## Clinical Diagnosis The patient presents with: - **Painless vision loss** in one eye over 3 weeks - **RAPD** (relative afferent pupillary defect) — indicates significant optic nerve or retinal pathology - **Optic disc pallor** and **flame-shaped hemorrhages** — classic for **central retinal vein occlusion (CRVO)** or **ischemic optic neuropathy (AION/PION)** - **Risk factor**: Diabetes mellitus (atherosclerosis, microvascular disease) The combination of optic disc pallor + flame-shaped hemorrhages + RAPD in a diabetic patient points to a **vascular occlusive event** at the level of the optic nerve or central retinal vasculature. The most appropriate investigation to **confirm the underlying vascular pathology** is direct retinal/optic nerve vascular imaging. **Key Point:** RAPD + optic disc pallor + flame-shaped hemorrhages + painless vision loss = retinal/optic nerve vascular emergency requiring structural vascular imaging, not merely functional testing. ## Investigation Rationale **Optical Coherence Tomography Angiography (OCTA)** is the most appropriate investigation because: 1. **Non-invasive vascular imaging**: Visualizes retinal and choroidal circulation without IV contrast injection — particularly important in diabetic patients with potential renal impairment 2. **High resolution structural detail**: Detects capillary dropout, ischemic zones, and vascular occlusion at the level of the optic nerve head and retina 3. **Confirms diagnosis directly**: Shows the site and extent of arterial or venous occlusion (central or branch), and differentiates CRVO from AION 4. **Guides management**: Identifies perfusion defects that may warrant urgent intervention (anti-VEGF, laser, thrombolysis) 5. **Modern first-line modality**: Per current ophthalmology guidelines, OCTA has largely replaced fluorescein angiography (FA) as the preferred first-line vascular imaging tool for retinal vascular occlusions — it is faster, non-invasive, and does not require IV contrast. **Note:** In settings where OCTA is unavailable, FA remains an acceptable alternative gold standard. ## Why the Other Options Are Incorrect | Investigation | Role | Why Not Best Here | |---|---|---| | **APD Testing with ND Filter (A)** | Quantifies RAPD severity | RAPD is already clinically evident; this confirms severity but does NOT identify the underlying pathology | | **Automated Perimetry (B)** | Documents functional visual field loss | Functional test only — does not diagnose the vascular cause or guide vascular management | | **OCTA (C)** | **Directly visualizes retinal/optic nerve vasculature; confirms occlusion** | **BEST ANSWER** | | **Carotid Duplex US (D)** | Screens for carotid stenosis as an embolic source | Relevant as a secondary systemic workup, but does NOT confirm the retinal/optic nerve pathology itself; it is an indirect upstream investigation | **Clinical Pearl (Harrison's / Kanski's Clinical Ophthalmology):** In retinal vascular occlusions and ischemic optic neuropathy, OCTA demonstrates areas of capillary non-perfusion and the precise location of occlusion with high sensitivity. This is superior to perimetry (functional only) and APD testing (confirms afferent defect but not its cause). Carotid duplex is part of the systemic workup for embolic disease but does not confirm the ocular diagnosis. **High-Yield:** The question asks for the investigation to **confirm the underlying pathology** — this requires direct structural vascular imaging of the eye (OCTA), not systemic vascular screening (carotid duplex) or functional testing (perimetry, APD quantification). 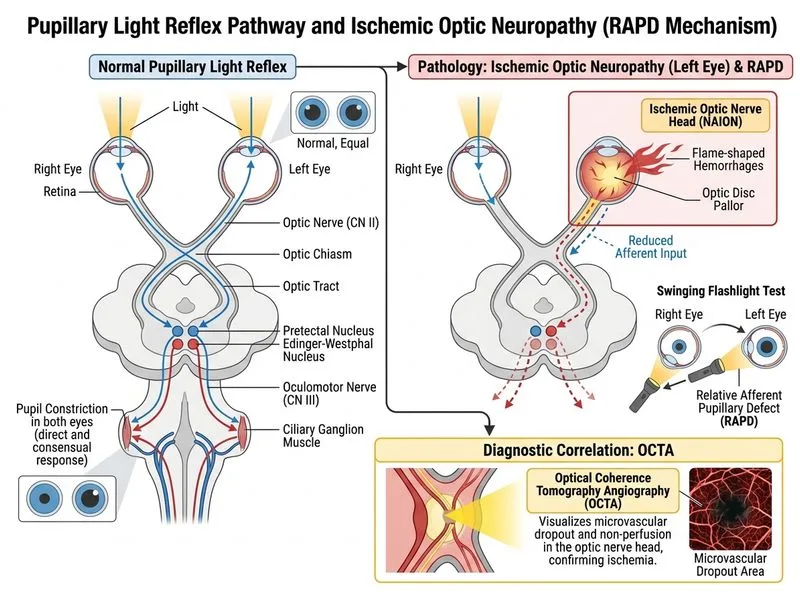
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.