## Clinical Context: Acute Bronchospasm in a COPD Patient on Atenolol This patient presents with acute bronchospasm while on atenolol (a β₁-selective blocker) for hypertension. The immediate priority is bronchodilation, and the long-term management of atenolol must be considered carefully. ## Immediate Management: Albuterol Nebulizer **Key Point:** Albuterol (salbutamol) is a **β₂-selective agonist** and is the **first-line agent** for acute bronchospasm in COPD. It should be administered immediately via nebulizer regardless of concurrent β-blocker use. - Onset: 5–15 minutes via nebulizer - Mechanism: Activates β₂-receptors on bronchial smooth muscle → bronchodilation - Even in the presence of a β₁-selective blocker, albuterol can overcome partial β₂-blockade and provide effective bronchodilation ## β₁-Selective Blockers in COPD: The Nuanced Reality **High-Yield:** Current evidence and major guidelines (GOLD, ESC/ERS) recognize that **β₁-selective blockers at low-to-moderate doses (e.g., atenolol 50 mg, metoprolol, bisoprolol) are NOT absolutely contraindicated in COPD** when there is a compelling cardiac indication (e.g., heart failure, post-MI, hypertension). This is a critical distinction from non-selective β-blockers. | β-Blocker Type | Bronchospasm Risk | Use in COPD | |---|---|---| | Non-selective (propranolol) | Very high | Contraindicated | | β₁-selective (atenolol 50 mg, metoprolol, bisoprolol) | Low–moderate | **Relative contraindication; may be continued with monitoring** | At standard doses (atenolol 50 mg), the β₁:β₂ selectivity ratio (~10:1) means that β₂-mediated bronchodilation is largely preserved. Abruptly discontinuing atenolol in a hypertensive patient without a clear plan is not the immediate priority during an acute bronchospasm episode. ## Why Option C Is Incorrect Option C recommends **discontinuing atenolol and switching to a calcium channel blocker** as part of the immediate next step. While long-term reassessment of atenolol is reasonable, **abrupt discontinuation of a β-blocker** carries risks (rebound hypertension, tachycardia) and is NOT the immediate priority in acute bronchospasm management. The acute step is bronchodilation; medication reconciliation follows stabilization. ## Why Option D Is Correct **Clinical Pearl:** Administering albuterol via nebulizer addresses the acute bronchospasm immediately. Continuing atenolol at this dose (50 mg) is defensible because: 1. β₁-selectivity at this dose minimizes β₂-blockade 2. Abrupt discontinuation is not indicated emergently 3. The cardiac benefit (blood pressure control) is maintained 4. Albuterol effectively counteracts any residual β₂-blockade This reflects the **best next step** in the acute setting — treat the bronchospasm first, then reassess antihypertensive therapy electively. ## Why Other Options Are Incorrect - **Option A:** Ipratropium alone is insufficient for acute bronchospasm; albuterol is the primary agent - **Option B:** Theophylline IV is not first-line; abrupt atenolol cessation is not indicated emergently **Mnemonic:** In acute bronchospasm — **"Treat the airway first, then reassess the heart meds."** [cite: GOLD Guidelines 2023; Harrison's Principles of Internal Medicine 21e Ch 256; KD Tripathi Essentials of Medical Pharmacology 8e Ch 10; Salpeter SR et al., Ann Intern Med 2002 — cardioselective β-blockers in COPD] 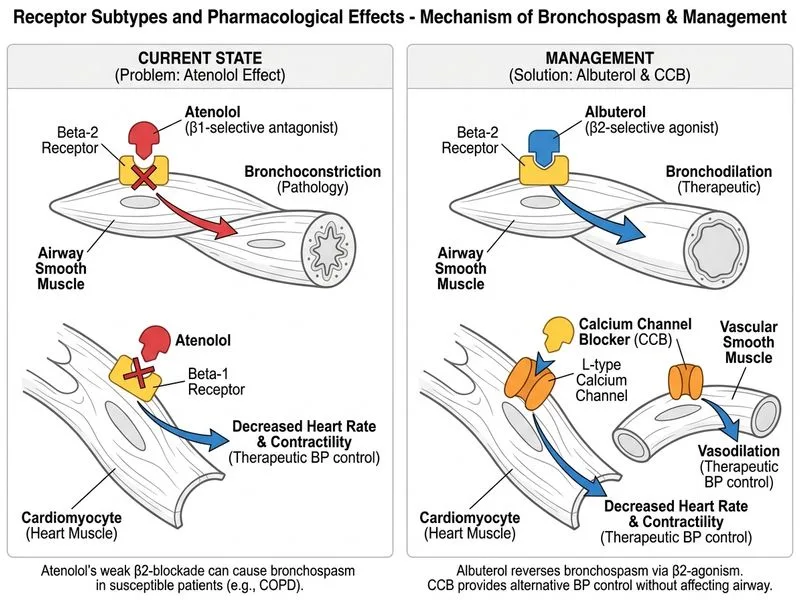
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.