## Acute Pustular Psoriasis — Emergency Recognition and Management **Key Point:** This patient has **acute pustular psoriasis**, a severe, life-threatening variant triggered by beta-blocker withdrawal or initiation. Immediate hospitalization and systemic intervention are mandatory. ### Clinical Diagnosis **High-Yield:** Pustular psoriasis is characterized by: - Sudden onset of widespread erythema with sterile pustules - Systemic symptoms (fever, malaise, elevated WBC) - Often triggered by: - Withdrawal of systemic corticosteroids (rebound) - Initiation of beta-blockers, lithium, or NSAIDs - Severe infection or pregnancy **Warning:** Do NOT confuse with secondary bacterial infection — pustules are sterile; cultures are negative. ### Management Pathway for Pustular Psoriasis ```mermaid flowchart TD A[Widespread pustules + fever + high BSA]:::outcome --> B{Trigger identified?}:::decision B -->|Beta-blocker, lithium, NSAIDs| C[DISCONTINUE offending agent]:::urgent B -->|Recent corticosteroid withdrawal| D[Reinstitute steroids cautiously]:::action C --> E[Admit to hospital]:::urgent D --> E E --> F[IV/oral corticosteroids + supportive care]:::action E --> G[Fluid, electrolyte, temperature monitoring]:::action F --> H[Consider acitretin or biologics if severe/recurrent]:::action G --> I[Assess for systemic complications]:::action ``` ### Why Beta-Blocker Discontinuation Is Critical | Aspect | Detail | |--------|--------| | **Mechanism** | Beta-blockers impair immune regulation; trigger pustular transformation in susceptible patients | | **Timing** | Onset typically 2–4 weeks after initiation | | **Reversibility** | Discontinuation leads to rapid improvement within days | | **Continuation risk** | Persistent pustular flare, systemic toxicity, sepsis, death if not stopped | **Clinical Pearl:** Pustular psoriasis can progress to **erythroderma** and **sepsis** if untreated. This is a dermatological emergency requiring ICU-level monitoring. ### Systemic Management in Hospital 1. **Discontinue beta-blocker immediately** — This is the single most important intervention. 2. **Systemic corticosteroids** — Oral prednisolone 0.5–1 mg/kg/day or IV methylprednisolone if severe. 3. **Supportive care** — IV fluids, temperature control, infection prevention, electrolyte monitoring. 4. **Avoid topical agents** — Extensive pustular disease does not respond to topical therapy; may worsen irritation. 5. **Consider acitretin or TNF-α inhibitors** — For recurrent or refractory cases after acute phase stabilization. **Mnemonic:** **PUSTULAR** = **P**rednisone/corticosteroids, **U**rgent admission, **S**top offending drug, **T**emperature & fluid support, **U**nderstand systemic risk, **L**aboratory monitoring (WBC, renal, liver), **A**void topicals, **R**efer to specialist if refractory. 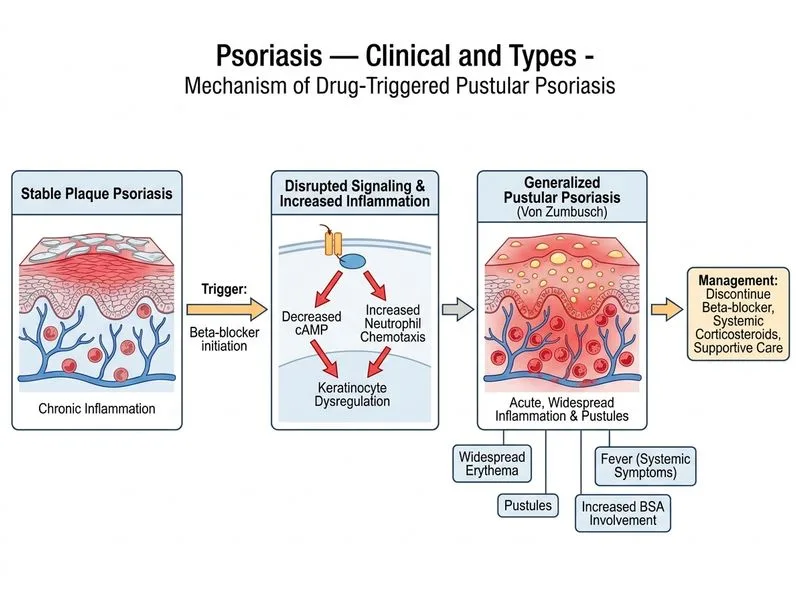
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.