## Acute Gout Flare During Urate-Lowering Therapy ### Clinical Scenario Analysis The patient experiences acute gout flare **despite successful reduction** of serum uric acid from 8.5 to 3.8 mg/dL. This paradoxical phenomenon is a well-recognized complication of initiating urate-lowering therapy (ULT) and is called **"flare of gout"** or **"mobilization flare."** ### Mechanism of Mobilization Flare ```mermaid flowchart TD A[Chronic hyperuricemia]:::outcome --> B[Tissue MSU crystal deposits]:::outcome B --> C[Stable deposits in cartilage, synovium]:::outcome D[Allopurinol initiated]:::action --> E[Serum uric acid ↓↓]:::action E --> F{Gradient reversal}:::decision F -->|Tissue UA > Serum UA| G[Mobilization of tissue deposits]:::urgent G --> H[Shedding of MSU crystals into synovial fluid]:::urgent H --> I[Acute inflammatory response]:::urgent I --> J[Gout flare]:::urgent K[Neutrophil activation by MSU crystals]:::action --> L[IL-1β, TNF-α release]:::action L --> M[Acute arthritis, fever, malaise]:::action ``` ### Pathophysiology **Key Point:** When serum uric acid drops rapidly, the concentration gradient between tissue deposits and serum reverses. Solid MSU crystals in cartilage and synovial tissue begin to dissolve and shed into the synovial fluid, triggering acute inflammation. 1. **Chronic state:** MSU crystals are stable in tissues when serum uric acid is persistently elevated (equilibrium). 2. **Rapid ULT initiation:** Serum uric acid drops sharply (3.8 mg/dL is well below saturation point). 3. **Gradient reversal:** Tissue urate concentration now exceeds serum concentration. 4. **Crystal mobilization:** Solid MSU deposits dissolve and crystals are shed into synovial fluid. 5. **Inflammatory cascade:** Resident macrophages and neutrophils phagocytose MSU crystals → NLRP3 inflammasome activation → IL-1β and TNF-α release → acute arthritis. ### High-Yield Facts **High-Yield:** Mobilization flare occurs in 30–80% of patients initiating ULT if prophylaxis is not given. It typically occurs within the first 2–6 weeks of therapy. **Mnemonic: FLARE-UP** — **F**ast reduction of urate → **L**iberation of tissue deposits → **A**cute **R**ecurrence of **E**rythema, **U**ric acid crystals → **P**ain paradox. ### Prevention and Management | Intervention | Mechanism | Timing | |---|---|---| | **Colchicine prophylaxis** | Inhibits NLRP3 inflammasome; blocks neutrophil migration | Start 1–2 weeks BEFORE ULT; continue 3–6 months | | **NSAIDs** | Anti-inflammatory; COX inhibition | Start BEFORE ULT; continue during flare | | **Low-dose corticosteroids** | Suppress IL-1β and TNF-α | Alternative if NSAID/colchicine contraindicated | | **Slow titration of ULT** | Gradual reduction minimizes gradient reversal | Increase allopurinol dose slowly (50–100 mg increments) | **Clinical Pearl:** The flare is a sign that ULT is working—it indicates mobilization of pathogenic crystal deposits. Continuing ULT while providing anti-inflammatory prophylaxis is the correct approach. ### Why Not the Other Options? - **Stevens–Johnson syndrome (SJS):** While allopurinol can rarely cause SJS (especially in HLA-B*5801 carriers), SJS presents with mucocutaneous blistering, not isolated arthritis with MSU crystals. - **Xanthine crystal deposition:** Xanthine is highly soluble and does not form crystals in joints, even with allopurinol use. Xanthinuria is asymptomatic. - **Hypersensitivity reaction:** Allopurinol hypersensitivity causes rash, fever, and hepatitis—not synovial MSU crystals. The presence of needle-shaped, negatively birefringent crystals is diagnostic of MSU, not a non-specific inflammatory response. ### Diagnostic Confirmation The finding of **needle-shaped, negatively birefringent crystals** in synovial fluid is pathognomonic for MSU gout and rules out other causes of acute arthritis during ULT initiation. 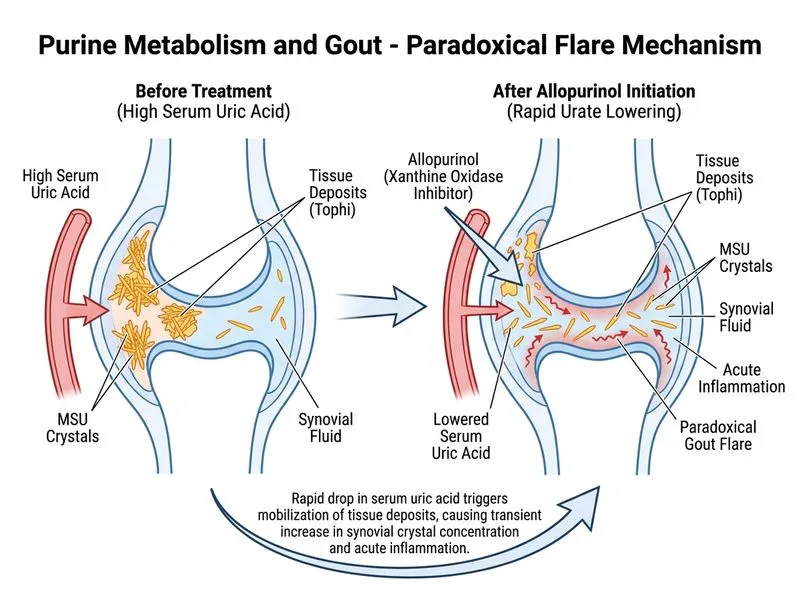
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.