## Diagnosis: Acute Generalized Exanthematous Pustulosis (AGEP) ### Clinical Presentation The patient presents with features highly suggestive of AGEP: - Sudden onset of small erythematous papules and pustules - Widespread distribution (face, trunk, flexural areas) - Temporal relationship with drug exposure (antifungal agent) - Absence of fever or systemic symptoms (though may be present) - Intense pruritus and pain - Rapid progression (within 2 weeks of drug initiation) ### Key Diagnostic Features **Key Point:** AGEP is a severe cutaneous adverse reaction (SCAR) characterized by acute onset of non-follicular pustules on an erythematous base, typically triggered by drugs (antibiotics, anticonvulsants, antiretrovirals, antifungals) or rarely infections. **High-Yield:** The hallmark of AGEP is the presence of sterile pustules (not follicular) on an erythematous background, distinguishing it from folliculitis or acne. Histology shows subcorneal or intraepidermal pustules with minimal dermal inflammation. ### Comparison of Psoriasis Variants and AGEP | Feature | AGEP | Pustular Psoriasis | Erythrodermic Psoriasis | Inverse Psoriasis | |---------|------|-------------------|----------------------|-------------------| | Onset | Acute (days–weeks) | Chronic or acute | Chronic or acute | Chronic | | Trigger | Drug/infection | Withdrawal, stress, infection | Withdrawal, stress, infection | Friction, moisture | | Pustules | Non-follicular, sterile | Non-follicular | Rare | Absent | | Distribution | Generalized, flexural | Generalized or localized | Generalized (>90% BSA) | Intertriginous areas | | Fever | May be present | Usually absent | Often present | Absent | | Prognosis | Self-limited (weeks) | Chronic, relapsing | Serious, life-threatening | Chronic | | Histology | Subcorneal pustules, minimal inflammation | Spongiform pustules, parakeratosis | Erythema, scaling | Minimal scale | **Clinical Pearl:** AGEP typically resolves within 1–2 weeks of drug withdrawal, whereas pustular psoriasis is chronic and relapsing. The absence of systemic symptoms in this case makes AGEP more likely than erythrodermic psoriasis, which often presents with fever, chills, and hemodynamic instability. ### Common Drug Triggers for AGEP **Mnemonic:** **ABACUS** for AGEP triggers: - **A**ntibiotics (β-lactams, macrolides, fluoroquinolones) - **B**eta-blockers - **A**nticonvulsants - **C**alcineurin inhibitors - **U**nknown (infections: HHV-6, EBV) - **S**ulfonamides Antifungals (azoles, terbinafine) are also well-recognized triggers. ### Pathophysiology AGEP is thought to result from: 1. T-cell-mediated hypersensitivity reaction to the offending drug or pathogen 2. Rapid recruitment of neutrophils to the epidermis 3. Formation of sterile pustules without significant dermal inflammation 4. Self-limited course due to rapid clearance of the trigger ### Management 1. **Immediate:** Discontinue the offending drug 2. **Supportive:** Topical corticosteroids, emollients, antihistamines for pruritus 3. **Systemic:** Oral corticosteroids (short course) for severe cases 4. **Monitoring:** Watch for secondary infection, fluid loss 5. **Prognosis:** Complete resolution within 1–2 weeks of drug withdrawal **Warning:** Do not confuse AGEP with pustular psoriasis triggered by drug withdrawal. In this case, the patient started (not stopped) the antifungal, making AGEP the diagnosis. [cite:Fitzpatrick's Dermatology in General Medicine 9e Ch 13] 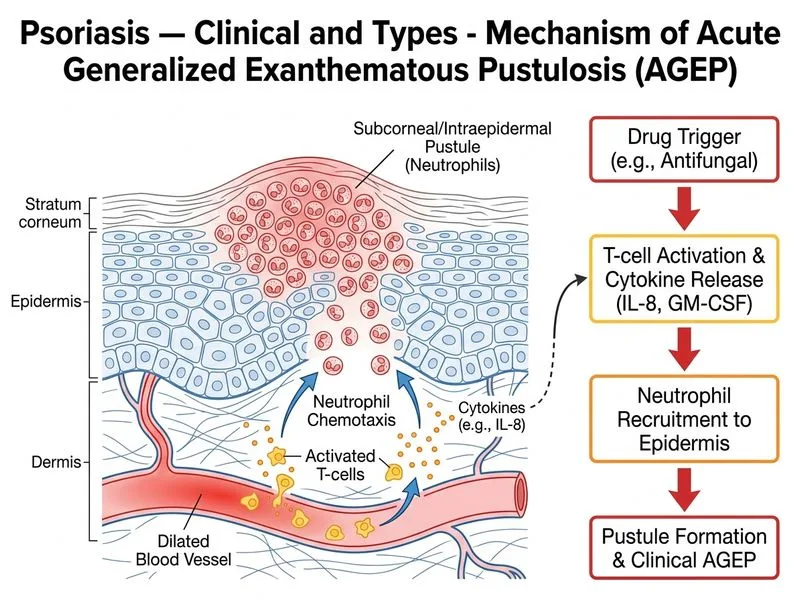
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.