## Management of Persistent Radial Nerve Deficit After 8 Weeks ### Clinical Context **Key Point:** At 8 weeks post-injury with **no clinical recovery**, the distinction between neuropraxia (which recovers by 3–4 weeks) and axonotmesis/neurotmesis becomes critical. Electrophysiological testing is now indicated to guide further management. ### Timeline of Nerve Recovery and Testing | Time Point | Clinical Status | Electrophysiological Finding | Action | |---|---|---|---| | 0–3 weeks | No recovery expected | Conduction block (neuropraxia) or no changes | Observe clinically | | 3–4 weeks | No clinical recovery | EMG shows denervation potentials | Order EMG/NCS | | 8 weeks | Persistent deficit | Complete conduction block or no motor units | EMG/NCS needed to classify injury severity | | 12+ weeks | No recovery | Chronic denervation | Consider surgical intervention | ### Role of EMG/NCS at 8 Weeks **High-Yield:** Electromyography and nerve conduction studies at 8 weeks serve to: 1. **Confirm complete vs. incomplete lesion** — complete block suggests neurotmesis or severe axonotmesis 2. **Assess denervation** — presence of fibrillation potentials indicates axonal loss 3. **Estimate prognosis** — preserved motor units suggest better recovery potential 4. **Guide surgical decision** — complete block with no motor recruitment favors surgical exploration ```mermaid flowchart TD A[Persistent radial nerve deficit at 8 weeks]:::outcome --> B[Obtain EMG/NCS]:::action B --> C{EMG/NCS findings?}:::decision C -->|Neuropraxia pattern: conduction block only| D[Continue observation, may recover up to 12 weeks]:::action C -->|Axonotmesis: denervation + some motor units| E[Observe further, repeat EMG at 12 weeks]:::action C -->|Neurotmesis: complete denervation, no motor recruitment| F[Surgical exploration and nerve repair]:::urgent E --> G{Recovery at 12 weeks?}:::decision G -->|Yes| H[Continue conservative management]:::action G -->|No| I[Surgical intervention]:::urgent ``` ### Why EMG/NCS Is Essential Now **Clinical Pearl:** At 8 weeks, clinical observation alone is insufficient. The patient has exceeded the typical recovery window for neuropraxia (3–4 weeks). EMG/NCS will: - Differentiate between conduction block (neuropraxia) and axonal loss (axonotmesis/neurotmesis) - Identify the presence or absence of motor unit action potentials (MUAPs) - Provide objective data to counsel the patient on prognosis ### Why Not Continue Conservative Management Alone? While spontaneous recovery can occur up to 12 weeks, **continuing without electrophysiological assessment is suboptimal**. EMG/NCS at 8 weeks provides critical prognostic information and may identify a complete lesion that requires surgical intervention before the "window of opportunity" for nerve repair closes (typically 12–18 months post-injury). ### Why Not Immediate Surgery? Surgical exploration without EMG/NCS confirmation is premature. If EMG shows neuropraxia or incomplete axonotmesis with some motor recruitment, surgery may not be indicated. Conversely, if EMG shows complete denervation, surgery becomes more justified. ### Why Not IVIG? Intravenous immunoglobulin has no role in traumatic peripheral nerve injuries. It may be used in autoimmune neuropathies (e.g., CIDP) but is not indicated here. 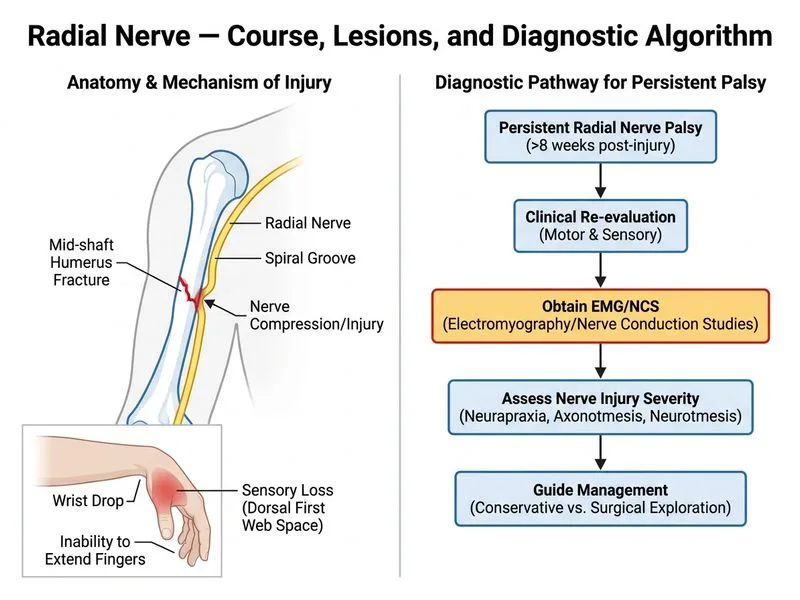
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.