## Clinical Presentation Analysis The patient presents with: 1. **Progressive vision loss in left eye** (3 weeks) 2. **Left pupil sluggish to direct light but brisk to consensual light** (pathognomonic for RAPD) 3. **Disc pallor and cotton-wool spots** on left fundoscopy 4. **Right pupil normal** 5. **Headaches** (suggesting demyelinating disease or inflammation) ## Understanding Relative Afferent Pupillary Defect (RAPD) **Key Point:** RAPD occurs when there is a **lesion of the afferent (sensory) pupillary pathway** — the optic nerve or retina — causing reduced light perception in that eye. The pupil appears to react better to consensual light (from the normal contralateral eye) than to direct light (from the affected eye). **High-Yield:** The **swinging flashlight test** is diagnostic: when light is swung from the normal eye to the affected eye, the affected pupil dilates (paradoxical dilation) because the consensual input from the normal eye is stronger than the direct input from the affected eye. ## Mechanism of RAPD in Optic Neuritis ```mermaid flowchart TD A[Optic neuritis<br/>inflammation of optic nerve]:::outcome --> B[Reduced light perception<br/>in affected eye]:::outcome B --> C[Afferent pupillary pathway<br/>compromised]:::outcome C --> D{Swinging flashlight test}:::decision D -->|Light on normal eye| E[Both pupils constrict<br/>via consensual reflex]:::action D -->|Light on affected eye| F[Both pupils dilate<br/>weak direct input]:::action E --> G[RAPD detected]:::outcome F --> G ``` **Clinical Pearl:** In optic neuritis, the pupil on the affected side reacts **sluggishly** to direct light but **briskly** to consensual light. This dissociation is the hallmark of RAPD. ## Differential Diagnosis: Pupillary Findings | Condition | Affected Pupil to Direct Light | Affected Pupil to Consensual Light | RAPD? | Associated Signs | |-----------|--------------------------------|-----------------------------------|-------|------------------| | **Optic neuritis (RAPD)** | Sluggish | Brisk | **Yes** | Vision loss, disc pallor, pain on eye movement | | Adie's tonic pupil | Slow (light-near dissociation) | Slow | No | Dilated pupil, normal vision, young female | | Third nerve palsy | Fixed, dilated | Fixed, dilated | No | Ptosis, ophthalmoplegia, normal vision | | Horner syndrome | Normal (miosis, not RAPD) | Normal | No | Miosis, ptosis, anhidrosis | **Mnemonic:** **RAPD = A**fferent **P**upillary **D**efect = optic nerve or retinal pathology (not efferent/motor pathway) ## Why This Is Optic Neuritis 1. **Age and sex:** 35-year-old woman (typical for demyelinating disease) 2. **Vision loss:** Progressive over 3 weeks (typical for optic neuritis) 3. **RAPD:** Pathognomonic for optic nerve lesion 4. **Disc findings:** Pallor and cotton-wool spots indicate optic nerve inflammation 5. **Headaches:** Suggest demyelinating disease (often associated with multiple sclerosis) 6. **Normal contralateral eye:** Rules out bilateral or systemic disease **High-Yield:** Optic neuritis is the **most common cause of RAPD** in young adults and is often the **first manifestation of multiple sclerosis** (especially in young women). ## Management Implications - **MRI brain + orbits:** To assess for demyelinating lesions and rule out MS - **Lumbar puncture:** CSF oligoclonal bands if MS suspected - **IV methylprednisolone:** Standard treatment for optic neuritis - **Long-term follow-up:** Monitor for development of MS 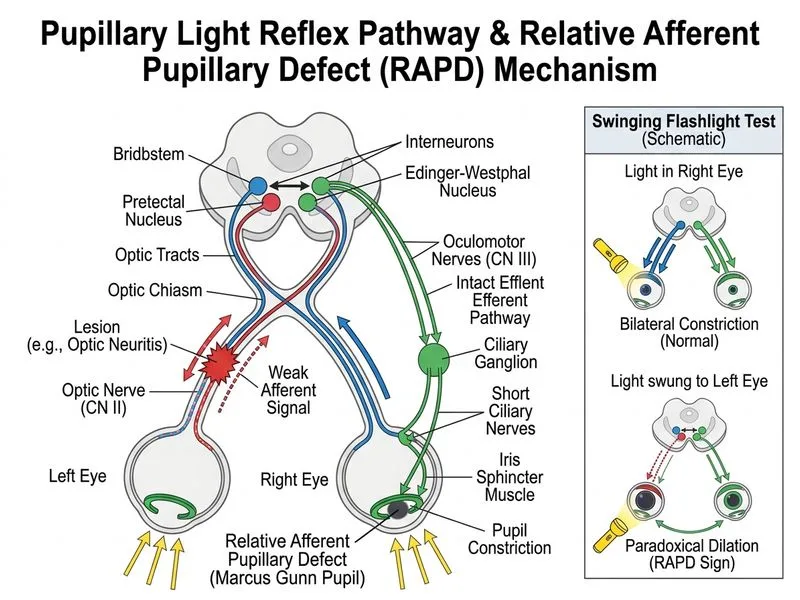
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.