## Diagnosis: Rhegmatogenous Retinal Detachment ### Clinical Presentation This patient presents with the classic triad of rhegmatogenous retinal detachment (RRD): 1. **Sudden floaters** — vitreous haemorrhage or pigment from the break 2. **Photopsia (flashing lights)** — vitreous traction on the retina 3. **Visual field defect** — the grey, elevated retinal fold extending from the optic disc ### Key Risk Factors Present - **High myopia (−12 D)** — causes posterior staphyloma and retinal thinning - **Lattice degeneration** — area of retinal thinning predisposed to breaks - **Acute symptom onset** — typical of RRD, not gradual as in tractional or exudative forms ### Fundoscopic Findings **Key Point:** The presence of **retinal breaks at the edge of the detachment** is pathognomonic for rhegmatogenous detachment. The grey, elevated appearance is due to the detached neurosensory retina separating from the retinal pigment epithelium (RPE). ### Pathophysiology ```mermaid flowchart TD A[Retinal break in high myope]:::outcome --> B[Vitreous fluid seeps through break]:::action B --> C[Fluid accumulates subretinally]:::action C --> D[Separation of neurosensory retina from RPE]:::outcome D --> E[Loss of photoreceptor function]:::urgent E --> F[Vision loss if macula involved]:::urgent ``` ### Differential Distinction | Feature | RRD | Tractional | Exudative | | --- | --- | --- | --- | | **Retinal breaks** | Present | Absent | Absent | | **Onset** | Sudden | Gradual | Gradual | | **Vitreous inflammation** | Mild/none | None | Moderate/severe | | **Causes** | Myopia, lattice, PVD | Proliferative DR, PVR | Uveal melanoma, inflammation | | **Detachment edge** | Irregular | Regular, smooth | Smooth, gentle slope | **High-Yield:** In a myopic patient with acute floaters, photopsia, and a retinal break visible on fundoscopy, RRD is the diagnosis until proven otherwise. ### Management Implications **Clinical Pearl:** Macula-on RRD (visual acuity 6/36 suggests macula-off) requires **urgent surgical intervention** — either pneumatic retinopexy, scleral buckle, or pars plana vitrectomy depending on break location and extent. 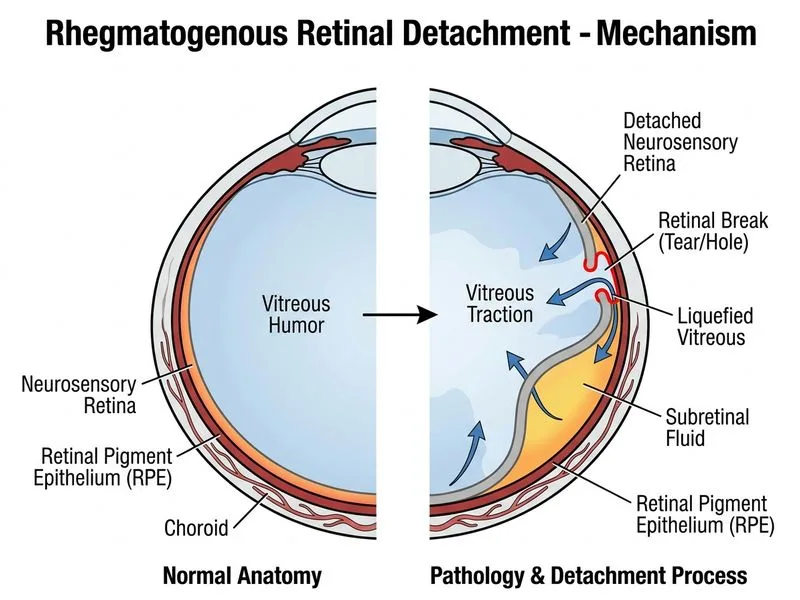
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.