## Clinical Diagnosis **Key Point:** This is Respiratory Distress Syndrome (RDS) — also called Hyaline Membrane Disease — in a preterm infant with classic presentation and radiological findings. ### Diagnostic Criteria Met | Feature | Finding | Significance | |---------|---------|---------------| | Gestational age | 28 weeks | High risk for surfactant deficiency | | Birth weight | 1200 g | VLBW — increased RDS incidence | | Clinical signs | Grunting, nasal flaring, retractions | Increased work of breathing | | CXR pattern | Ground-glass + air bronchograms | Pathognomonic for RDS | | Blood gas | pH 7.28, PaCO₂ 52, PaO₂ 58 on 60% FiO₂ | Respiratory acidosis + hypoxemia | | Antenatal steroids | Not given | No neuroprotection or lung maturity benefit | ### Why Surfactant + Mechanical Ventilation? **High-Yield:** RDS is caused by **surfactant deficiency** in preterm lungs. Surfactant reduces surface tension, preventing alveolar collapse at end-expiration. Without it, the work of breathing increases exponentially. 1. **Respiratory acidosis** (PaCO₂ 52) indicates **ventilatory failure** — CPAP alone is insufficient. 2. **Hypoxemia despite 60% FiO₂** suggests significant intrapulmonary shunting. 3. **Exogenous surfactant** (e.g., poractant alfa, beractant) is the definitive treatment and dramatically improves oxygenation and compliance. 4. **Mechanical ventilation** is required to deliver surfactant and support gas exchange until endogenous surfactant production increases (typically by day 3–5). ### Management Algorithm ```mermaid flowchart TD A[Preterm infant with RDS signs]:::outcome --> B{Respiratory acidosis or severe hypoxemia?}:::decision B -->|Yes| C[Intubate for airway protection]:::action C --> D[Administer exogenous surfactant]:::action D --> E[Mechanical ventilation]:::action E --> F[Monitor blood gases, wean as tolerated]:::action B -->|No| G[Trial of CPAP + supplemental O₂]:::action G --> H{Improvement?}:::decision H -->|Yes| I[Continue CPAP]:::action H -->|No| C ``` **Clinical Pearl:** The "INSURE" technique (Intubate, give Surfactant, extUbate to CPAP) is used in some centres for mild-moderate RDS, but this infant's respiratory acidosis mandates full mechanical ventilation support. **Mnemonic: SURFACTANT DEFICIENCY** — **S**urfactant deficiency, **U**nder 32 weeks, **R**etractions, **F**iO₂ requirement, **A**ir bronchograms, **C**ompliance ↓, **T**achypnea, **A**cidosis, **N**asal flaring, **T**emperature instability. [cite:Nelson Textbook of Pediatrics 21e Ch 102] 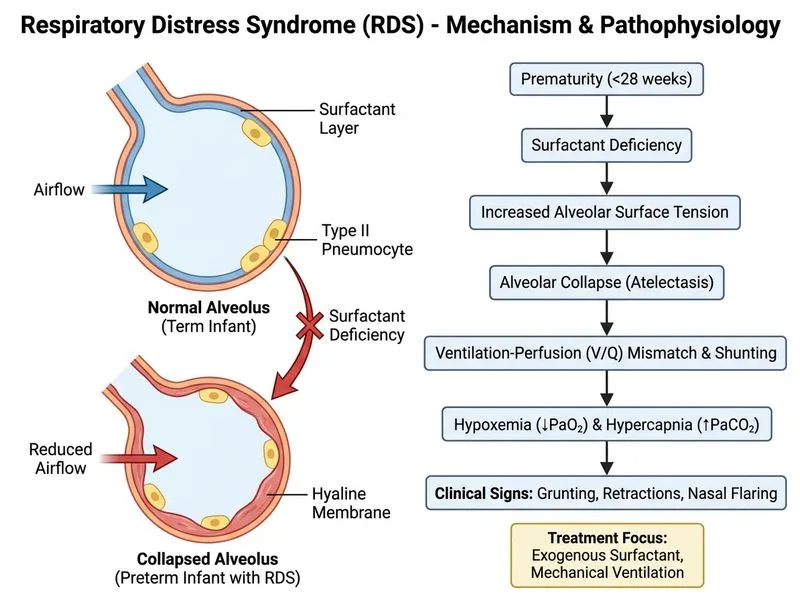
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.