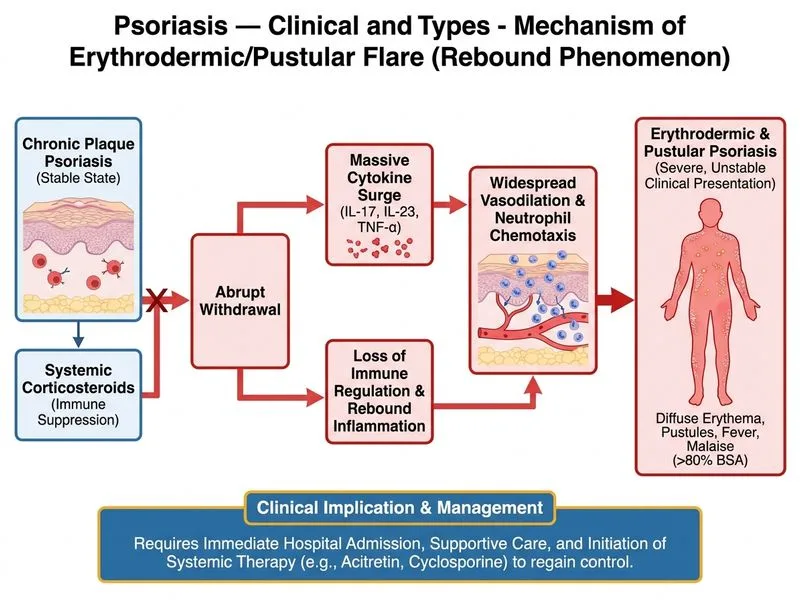
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.