## RDS vs TTN: Discriminating by Gas Exchange Severity ### The Pathophysiology Divide **Key Point:** RDS causes **severe ventilation-perfusion (V/Q) mismatch and intrapulmonary shunting** due to surfactant deficiency and alveolar collapse. TTN causes **mild-to-moderate V/Q mismatch** from retained fetal fluid, which is self-limited. ### Arterial Blood Gas Patterns — The Reliable Discriminator | Parameter | RDS | TTN | |-----------|-----|-----| | **PaO₂** | <50 mmHg on FiO₂ ≥0.60 (severe hypoxemia) | >60 mmHg on room air or low FiO₂ | | **PaCO₂** | >55 mmHg (hypercapnia from poor ventilation) | 35–45 mmHg (normal or mild elevation) | | **pH** | <7.25 (respiratory acidosis) | >7.30 (normal or mild acidosis) | | **A-a gradient** | Markedly elevated (>200 mmHg on FiO₂ 1.0) | Mildly elevated (<100 mmHg) | | **Response to O₂** | Poor; refractory hypoxemia | Good; rapid improvement | ### Why Severity of Gas Exchange is the Best Discriminator **High-Yield:** The **severity of hypoxemia and hypercapnia** reflects the **degree of alveolar collapse and shunting**: - RDS: Surfactant deficiency → widespread alveolar atelectasis → massive shunt → severe hypoxemia + CO₂ retention - TTN: Retained fluid → transient air trapping → mild V/Q mismatch → mild-to-moderate hypoxemia, normal CO₂ In the clinical scenario: - RDS infant: PaO₂ 45 mmHg on FiO₂ 0.80 (severe refractory hypoxemia) + PaCO₂ 65 mmHg (hypercapnia) → classic RDS - TTN infant: Normal ABG on room air → TTN ### Why the Other Options Are Not Reliable Discriminators 1. **Grunting and nasal flaring** — Both are signs of respiratory distress and occur in both RDS and TTN. Not specific. 2. **Gestational age + maternal risk factors** — While RDS is more common in preterm infants without antenatal steroids, TTN can occur in preterm infants, and RDS can occur in term infants (e.g., maternal diabetes, cesarean delivery). Risk factors guide suspicion but do not definitively discriminate. 3. **Response to surfactant within 30 minutes** — This is a **treatment response**, not a diagnostic feature. Some RDS infants respond dramatically; others have a delayed response. TTN does not receive surfactant, so this cannot be used prospectively for diagnosis. ### Clinical Pearl **Mnemonic: "RDS = Refractory hypoxemia + CO₂ retention; TTN = Mild hypoxemia, normal CO₂"** When you see a tachypneic newborn: - Check the ABG immediately. If **PaO₂ <50 on FiO₂ ≥0.60 AND PaCO₂ >55** → RDS → Surfactant - If **PaO₂ >60 on room air AND PaCO₂ normal** → TTN → Supportive care ### Mechanism: Why RDS Causes Severe Gas Exchange Impairment ```mermaid flowchart TD A[Surfactant Deficiency]:::outcome --> B[Increased Surface Tension]:::outcome B --> C[Alveolar Collapse at End-Expiration]:::outcome C --> D[Intrapulmonary Shunting<br/>Perfused but Not Ventilated]:::urgent D --> E[Severe Hypoxemia<br/>Refractory to O₂]:::urgent C --> F[Reduced Lung Compliance]:::outcome F --> G[Increased Work of Breathing]:::outcome G --> H[CO₂ Retention<br/>Hypercapnia]:::urgent E --> I[RDS Diagnosis]:::action H --> I ``` [cite:Harrison Principles of Internal Medicine 21e Ch 297] 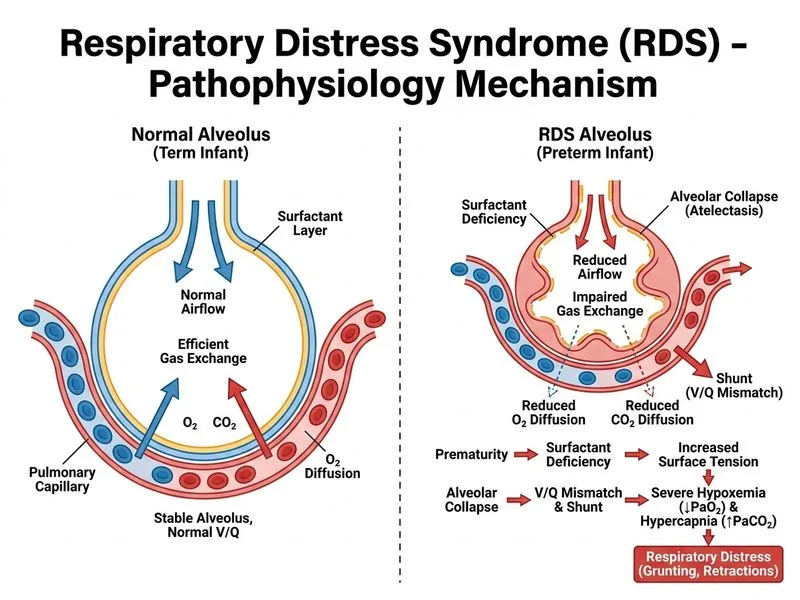
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.