## Clinical Presentation: Massive Pulmonary Embolism **Key Point:** This patient has a hemodynamically unstable, massive PE with imaging evidence of severe RV strain (RV/LV ratio 1.8, severely dilated RV) and biochemical evidence of myocardial injury (elevated troponin). Cardiogenic shock is present. ## Imaging Findings Indicating Massive PE | Finding | This Patient | Significance | |---------|--------------|---------------| | Location | Saddle embolism at bifurcation | Central, high-burden thrombus | | Extent | Bilateral PA involvement | Massive obstruction | | RV/LV ratio | 1.8 (>0.9 is abnormal) | Severe RV strain | | RV appearance | Severely dilated | Acute RV failure | | Hemodynamics | Shock (BP 88/56) | Acute decompensation | | Troponin | Markedly elevated | RV myocardial injury | ## Pathophysiology of Hemodynamic Collapse ```mermaid flowchart TD A["Large central PE"]:::outcome --> B["Acute RV afterload increase"]:::outcome B --> C["RV dilatation and failure"]:::outcome C --> D["Decreased LV preload"]:::outcome D --> E["Decreased cardiac output"]:::outcome E --> F["Cardiogenic shock"]:::urgent F --> G{"Intervention?"}:::decision G -->|Anticoagulation alone| H["High mortality"]:::urgent G -->|Reperfusion therapy| I["Improved survival"]:::action ``` ## Management of Massive PE with Shock **High-Yield:** Patients with hemodynamically unstable PE (shock, severe hypotension) and imaging evidence of massive PE require **urgent reperfusion therapy**, not observation. Options include: 1. **Thrombolysis** (alteplase, tenecteplase) — first-line if no contraindications 2. **Mechanical thrombectomy** — if thrombolysis contraindicated or failed 3. **ECMO** — as bridge to thrombectomy or definitive therapy **Clinical Pearl:** Anticoagulation alone in massive PE with shock has mortality rates exceeding 30%. Reperfusion therapy (thrombolysis or thrombectomy) reduces mortality to <5% in appropriate candidates. ## Immediate Actions 1. **Oxygen supplementation** — target SpO₂ >90% 2. **Fluid resuscitation** — cautious IV bolus (RV is preload-dependent in acute failure) 3. **Vasopressor support** — norepinephrine if hypotension persists 4. **Urgent transfer** — to a center with capability for thrombolysis or mechanical thrombectomy 5. **Initiate anticoagulation** — unfractionated heparin (UFH) preferred over LMWH for potential need for urgent reversal **Mnemonic:** **SHOCK-PE** = **S**upport oxygenation, **H**eparin (UFH), **O**xygen, **C**ardiac support (fluids/vasopressors), **K**eep patient moving (transfer), **P**erfusion therapy (thrombolysis/thrombectomy), **E**chocardiography (confirm RV strain). ## Why This Patient Needs Reperfusion Therapy **Key Point:** The presence of: - Hemodynamic instability (shock) - Massive central PE on imaging - Severe RV dysfunction (RV/LV 1.8) - Elevated troponin (myocardial injury) ...mandates **urgent reperfusion** as the standard of care. Waiting for spontaneous thrombolysis or observing with anticoagulation alone is associated with unacceptably high mortality. ## Thrombolysis Eligibility **Warning:** Thrombolysis is contraindicated if: - Active bleeding or recent major surgery - Recent stroke or intracranial pathology - Uncontrolled hypertension (>180/110) If contraindicated → mechanical thrombectomy is the alternative. [cite:Harrison 21e Ch 298; ESC Guidelines 2019 on PE] 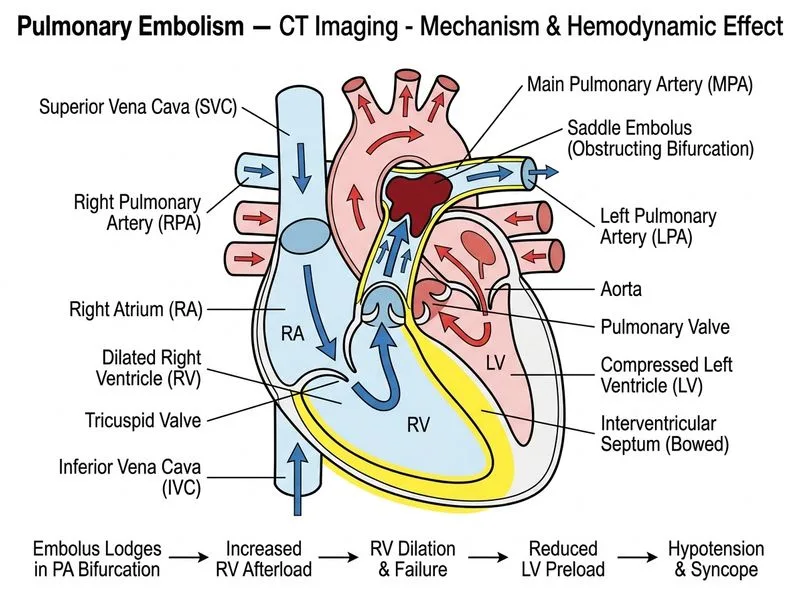
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.