## Differential Diagnosis and Clinical Analysis ### Key Clinical Features Pointing to TTN **High-Yield:** The chest X-ray finding of **bilateral hyperinflation with perihilar streaking and fluid in the fissures** ("wet lung" appearance) is pathognomonic for **Transient Tachypnea of the Newborn (TTN)**, NOT RDS. | Feature | RDS | TTN | |---------|-----|-----| | **Gestational age** | <32 weeks (surfactant deficiency) | 34–37 weeks or term (delayed fluid clearance) | | **Risk factors** | Prematurity, maternal diabetes (impaired surfactant synthesis) | Maternal diabetes, cesarean delivery, perinatal asphyxia | | **Chest X-ray** | Reticulogranular pattern, air bronchograms, ground-glass | Hyperinflation, perihilar streaking, fluid in fissures, "wet lung" | | **Onset** | Birth to 2 hours | 2–12 hours (delayed presentation) | | **Course** | Progressive without surfactant | Self-limited; resolves in 48–72 hours | | **Surfactant response** | Dramatic improvement | No response (not surfactant-deficient) | ### Why This Infant Has TTN, Not RDS **Key Point:** Although this is a preterm infant (34 weeks) with maternal diabetes, several factors favor TTN: 1. **Antenatal corticosteroids completed 3 days ago** — Betamethasone accelerates fetal lung maturity and surfactant production; by 34 weeks + steroid effect, surfactant is likely adequate 2. **Chest X-ray pattern** — Hyperinflation with perihilar streaking and fissural fluid is classic TTN, NOT the reticulogranular pattern of RDS 3. **Delayed onset** — Symptoms at 4 hours (not immediate at birth) is typical for TTN; RDS usually presents within 2 hours 4. **Maternal diabetes** — Increases risk of TTN by impairing fetal fluid resorption and delaying lung fluid clearance ### Pathophysiology of TTN ```mermaid flowchart TD A[Delayed clearance of fetal lung fluid]:::outcome --> B[Retained fluid in alveoli and interstitium]:::outcome B --> C[Increased airway resistance]:::outcome C --> D[Air trapping and hyperinflation]:::outcome D --> E[Tachypnea, grunting, retractions]:::outcome E --> F[Self-limited; resolves in 48-72 hours]:::action G[Risk factors: maternal diabetes, cesarean delivery, perinatal asphyxia]:::decision --> A ``` **Clinical Pearl:** TTN is a diagnosis of **exclusion** — rule out infection, pneumonia, and RDS first. However, the classic radiographic appearance (wet lung) and clinical context make TTN the most likely diagnosis here. ### Management of TTN **Mnemonic: CPAP-O** — CPAP, Oxygen titration, Positioning, Observation 1. **CPAP (5–7 cm H₂O)** — Maintains positive pressure; helps recruit fluid-filled alveoli 2. **Supplemental oxygen** — Titrate to SpO₂ 90–95% 3. **Supportive care** — IV fluids, glucose monitoring, thermal regulation 4. **Observation** — Most cases resolve within 48–72 hours without surfactant 5. **Avoid unnecessary antibiotics** — If no signs of infection (normal WBC, negative cultures) **Warning:** Do NOT give surfactant for TTN — it is not surfactant-deficient and surfactant will not improve outcomes. This is a common mistake in exam questions. [cite:Nelson Textbook of Pediatrics 21e Ch 101] 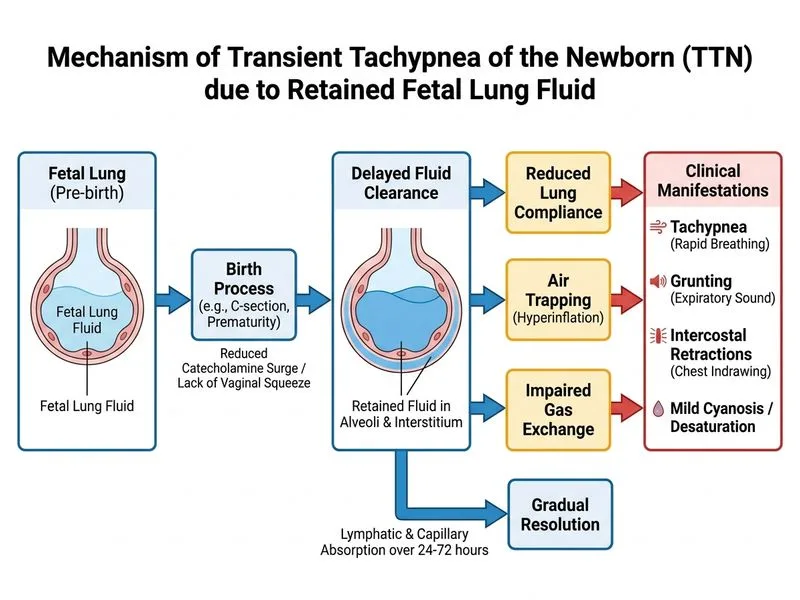
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.