## Radiation Dosimetry and Risk Assessment **Key Point:** Effective dose is measured in Sieverts (Sv) or millisieverts (mSv). A PET-CT study typically delivers 15–25 mSv, which is a high dose by diagnostic imaging standards but below the threshold for acute radiation syndrome (>1000 mSv). ## Dose Categories and Clinical Implications | Effective Dose (mSv) | Clinical Context | Cancer Risk | Acute Effects | |----------------------|------------------|-------------|---------------| | <1 | Annual background radiation | Negligible | None | | 1–10 | Diagnostic imaging (CT, PET-CT) | ~0.01–0.1% | None | | 10–100 | High-dose diagnostic imaging (PET-CT, multiple CTs) | ~0.1–1% | None | | >100 | Occupational/accidental exposure | >1% | Possible | | >1000 | Acute exposure | High | Acute radiation syndrome | **High-Yield:** The cancer risk from a single 25 mSv PET-CT is approximately **0.1% (1 in 1000)**, which is small in absolute terms but NOT negligible. This is why serial imaging must be justified. ## Radiation Risk Model **Mnemonic:** **BEIR VII model** — **B**iological **E**ffects of **I**onizing **R**adiation (7th report) provides the basis for cancer risk estimation in diagnostic radiology. For a 62-year-old man exposed to 25 mSv: - Lifetime attributable cancer risk ≈ 0.1% (age-dependent; older patients have lower lifetime risk than younger patients) - This is a small but measurable increase above background cancer incidence ## Clinical Decision-Making: Justification vs. Risk ```mermaid flowchart TD A[Patient requires staging/follow-up imaging]:::outcome --> B{Is the diagnostic question critical?}:::decision B -->|Yes, high clinical impact| C[Proceed with imaging]:::action B -->|No, low clinical impact| D[Defer or use alternative modality]:::action C --> E{Is this the first or repeat study?}:::decision E -->|First study| F[Document indication and dose]:::action E -->|Repeat study| G{Can MRI or ultrasound substitute?}:::decision G -->|Yes| H[Use non-ionizing modality]:::action G -->|No| I[Justify repeat imaging; document cumulative dose]:::action F --> J[Counsel patient on small but real cancer risk]:::action H --> J I --> J ``` **Clinical Pearl:** In oncology patients (like this myeloma patient), the benefit of accurate staging and treatment planning typically outweighs the small cancer risk from a single PET-CT. However, cumulative dose from serial imaging over years becomes a concern and should prompt consideration of alternative modalities (MRI, ultrasound) for follow-up when appropriate. ## Why This Study Is Justified Despite the Risk 1. **Indication:** Staging of multiple myeloma is critical for treatment planning and prognosis. 2. **No alternative:** PET-CT is the gold standard for myeloma staging; MRI and ultrasound cannot replace it for this indication. 3. **Benefit >> Risk:** The diagnostic benefit (accurate staging, treatment guidance, prognostic information) far exceeds the small cancer risk (~0.1%). 4. **Cumulative concern:** If the patient requires repeat PET-CTs annually, cumulative dose becomes a concern, and alternative modalities should be explored for follow-up. **Warning:** Do NOT confuse effective dose (mSv) with acute radiation syndrome threshold. A 25 mSv diagnostic study causes no acute effects; acute radiation syndrome requires >1000 mSv in a short time frame. [cite:BEIR VII Report, National Academies Press 2006; ICRP Publication 103, 2007] 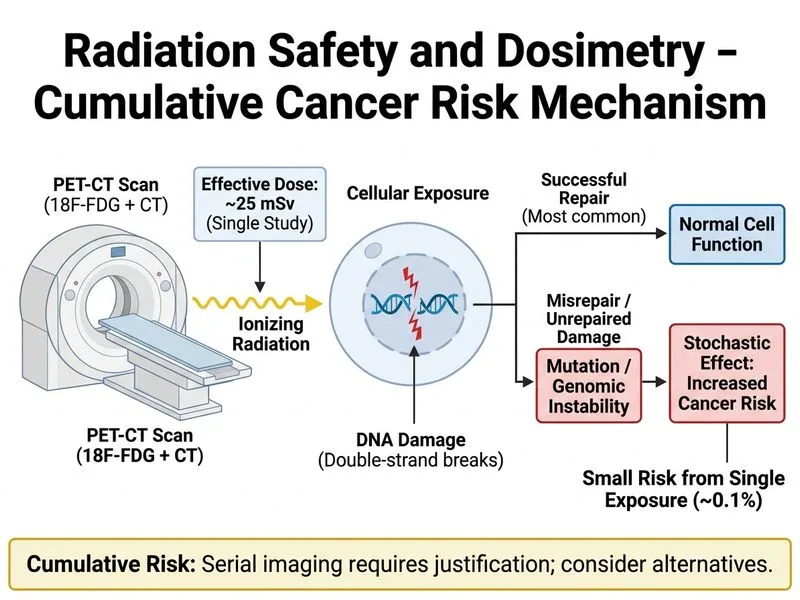
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.