## Diagnosis: Pustular Psoriasis of the Palms and Soles (Acanthosis Pustulosa) ### Clinical Presentation The patient presents with the characteristic features of pustular psoriasis localized to the palms and soles: - Well-demarcated erythematous plaques with hyperkeratosis - Pustules on palms and soles (acanthosis pustulosa) - Bilateral and symmetrical distribution - Severe pruritus and pain - History of chronic plaque psoriasis - Absence of systemic involvement (no fever, no constitutional symptoms) ### Classification of Psoriasis Types **High-Yield:** Pustular psoriasis comprises 1–3% of all psoriasis cases and is classified into generalized and localized forms. Localized pustular psoriasis affecting palms and soles is more common than generalized pustular psoriasis. | Type | Features | Systemic Involvement | Prognosis | | --- | --- | --- | --- | | **Chronic plaque psoriasis** | Well-demarcated plaques, silvery scale, extensor surfaces | Arthritis in 10–15% | Chronic, relapsing-remitting | | **Pustular psoriasis (localized)** | Pustules on palms/soles, hyperkeratosis, painful | Rare | Chronic, difficult to treat | | **Pustular psoriasis (generalized)** | Widespread erythema with pustules, fever, systemic toxicity | Common (life-threatening) | Acute, severe | | **Inverse psoriasis** | Flexor surfaces, intertriginous areas, minimal scale | Rare | Chronic | | **Erythrodermic psoriasis** | >90% body surface area involvement, systemic symptoms | Common | Acute, severe | | **Guttate psoriasis** | Small papules (1–10 mm), trunk and proximal limbs, post-streptococcal | Rare | Often self-limited | ### Pathophysiology of Pustular Psoriasis **Key Point:** Pustular psoriasis is characterized by neutrophilic infiltration into the epidermis, forming Munro microabscesses and subcorneal pustules. The pathogenesis involves IL-36 signaling dysregulation. 1. **Localized form (palms/soles):** IL-36 pathway activation → neutrophil recruitment → pustule formation 2. **Generalized form:** Severe systemic inflammation, often triggered by infection, pregnancy, or drug withdrawal (especially systemic corticosteroids) ### Distinguishing Features from Other Pustular Disorders **Clinical Pearl:** The presence of a prior history of chronic plaque psoriasis, bilateral symmetrical distribution, and hyperkeratotic base of pustules strongly suggest pustular psoriasis rather than infectious or inflammatory eczematous conditions. **Mnemonic: PALMS** — Pustules, Acanthosis pustulosa, Localized to palms/soles, Marked hyperkeratosis, Symmetrical distribution ### Management Approach Localized pustular psoriasis is notoriously difficult to treat: - **First-line:** Potent topical corticosteroids (Class II–III) + keratolytics (salicylic acid) - **Second-line:** Topical retinoids (tretinoin), vitamin D analogues - **Third-line:** Systemic agents — acitretin (most effective), methotrexate, or biologics (TNF-α inhibitors, IL-17 inhibitors) - **Avoid:** Systemic corticosteroid withdrawal (can precipitate generalized pustular psoriasis) **Warning:** Abrupt withdrawal of systemic corticosteroids in a patient with psoriasis can trigger generalized pustular psoriasis, which is a dermatological emergency. 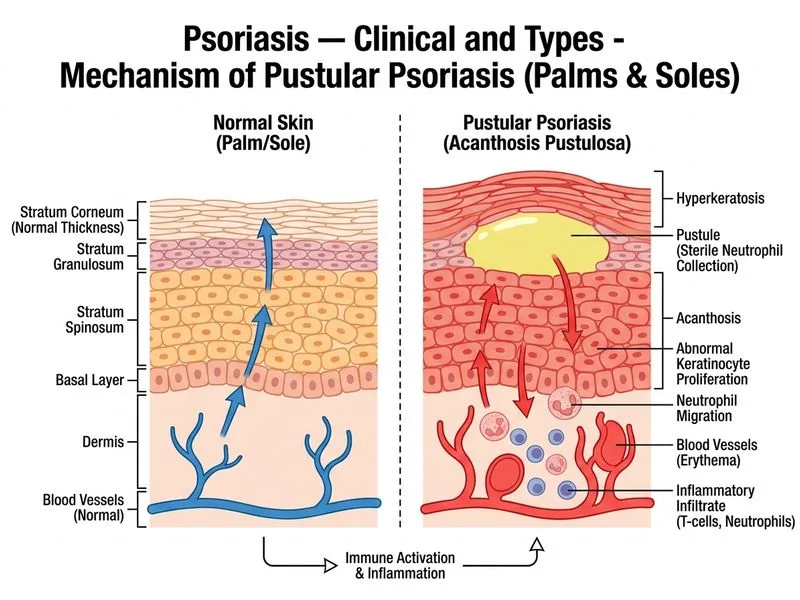
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.