## Pulmonary Infarction in the Context of PE ### Pathophysiology of Hampton's Hump **Key Point:** A wedge-shaped peripheral consolidation with a rounded apex pointing toward the hilum (Hampton's hump) represents **pulmonary infarction**—tissue necrosis resulting from venous occlusion by the embolism and loss of collateral blood supply. ### Mechanism of Pulmonary Infarction 1. **Pulmonary artery occlusion** by thrombus → loss of primary blood supply 2. **Dual blood supply failure:** - Pulmonary circulation blocked by PE - Bronchial circulation insufficient (especially in areas of low pressure) 3. **Tissue hypoxia and necrosis** → hemorrhagic infarction 4. **Hemorrhage into alveoli** → consolidation visible on imaging **Clinical Pearl:** Pulmonary infarction occurs in only **5–15% of PE cases**. It is more common when: - PE is large (lobar or segmental occlusion) - Underlying cardiopulmonary disease limits collateral flow (e.g., COPD, heart failure) - Venous stasis is prolonged ### Radiographic Features of Hampton's Hump | Feature | Description | |---------|-------------| | **Shape** | Wedge-shaped (triangular) | | **Apex** | Rounded, pointing toward hilum | | **Base** | Pleural surface (peripheral) | | **Density** | Consolidation (opaque) | | **Timeline** | Appears 24–72 hours after PE | | **Evolution** | Gradually resolves over weeks; may cavitate if infected | **High-Yield:** The **combination of a filling defect in the PA + peripheral wedge-shaped consolidation** is virtually pathognomonic for PE with infarction. The consolidation is the *consequence* of the embolism, not a separate diagnosis. ### Why This Patient Has Infarction - **Large PE** (left lower lobe artery occlusion) - **Underlying COPD** → reduced bronchial collateral perfusion - **Prolonged immobilization** → extensive thrombosis - **Hemoptysis** → evidence of alveolar hemorrhage **Mnemonic:** **CHAMP** — **C**onsolidation, **H**emoptysis, **A**cute, **M**assive PE, **P**leural base = Hampton's hump. ### Differential Considerations **Why not bacterial pneumonia?** Pneumonia would lack the filling defect in the PA and typically shows more lobar/segmental distribution with air bronchograms. Clinical context (immobilization, acute PE) favors infarction. **Why not COPD exacerbation?** COPD exacerbation causes bronchitis and mucus plugging but does not produce the characteristic wedge-shaped pleural-based consolidation or the PA filling defect. 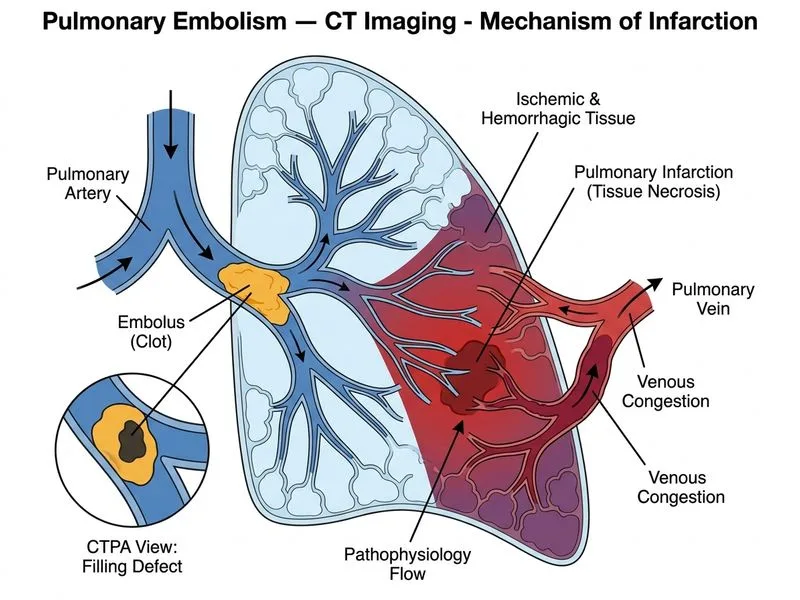
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.