## Clinical Diagnosis **Key Point:** This is **Transient Tachypnea of the Newborn (TTN)**, not RDS. The clinical and radiological features are distinct and have different pathophysiology. ### Differential Diagnosis: TTN vs RDS | Feature | TTN | RDS | |---------|-----|-----| | **Gestational age** | ≥34 weeks (usually ≥35) | <32 weeks | | **Antenatal steroids** | Does not prevent TTN | Prevents RDS | | **Onset** | Within 2–6 hours | Within 1–2 hours | | **Respiratory rate** | 60–120/min (mild tachypnea) | Often >60, progressive | | **Retractions** | Mild to moderate | Severe, increasing | | **CXR pattern** | Hyperinflation, perihilar streaking, fissural fluid | Ground-glass, air bronchograms | | **Blood gas** | Mild respiratory alkalosis or normal | Respiratory acidosis | | **Course** | Self-limited, resolves in 24–72 hours | Worsens without surfactant | | **Treatment** | Observation, supplemental O₂ as needed | Surfactant + mechanical ventilation | ### Pathophysiology of TTN **High-Yield:** TTN is caused by **delayed clearance of fetal lung fluid** (amniotic fluid) from the alveoli. Normally, labour contractions and thoracic compression during vaginal delivery expel ~80% of fetal lung fluid. In this case: 1. **Caesarean delivery without labour** (implied by gestational diabetes risk) = inadequate thoracic compression. 2. **Maternal hyperglycemia** may impair fetal lung fluid reabsorption via Na⁺-K⁺-ATPase. 3. **Retained fluid** causes air trapping (hyperinflation) and ventilation-perfusion mismatch. 4. **Self-limited:** Fluid is gradually reabsorbed via lymphatic and vascular channels over 24–72 hours. ### Why NOT RDS? **Clinical Pearl:** This infant **received antenatal corticosteroids**, which accelerate fetal lung maturation and surfactant production. At 34 weeks with steroids, RDS is unlikely. Additionally: - **Ground-glass CXR** is absent; instead, there is **hyperinflation with perihilar streaking** (classic TTN). - **Blood gas is near-normal** (pH 7.34, PaCO₂ 38); RDS typically presents with respiratory acidosis. - **Mild retractions** and **moderate tachypnea** are consistent with TTN, not severe RDS. ### Management Algorithm ```mermaid flowchart TD A[Tachypneic newborn at 34+ weeks]:::outcome --> B{Antenatal steroids given?}:::decision B -->|Yes| C{CXR pattern?}:::decision B -->|No| D{CXR pattern?}:::decision C -->|Hyperinflation + perihilar streaking| E[TTN]:::outcome C -->|Ground-glass + air bronchograms| F[RDS]:::outcome D -->|Hyperinflation + perihilar streaking| G[TTN likely, but RDS possible]:::outcome D -->|Ground-glass + air bronchograms| F E --> H[Observation, supplemental O₂ PRN]:::action F --> I[Surfactant + mechanical ventilation]:::action ``` **Mnemonic: TTN FLUID** — **T**ransient, **T**achypnea, **N**ewborn, **F**luid retention, **L**ate preterm/term, **U**ncomplicated delivery, **I**mprovement in 24–72 hours, **D**elay in fetal lung fluid clearance. [cite:Nelson Textbook of Pediatrics 21e Ch 102] 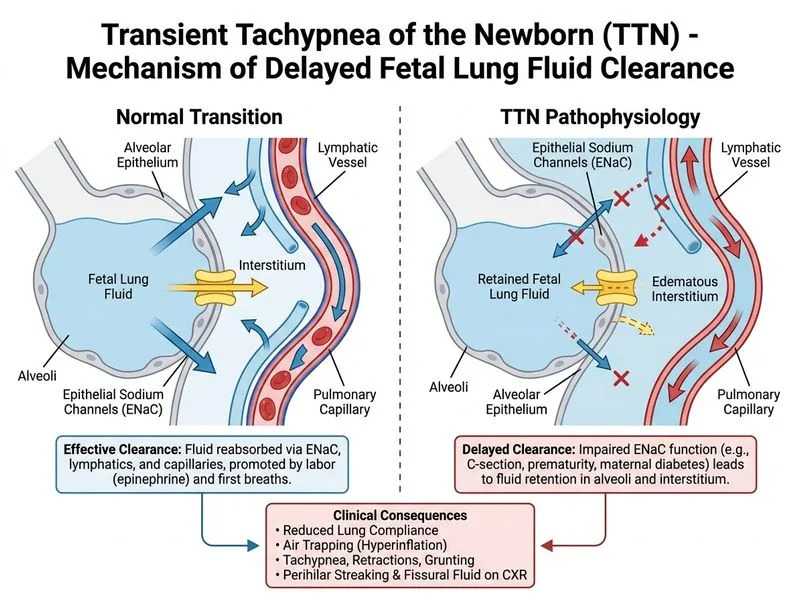
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.