## Diagnosis and Clinical Context **Key Point:** This is a classic presentation of Respiratory Distress Syndrome (RDS) in a preterm infant — the reticulogranular pattern with air bronchograms on chest X-ray is pathognomonic for surfactant deficiency. ### Pathophysiology of RDS 1. **Surfactant deficiency** — At 28 weeks, fetal lungs have immature type II pneumocytes; surfactant production is minimal 2. **Increased surface tension** — Without surfactant, alveolar collapse occurs at end-expiration (atelectasis) 3. **Increased work of breathing** — Leads to tachypnea, retractions, and metabolic acidosis 4. **Ventilation-perfusion mismatch** — Results in hypoxemia and hypercapnia ### Management Strategy **High-Yield:** Modern RDS management follows the **INSURE principle** (Intubate, Surfactant, Extubate to CPAP) or **LISA approach** (Less Invasive Surfactant Administration): | Step | Rationale | |------|----------| | **CPAP initiation** | Maintains positive end-expiratory pressure (PEEP); recruits collapsed alveoli; reduces work of breathing | | **Exogenous surfactant** | Replaces deficient endogenous surfactant; reduces surface tension; improves lung compliance | | **Oxygen titration** | Target SpO₂ 90–95% (avoid hyperoxia → retinopathy of prematurity) | | **Supportive care** | Temperature control, fluid/electrolyte management, monitoring | **Clinical Pearl:** CPAP is the first-line non-invasive respiratory support in RDS. Intubation and mechanical ventilation are reserved for: - Failure to improve on CPAP (persistent severe acidosis, apnea, exhaustion) - Surfactant administration (if not using LISA technique) - Severe hypoxemia refractory to CPAP + supplemental oxygen ### Why Option 1 (CPAP + Surfactant) Is Correct This infant has moderate RDS (pH 7.28, PaCO₂ 52, PaO₂ 48 on FiO₂ 0.60) with clear radiographic evidence of surfactant deficiency. The current guidelines (AAP, ACOG, NRSG) recommend: 1. **Initiate CPAP** (typically 5–7 cm H₂O) as first-line support 2. **Administer exogenous surfactant** (e.g., poractant alfa, beractant) — improves oxygenation and reduces need for mechanical ventilation 3. **Avoid intubation unless necessary** — reduces ventilator-associated lung injury and BPD risk 4. **Supportive measures** — thermal regulation, IV fluids, glucose monitoring The infant's respiratory status is not yet critical (not in severe acidosis, not apneic); CPAP with surfactant offers the best risk-benefit profile. [cite:Nelson Textbook of Pediatrics 21e Ch 101] 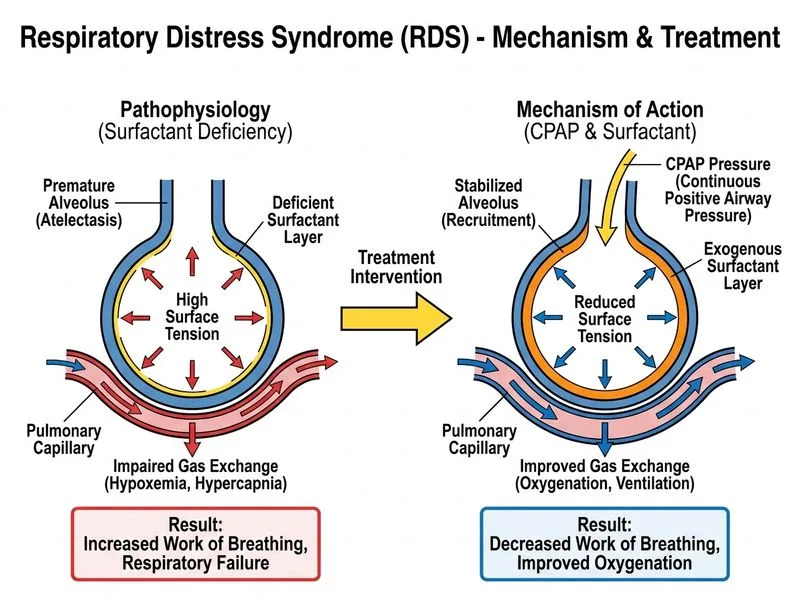
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.