## Clinical Diagnosis This is a classic presentation of Respiratory Distress Syndrome (RDS) in a preterm infant (28 weeks gestation). The clinical triad of grunting, retractions, and nasal flaring, combined with ground-glass opacification on chest X-ray and hypoxemia with hypercapnia, confirms RDS due to surfactant deficiency. ## Pathophysiology of RDS Surfactant production begins around 24 weeks gestation but is inadequate until ~34–35 weeks. Without surfactant: - Alveolar surface tension increases → alveolar collapse (atelectasis) - Compliance decreases → increased work of breathing - Ventilation–perfusion mismatch → hypoxemia and hypercapnia ## Management Algorithm ```mermaid flowchart TD A[Preterm infant with RDS signs + CXR ground-glass]:::outcome --> B{Respiratory support needed?}:::decision B -->|Yes| C[CPAP as first-line respiratory support]:::action C --> D{Response adequate?}:::decision D -->|Yes| E[Continue CPAP + Surfactant]:::action D -->|No| F[Intubate and give surfactant]:::action E --> G[Wean CPAP as clinical improvement occurs]:::action F --> G ``` ## Why CPAP + Surfactant is Correct **Key Point:** CPAP (Continuous Positive Airway Pressure) is the first-line non-invasive respiratory support for RDS in preterm infants. It: - Maintains positive end-expiratory pressure (PEEP) to prevent alveolar collapse - Reduces work of breathing - Allows spontaneous breathing - Minimizes ventilator-induced lung injury (VILI) **High-Yield:** Exogenous surfactant replacement is the definitive treatment for RDS. Modern approach is "INSURE" (Intubate–Surfactant–Extubate) or "CPAP-first" strategy: - Administer surfactant via thin endotracheal tube or laryngeal mask airway - Extubate immediately back to CPAP if possible - This reduces need for prolonged mechanical ventilation and decreases BPD risk **Clinical Pearl:** In this case, the infant has moderate-to-severe RDS (PaO₂ 48 mmHg on room air, pH 7.28). CPAP alone may not be sufficient; surfactant administration is indicated. The combination of CPAP + surfactant is the standard of care and offers the best balance of efficacy and lung protection. ## Why Other Options Are Suboptimal | Option | Why Wrong | |--------|----------| | Antenatal corticosteroids + observation | Antenatal steroids accelerate fetal lung maturity but are given *before* delivery; they cannot be given now. Observation alone will lead to progressive hypoxemia and respiratory failure. | | Immediate intubation without surfactant | Intubation without surfactant leaves the underlying deficiency untreated. Mechanical ventilation alone increases VILI risk and BPD. | | High-flow nasal cannula + defer intervention | High-flow nasal cannula provides insufficient support for this degree of RDS. Deferring surfactant allows progressive atelectasis and deterioration. | **Warning:** Do not confuse CPAP-first strategy with "no surfactant." CPAP is the respiratory support modality; surfactant is the pharmacological treatment. Both are needed in moderate-to-severe RDS. 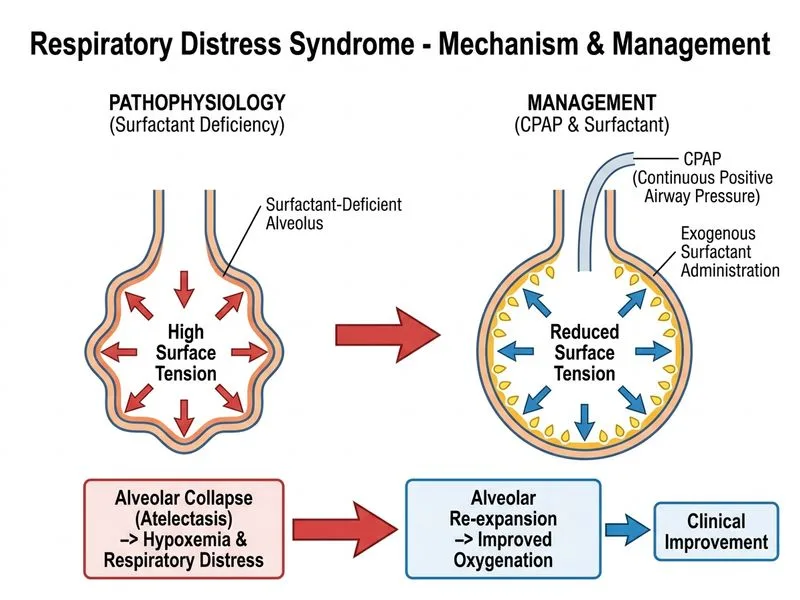
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.