## Clinical Diagnosis: Respiratory Distress Syndrome (RDS) ### Key Presentation **Key Point:** RDS (also called hyaline membrane disease) is the most common cause of respiratory distress in preterm neonates, caused by surfactant deficiency. ### Pathophysiology 1. Surfactant production begins at ~24 weeks gestation but is insufficient before 34–35 weeks 2. Lack of surfactant → increased alveolar surface tension → alveolar collapse at end-expiration (atelectasis) 3. Results in ventilation-perfusion mismatch and hypoxemia ### Clinical Features Supporting RDS | Feature | RDS | TTN | MAS | PPHN | |---------|-----|-----|-----|------| | **Gestational age** | <34 weeks (very preterm) | Term/near-term | Term | Term/near-term | | **Onset** | Within 1–2 hours | 6–12 hours | Variable | | **Chest X-ray** | Ground-glass, air bronchograms | Hyperinflation, fluid lines | Hyperinflation, patchy infiltrates | Normal or hyperinflation | | **Risk factors** | Prematurity, no steroids | Maternal diabetes, C-section | Meconium-stained fluid | Aspiration, sepsis, CDH | | **Response to CPAP/ventilation** | Good | Good | Variable | Poor (requires iNO) | ### Why This Case = RDS **High-Yield:** The combination of **extreme prematurity (28 weeks) + absence of antenatal steroids + early onset (2 hours) + ground-glass CXR + respiratory acidosis** is pathognomonic for RDS. **Clinical Pearl:** Antenatal corticosteroids (betamethasone or dexamethasone) accelerate fetal lung maturity and reduce RDS risk by ~50% even at 28 weeks. This mother's lack of steroid exposure is a critical risk factor. ### Management 1. Exogenous surfactant replacement (INSURE or LISA technique) 2. Gentle ventilation (permissive hypercapnia) 3. Supportive care: temperature control, fluid/electrolyte management 4. Antibiotics if sepsis suspected [cite:Nelson Textbook of Pediatrics 21e Ch 102] 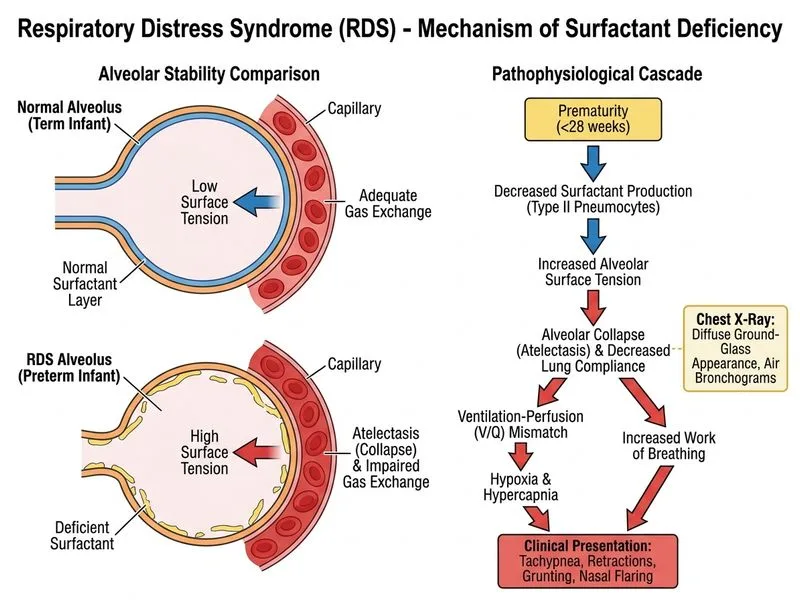
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.