## Diagnostic Threshold for PE on CTPA **Key Point:** A filling defect must be identified in **segmental or larger pulmonary arteries** (diameter ≥2–5 mm) to be considered diagnostic for acute PE. Subsegmental PE detection is unreliable and not recommended as a sole basis for diagnosis. ### Vessel Size and Diagnostic Reliability | Vessel Level | Diameter | Diagnostic Confidence | Clinical Significance | |--------------|----------|----------------------|----------------------| | **Main PA** | >10 mm | Very high | Central PE; high mortality risk | | **Lobar PA** | 5–10 mm | Very high | Lobar PE; significant hemodynamic impact | | **Segmental PA** | 2–5 mm | High | Segmental PE; clinically important | | **Subsegmental PA** | <2 mm | Low | Difficult to assess; imaging artifact mimicry | **High-Yield:** Current guidelines (ACCP, ESC) recommend **NOT diagnosing PE based solely on subsegmental filling defects** because: 1. Interobserver agreement is poor 2. Artifact and motion can mimic thrombus 3. Clinical significance of isolated subsegmental PE is debated 4. False-positive rate is unacceptably high **Mnemonic: LSCM** — **Lobar, Segmental, Central, Main** are the reliable levels for PE diagnosis on CTPA. ### Clinical Implications - **Segmental or larger PE** → Diagnose and treat - **Isolated subsegmental PE** → Requires clinical correlation; consider D-dimer, repeat imaging, or clinical follow-up; do not treat empirically - **Negative CTPA (segmental level)** → PE excluded with high confidence **Clinical Pearl:** A patient with high clinical suspicion but negative segmental-level CTPA should undergo lower extremity ultrasound to detect DVT, which would support PE diagnosis despite negative CTPA. 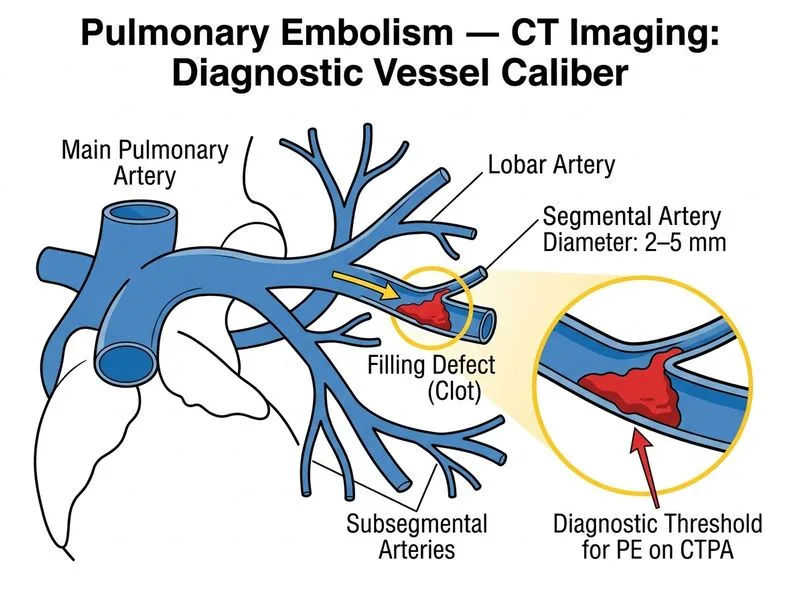
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.